Recognizing that your body requires more time to bounce back from stress, physical exertion, or illness empowers you to adjust your routines and protect your long-term health. While occasional fatigue remains a normal part of life, a persistent lag in recovery often points to underlying cellular changes and shifting hormonal baselines as you age. Ignoring these subtle biological shifts can lead to chronic inflammation, recurring injuries, and deep physiological burnout. By tuning into the silent signals your body broadcasts—from lingering muscle soreness to disrupted sleep architectures—you can proactively intervene and support your system. Understanding this natural evolution allows you to optimize your nutrition, refine your movement strategies, and seek appropriate medical guidance before minor setbacks transform into major physiological barriers.
The Biological Mechanics of Shifting Recovery Timelines
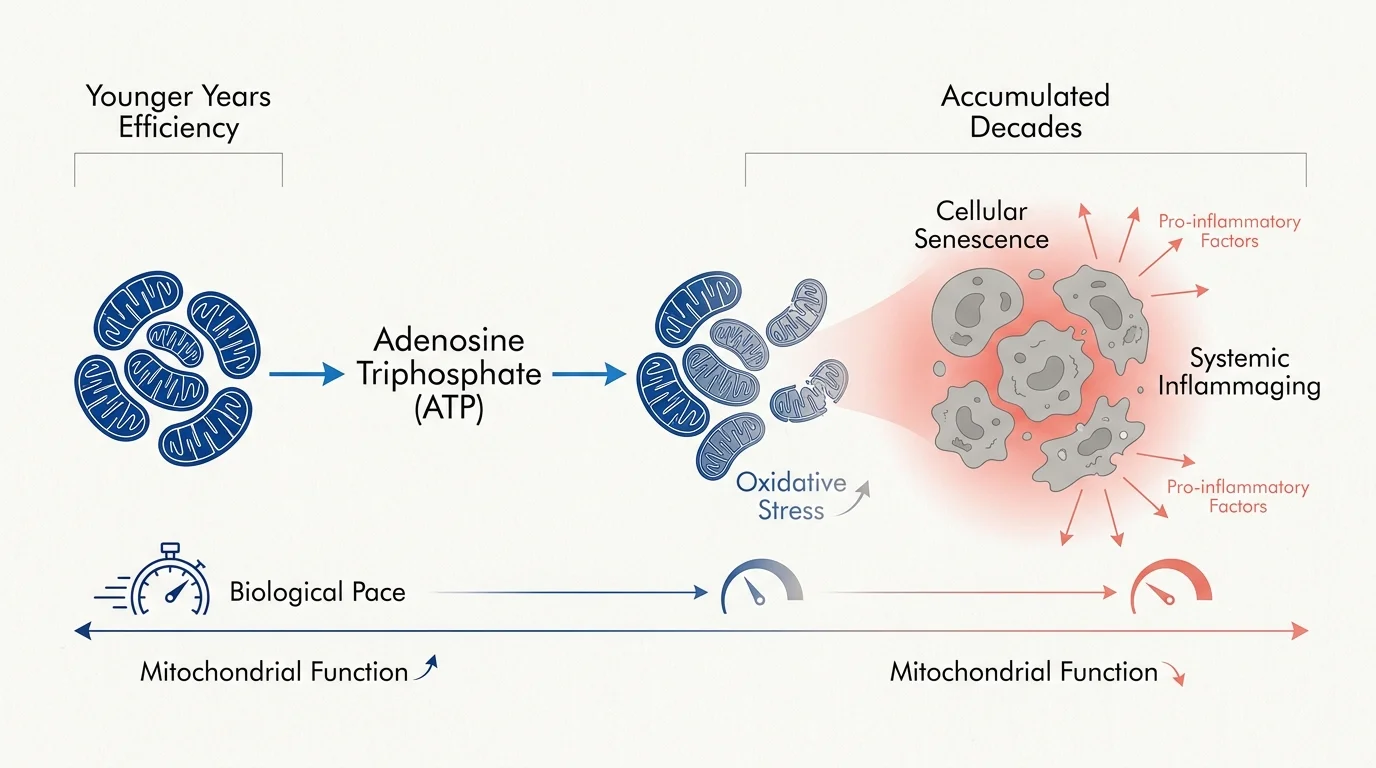
Your body operates as a highly efficient regenerative machine during your younger years; however, this efficiency subtly declines as you accumulate decades. Cellular senescence—a process where aging cells stop dividing but refuse to die—contributes to a low-level, systemic state of inflammation often referred to in clinical circles as inflammaging. This steady hum of inflammation diverts valuable energy away from tissue repair and immune defense, forcing your system to work significantly harder to achieve baseline recovery. Researchers studying the aging body frequently note that mitochondrial function naturally diminishes over time, leading to reduced production of adenosine triphosphate, the primary energy currency of your cells.
Understanding these mechanisms shifts the narrative from frustration to empowerment. Data compiled by the National Institute on Aging emphasizes that lifestyle modifications drastically influence how your cells manage oxidative stress and repair damaged DNA. You cannot halt the chronological clock, but you possess immense agency over your biological pace. By paying close attention to how your body responds to stressors, you can implement targeted behavioral changes that directly support mitochondrial health, lower inflammatory markers, and restore a robust recovery timeline.
8 Silent Signs Your Body Is Recovering More Slowly

