Misinterpreting your body’s distress signals after a meal often leads to unnecessary dietary restrictions and lingering anxiety about food. Understanding the precise difference between a true immune-system food allergy and a digestive intolerance empowers you to seek the right treatment and reclaim your nutritional freedom. While genuine food allergies trigger rapid, potentially life-threatening immune responses, many uncomfortable post-meal symptoms actually stem from metabolic sensitivities, enzyme deficiencies, or functional gastrointestinal disorders. By identifying the true root cause of your discomfort, you can implement targeted lifestyle adjustments rather than completely eliminating your favorite meals. Learning to translate your physical symptoms accurately ensures you receive appropriate medical care while maintaining a balanced, inclusive approach to your everyday nutrition.
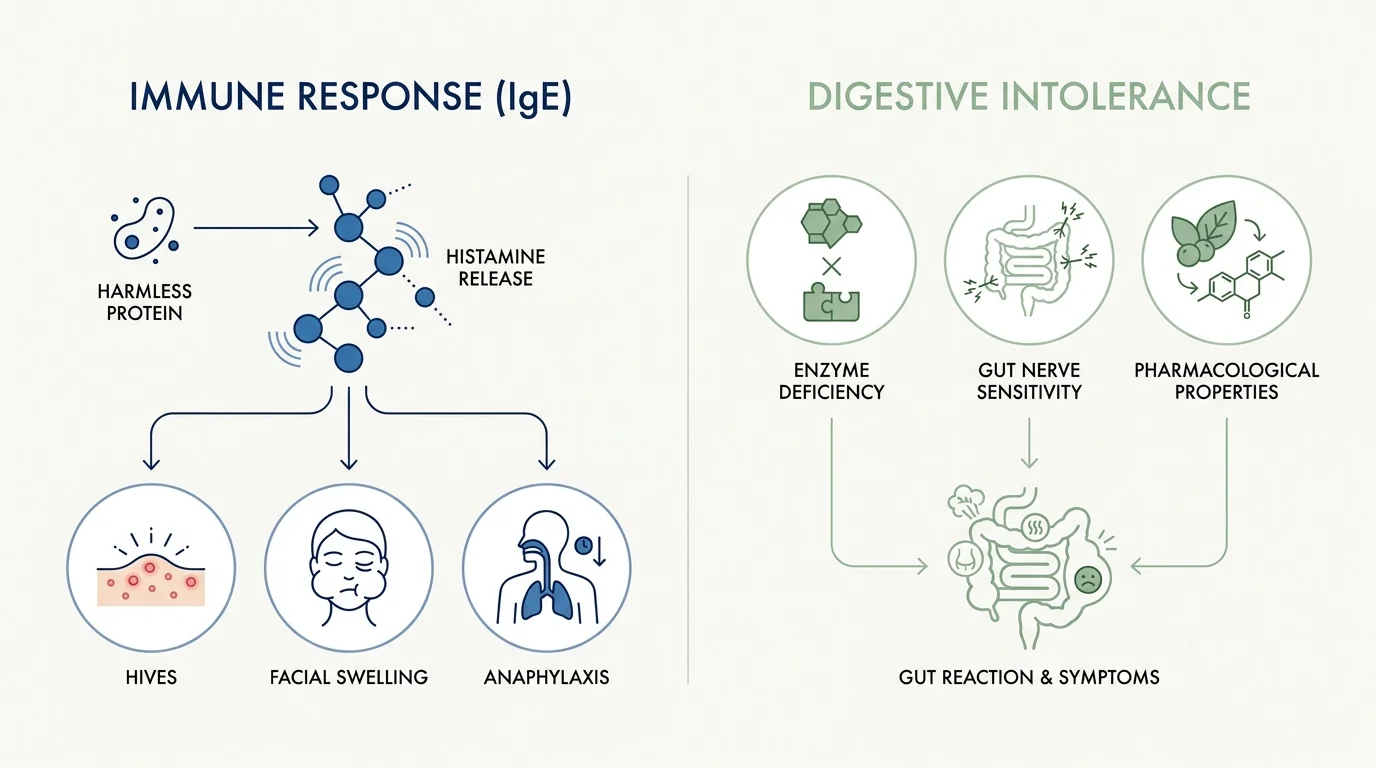
The Science Snapshot: Immune Response Versus Intolerance
When you eat something that disagrees with you, the immediate assumption is often an allergy; however, clinical data paints a distinctly different picture. The Centers for Disease Control and Prevention notes that while millions of Americans experience adverse reactions to food, true immunoglobulin E (IgE) mediated food allergies affect a much smaller percentage of the adult population. A legitimate food allergy involves your immune system treating a harmless protein as a dangerous invader, launching a massive antibody attack that releases a flood of histamine. This chemical cascade causes rapid, systemic reactions like hives, facial swelling, and anaphylaxis.
Intolerances and functional sensitivities largely originate in your digestive tract or metabolic pathways rather than your immune system. They occur when your body lacks the specific enzymes needed to break down certain compounds, when gut nerve endings become hypersensitive, or when pharmacological properties of the food alter your heart rate. Relying on accurate medical diagnostics rather than self-imposed elimination diets protects you from nutritional deficiencies and ensures you address the actual physiological mechanism behind your specific symptoms.