1. Prolonged Muscle Soreness After Routine Activities
Experiencing delayed onset muscle soreness after pushing your limits is expected, yet feeling debilitating stiffness for several days after a standard workout signals a delayed repair process. When muscle fibers sustain micro-tears during exertion, your body triggers an inflammatory response to clear cellular debris and synthesize new proteins. If this localized inflammation lingers for three or four days instead of the usual 48 hours, your circulatory system and protein synthesis pathways are likely struggling to keep pace. Monitoring how long it takes your legs to feel fresh after a brisk walk or a familiar weightlifting session provides a clear metric of your current recovery capacity.
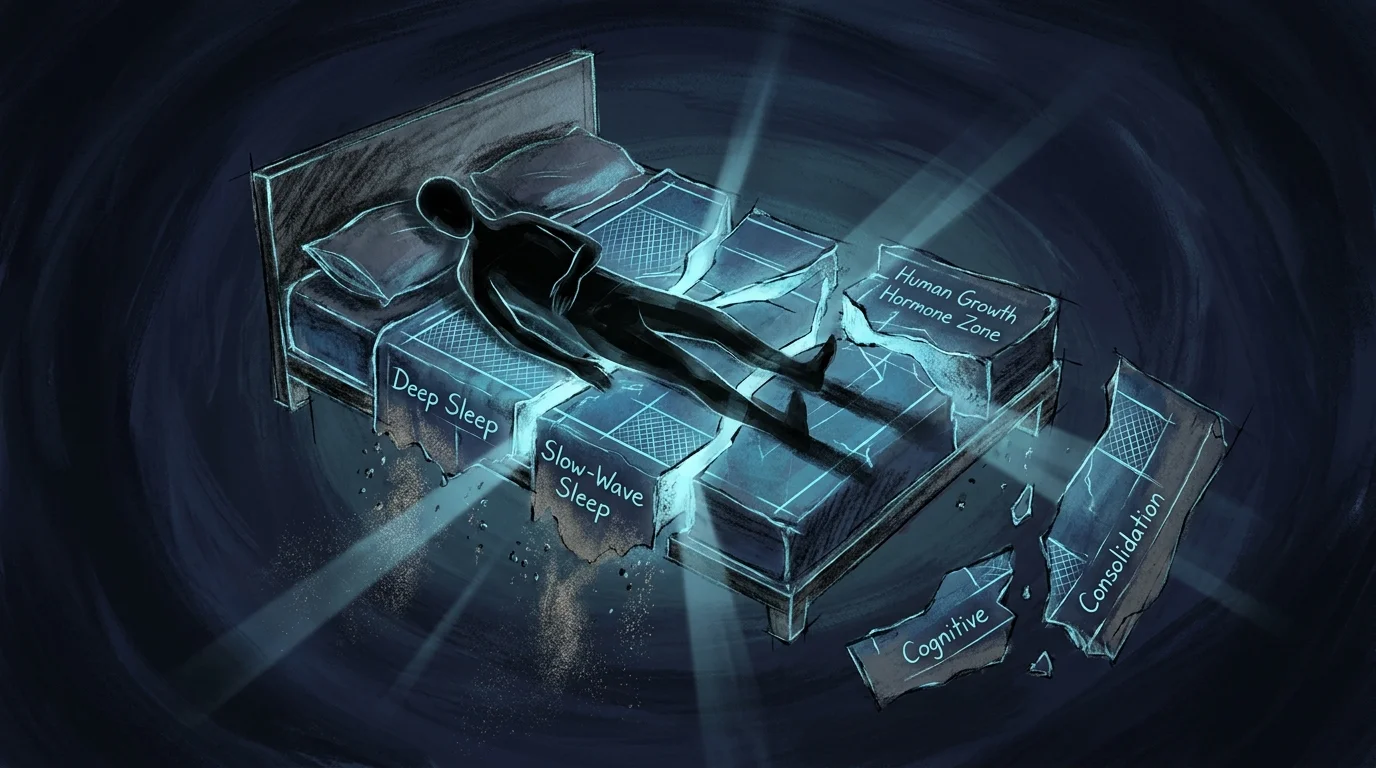
2. Shifting Sleep Architectures and Unrefreshing Rest
You might log eight hours in bed, but if you consistently wake up feeling as though you barely slept, your sleep architecture is likely fracturing. Deep, slow-wave sleep serves as the critical window when your pituitary gland releases human growth hormone, a vital component for tissue repair and cognitive consolidation. As recovery mechanisms slow down, pain, elevated cortisol, or minor metabolic disruptions easily interrupt these deep sleep cycles. You find yourself spending more time in lighter sleep stages, meaning your brain and muscles never receive the profound restorative maintenance they require to function optimally the following day.