Reaction 1: The Abdominal Bloat Of Lactose Intolerance
Drinking a glass of milk and subsequently experiencing severe abdominal cramping and bloating frequently leads people to believe they have a dairy allergy. In reality, you are likely dealing with lactose intolerance—a structural lack of lactase, the enzyme required to digest the primary sugar found in milk. Without adequate lactase, undigested lactose moves into your colon, where resident bacteria ferment it, producing significant amounts of gas and drawing excess water into your bowels.
Addressing this digestive challenge requires targeted nutritional strategies rather than panic over an immune response. The National Institute of Diabetes and Digestive and Kidney Diseases suggests utilizing over-the-counter lactase enzyme supplements right before consuming dairy to aid digestion. Additionally, you can explore calcium-fortified plant milks, which offer cost-effective and highly accessible alternatives for those who prefer to bypass lactose entirely while maintaining optimal bone health.

Reaction 2: The Flushing And Headaches Of Histamine Intolerance
Consuming aged cheeses, cured meats, or a glass of red wine can sometimes trigger facial flushing, sudden headaches, and a runny nose. Because these symptoms mirror the exact effects of an allergic histamine release, they frequently result in misdiagnoses. The culprit here is usually histamine intolerance, a metabolic condition where your body fails to produce enough diamine oxidase (DAO), the enzyme responsible for breaking down histamine found naturally in aged and fermented foods.
When you consume histamine-rich foods without sufficient DAO, the chemical accumulates in your bloodstream, dilating blood vessels and sparking allergy-like symptoms. Managing this condition involves a strategic approach to food sourcing. Prioritize fresh meats and produce over preserved, canned, or highly fermented options, as histamine levels increase significantly during the aging process. Working with a registered dietitian can help you establish a nutrient-dense baseline diet that naturally keeps your histamine bucket from overflowing.

Reaction 3: Severe Gut Distress From FODMAP Sensitivities
Many individuals convinced they have a severe allergy to onions, garlic, or wheat are actually experiencing the hallmark symptoms of Irritable Bowel Syndrome (IBS) triggered by fermentable carbohydrates known as FODMAPs. When you consume these specific short-chain carbohydrates, they draw excess liquid into the intestine and rapidly ferment, producing severe gas, distension, and erratic bowel movements.
Because the gut and brain are intimately connected via the vagus nerve, psychological stress drastically amplifies these digestive symptoms. To find relief, you must merge nutritional changes with mindset and movement practices. The American College of Gastroenterology outlines the importance of working with a professional to implement a temporary low-FODMAP protocol to identify your specific triggers. Coupling this dietary investigation with daily stress-reduction techniques—such as deep diaphragmatic breathing and routine light cardiovascular exercise—calms the nervous system and significantly reduces gut hypersensitivity.
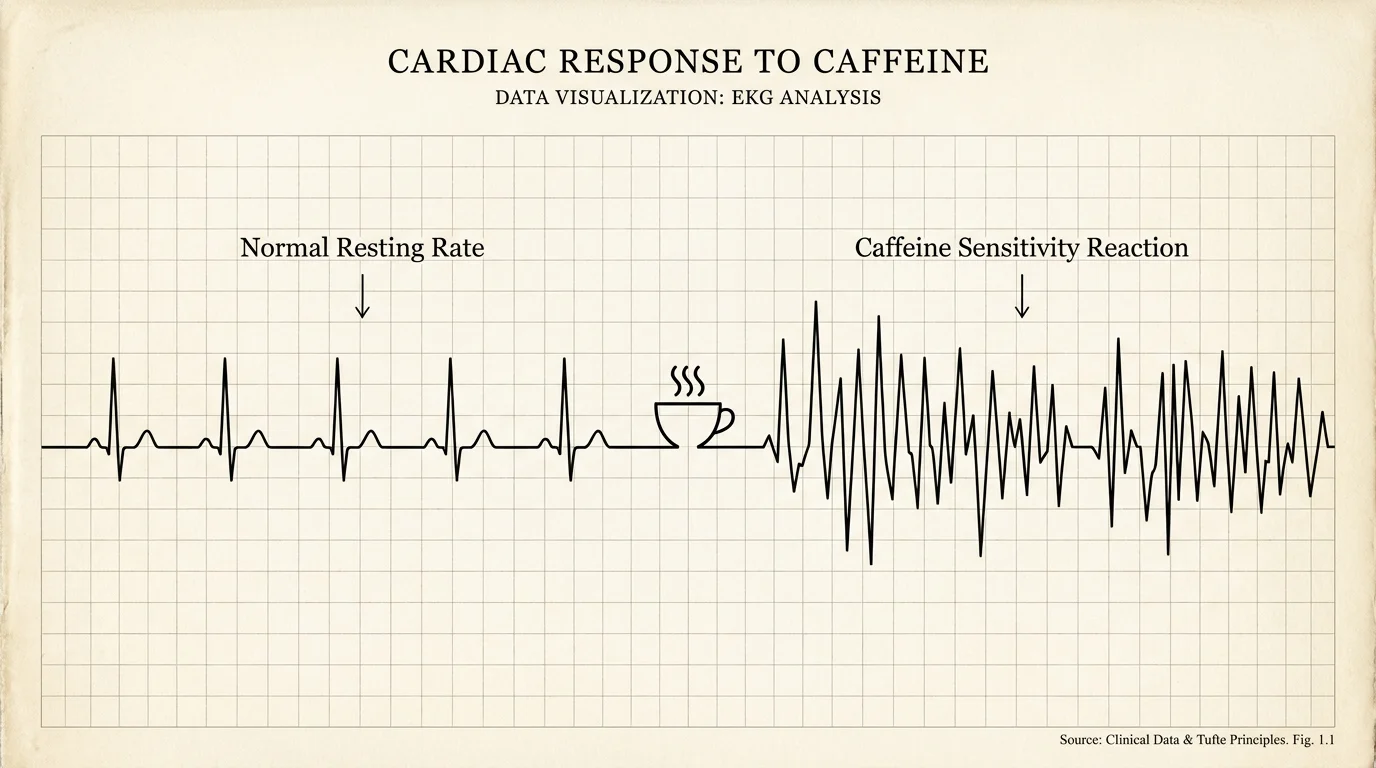
Reaction 4: The Heart Palpitations Of Caffeine Sensitivity
Experiencing a racing heart, trembling hands, and a sudden wave of anxiety after eating dark chocolate or drinking an espresso beverage often mimics the terrifying onset of anaphylaxis. People frequently mistake this physiological arousal for an allergic reaction to the cocoa bean or the coffee plant. In truth, this response highlights a genetic variation in how your liver metabolizes caffeine, combined with a hypersensitive central nervous system.
When caffeine lingers in your system, it triggers the release of adrenaline, effectively shifting your body into a fight-or-flight state. To manage this intense reaction, you should closely audit your daily intake of hidden stimulants found in pre-workout powders, certain teas, and dark chocolate. Hydrating adequately and substituting highly caffeinated beverages with herbal alternatives protects your nervous system from unnecessary chemical stress and keeps your heart rate stable.