3. Lingering Brain Fog After High-Stress Events
Physical exertion is not the only stressor that demands significant recovery time; emotional and cognitive hurdles exact a heavy toll on your system. The human brain consumes roughly twenty percent of your body’s energy reserves, and navigating intense deadlines, emotional conflicts, or complex problem-solving depletes these resources rapidly. If you notice that you feel mentally sluggish, easily distracted, or unusually forgetful for days after a stressful event resolves, your central nervous system is signaling a deficit. This prolonged brain fog indicates that your neurochemical balance and systemic energy reserves are taking much longer to replenish than they previously did.
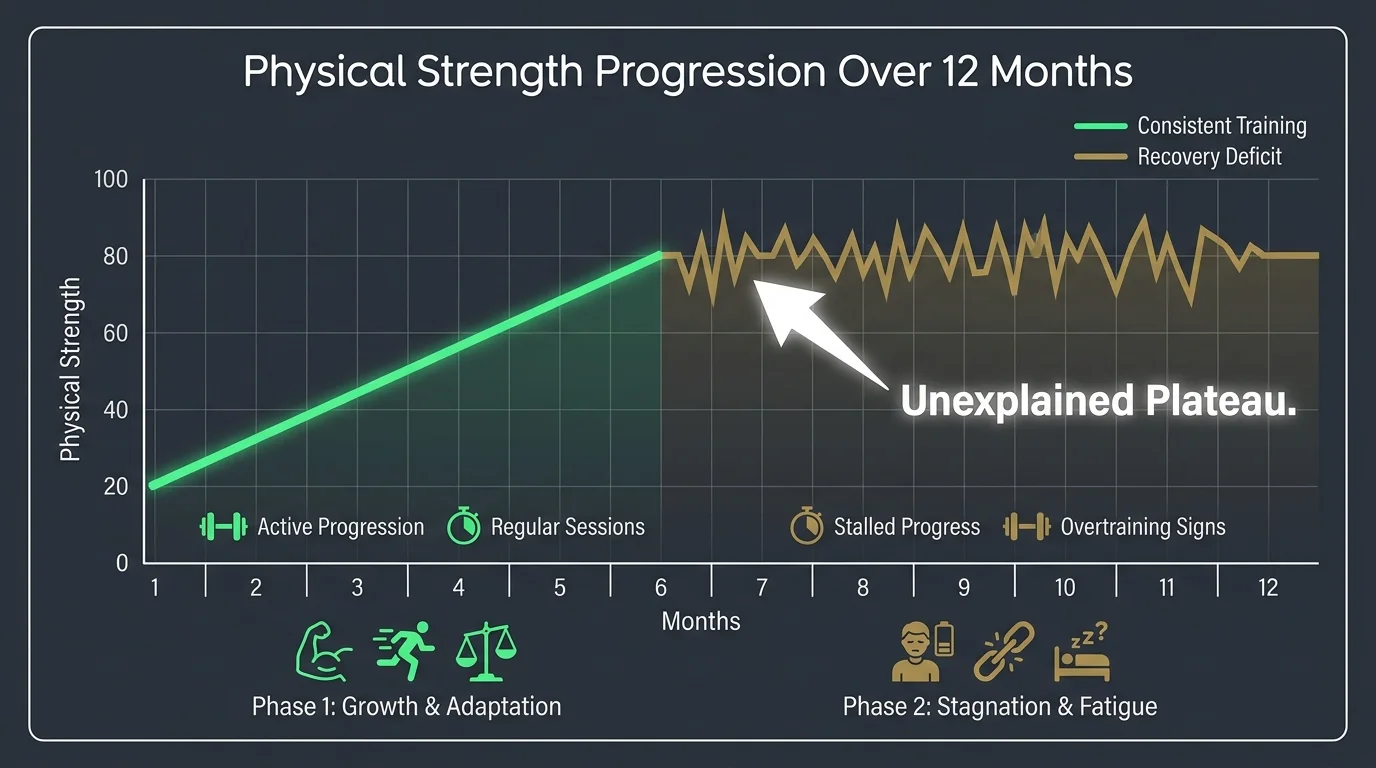
4. Unexplained Plateaus in Physical Strength
Consistent effort usually yields consistent, albeit gradual, progress in physical strength and endurance. Hitting a sudden, unyielding wall where you can no longer increase your weights, run your usual distance, or hold a yoga pose without trembling suggests that your muscles are not recovering adequately between sessions. This stagnation often acts as a precursor to overtraining syndrome. When your muscular breakdown outpaces your nutritional and physiological repair processes, your body halts adaptation altogether to conserve energy and prevent severe injury. Recognizing this plateau allows you to intervene before a significant physical setback occurs.

5. Increased Susceptibility to Minor Infections
Your immune system and your physical recovery pathways share the same energy pools and physiological resources. When your body struggles to repair tissue damage or clear systemic inflammation, immune surveillance naturally weakens. You might find yourself catching every mild cold that circulates through your office, or you might notice that a minor scratch takes an unusually long time to heal completely. The World Health Organization notes that immune function naturally declines over time—a phenomenon called immunosenescence—but an abrupt increase in minor illnesses often highlights an acute recovery deficit requiring immediate lifestyle adjustments.

6. Joint Stiffness That Defies Your Warm-Up Routine
Waking up with stiff joints is common, particularly in cooler environments, but this stiffness should dissipate after ten or fifteen minutes of gentle movement. If your knees, hips, or shoulders remain profoundly rigid and achy even after a thorough warm-up, your joint capsules are likely lacking adequate synovial fluid or struggling to clear localized inflammation. Cartilage does not possess its own direct blood supply; it relies entirely on movement to pump nutrients in and push waste products out. Persistent stiffness signals that this fluid exchange process is operating at a deficit, leaving joint tissues vulnerable to accelerated wear.

7. Delayed Heart Rate Normalization Post-Exertion
A healthy, resilient cardiovascular system ramps up your heart rate efficiently during exercise and brings it back down to baseline swiftly once you stop moving. Tracking your heart rate recovery—the speed at which your pulse drops in the first two minutes after stopping intense activity—provides excellent insight into your autonomic nervous system. If your heart continues to race long after you have finished a jog or climbed a steep flight of stairs, your sympathetic nervous system is trapped in a state of hyperarousal. This delayed normalization indicates your body is struggling to toggle back into the parasympathetic “rest and digest” mode necessary for healing.

8. Persistent Mood Fluctuations and Irritability
Your emotional resilience remains deeply intertwined with your physiological recovery status. When your body works overtime to clear metabolic waste and repair tissues, it often sustains elevated levels of stress hormones like cortisol and adrenaline. This chronic hormonal elevation keeps you on edge, leading to a notably shorter temper, sudden bouts of weepiness, or a pervasive sense of apathy toward activities you usually enjoy. Recognizing unexplained irritability as a biological cry for rest, rather than a personal character flaw, allows you to address the root physical exhaustion driving the mood shifts.

Foundational Strategy Pillars for Better Resilience

Optimizing Nutrition for Cellular Repair
Your cells literally rebuild themselves from the raw materials you consume on a daily basis. To accelerate sluggish recovery, you must prioritize high-quality protein, which supplies the essential amino acids required to mend micro-tears in your muscle tissue. Clinical insights from the Academy of Nutrition and Dietetics highlight the importance of spreading protein intake evenly across your meals to maximize muscle protein synthesis. Beyond macronutrients, you need a robust array of antioxidants derived from vibrant, colorful vegetables and omega-3 fatty acids from fish or flaxseeds to actively suppress the systemic inflammation that delays cellular healing. Hydration also remains non-negotiable; water facilitates the efficient transport of these vital nutrients deep into your tissues.

Modifying Movement to Prioritize Consistency Over Intensity
Pushing through exhaustion generally backfires when your biological recovery systems are already lagging. Instead of grinding through high-intensity intervals every day, you must weave active recovery strategies directly into your weekly schedule. Gentle movements—such as restorative yoga, swimming, or brisk walking in nature—stimulate beneficial blood flow without imposing significant mechanical stress on your joints and nervous system. This approach flushes metabolic waste from tired muscles while keeping your joints lubricated. Scaling back the intensity of your workouts does not signify a loss of fitness; it demonstrates a sophisticated understanding of how to train intelligently within your current physiological limits.

Cultivating a Mindset Geared Toward Restoration
Chronic mental stress actively sabotages physical healing by flooding your bloodstream with cortisol, which inhibits protein synthesis and disrupts restorative sleep cycles. To enhance your recovery, you must carve out dedicated periods of psychological unwinding. Techniques such as diaphragmatic breathing, structured meditation, or even simply disengaging from digital screens an hour before bed can dramatically shift your nervous system into a parasympathetic state. You must treat this mental decompression with the exact same reverence and scheduling priority that you apply to your physical workouts or professional obligations.

Integrating Proactive Medical Care
Sometimes, delayed recovery points to underlying issues that require clinical intervention, such as thyroid dysfunction, severe vitamin D deficiencies, or emerging autoimmune conditions. Working directly with healthcare professionals to run comprehensive blood panels removes the guesswork from your wellness strategy. By examining biomarkers related to inflammation, hormone balances, and nutrient statuses, you and your physician can craft a highly personalized recovery protocol. Acknowledge that social determinants—including your access to fresh food and safe recreational spaces—impact these outcomes, and communicate openly with your providers about any systemic barriers you face so they can tailor realistic, actionable advice.

Real Voices on Navigating Age and Recovery
Listening to those who successfully navigate these physiological shifts offers immense practical value. Sarah, a registered physical therapist who works extensively with aging populations, emphasizes the importance of honoring the body’s changing rhythms. She frequently reminds her patients that attempting to replicate the workout routines of their twenties during their fifties often leads to disaster. Instead, she advocates for a phased approach to fitness, where every intense effort is immediately followed by planned, deliberate rest.
Similarly, Marcus, a clinical dietitian focusing on senior health, notes that many of his clients drastically underestimate their caloric and nutritional needs as they age. He observes that older adults often restrict their food intake out of a fear of weight gain, inadvertently starving their bodies of the precise nutrients required to repair tissue damage and fight off daily fatigue. By shifting the conversation from restriction to nourishment, he helps his clients reclaim their energy and drastically shorten their recovery timelines.
Frequently Asked Questions
How do I know if my delayed recovery requires a doctor visit?
You should consult a physician if your fatigue feels profoundly debilitating, disrupts your ability to complete normal daily tasks, or is accompanied by unexplained pain, dizziness, or sudden weight changes. While minor extensions in recovery time are a normal part of aging, a sudden, drastic drop in your physical resilience strongly indicates that an underlying medical issue—such as a metabolic disorder or clinical deficiency—requires professional diagnosis and targeted treatment.
Can I speed up recovery with specific supplements?
While certain supplements like tart cherry juice, magnesium, and omega-3 fatty acids demonstrate solid efficacy in reducing inflammation and supporting muscle repair, they cannot replace the foundational pillars of sleep, proper hydration, and whole-food nutrition. You should view supplements strictly as tools to bridge minor dietary gaps rather than primary solutions. Always discuss new supplementation with your healthcare provider, as many over-the-counter products interact negatively with prescribed medications or underlying conditions.
Does slowing down mean I have to stop intense exercise completely?
Absolutely not. Incorporating vigorous activity remains crucial for maintaining cardiovascular health, bone density, and metabolic efficiency as you age. The required adjustment lies in your scheduling and frequency rather than abandoning intensity altogether. If your body requires three days to recover from a heavy lifting session instead of one, you simply space out those intense efforts and fill the intermediate days with mobility work, walking, or gentle stretching to support the healing process.
Why does mental stress impact my physical recovery so severely?
Your brain and your body do not operate in isolated silos; they share a unified neuroendocrine system. When you perceive a stressful situation, your adrenal glands release stress hormones that prepare your body for immediate physical action. If this stress becomes chronic, your system remains on high alert, diverting massive amounts of energy and resources away from long-term projects like immune function, digestion, and muscular repair. Consequently, unresolved psychological tension directly translates into persistent physical exhaustion.
Your Next Step Forward
Navigating a shifting physiological baseline requires immense patience and self-compassion, but acknowledging these changes is the first powerful step toward sustainable wellness. Start by observing your body without judgment. Choose one specific area of your life this week—perhaps prioritizing an extra hour of sleep or adding a dedicated stretching routine after your daily walk—and commit to executing it consistently. Reflect on how your energy levels shift when you proactively support your system rather than forcing it to perform on empty reserves. By tuning in and responding to your body’s subtle signals, you lay a resilient foundation for long-term health and vibrant longevity.










Leave a Reply