Reaction 5: Throat Tightness Caused By Acid Reflux
The sensation of your throat suddenly swelling shut is a classic warning sign of a severe allergic emergency, prompting understandable alarm. Yet, countless individuals who rush to urgent care with throat tightness after a spicy, heavy, or late-night meal are actually suffering from severe gastroesophageal reflux disease (GERD). When highly acidic stomach contents wash back up into your esophagus, the sensitive mucosal lining becomes irritated, triggering localized esophageal spasms.
These spasms create a gripping, restrictive feeling in the chest and throat that perfectly simulates the respiratory distress of an allergy. Preventing this frightening symptom requires you to manipulate both movement and meal timing. Taking a gentle twenty-minute walk after eating leverages gravity and movement to speed up gastric emptying, preventing acid from pooling. You must also proactively avoid lying down or performing intense core exercises for at least two hours post-meal. If this sensation occurs frequently, consult a medical professional for structural assessments and targeted therapies.

Reaction 6: The Sudden Illness Of Food Poisoning
Violent vomiting, severe stomach cramps, and explosive diarrhea occurring just hours after eating a new food often lead individuals to declare a sudden, severe allergy to whatever they just consumed. However, these acute gastrointestinal explosions are usually the result of foodborne illness caused by bacterial toxins. According to the World Health Organization, pathogens like Staphylococcus aureus can produce heat-stable toxins that rapidly irritate the stomach lining.
Unlike an allergy, which requires your immune system to build antibodies over prior exposures, food poisoning strikes anyone who ingests the contaminated item. The symptoms represent your body’s emergency evacuation protocol to expel harmful bacteria. Rather than permanently banning the suspected food from your life, focus on rigorous food safety practices. Verify internal cooking temperatures with a reliable meat thermometer and ensure prompt refrigeration of leftovers to prevent bacterial proliferation.

Reaction 7: Wheezing And Flushing From Sulfite Sensitivities
Experiencing sudden wheezing, chest tightness, or a warm facial flush after eating dried apricots or drinking a glass of white wine can be deeply concerning. While these respiratory and dermatological symptoms strongly resemble an IgE-mediated allergy, they frequently point to a specific sensitivity to sulfites. Sulfites are naturally occurring compounds and chemical additives used extensively to preserve the color and extend the shelf life of various foods and beverages.
People with underlying asthma are particularly vulnerable to sulfite reactions, as the gas released during the digestion of these compounds irritates the airway passages. Navigating a sulfite sensitivity requires diligent label reading rather than carrying an epinephrine auto-injector. Check ingredient lists for terms like sulfur dioxide, potassium bisulfite, or sodium sulfite, and prioritize fresh, unpackaged fruits and vegetables to naturally minimize your exposure to these industrial preservatives.
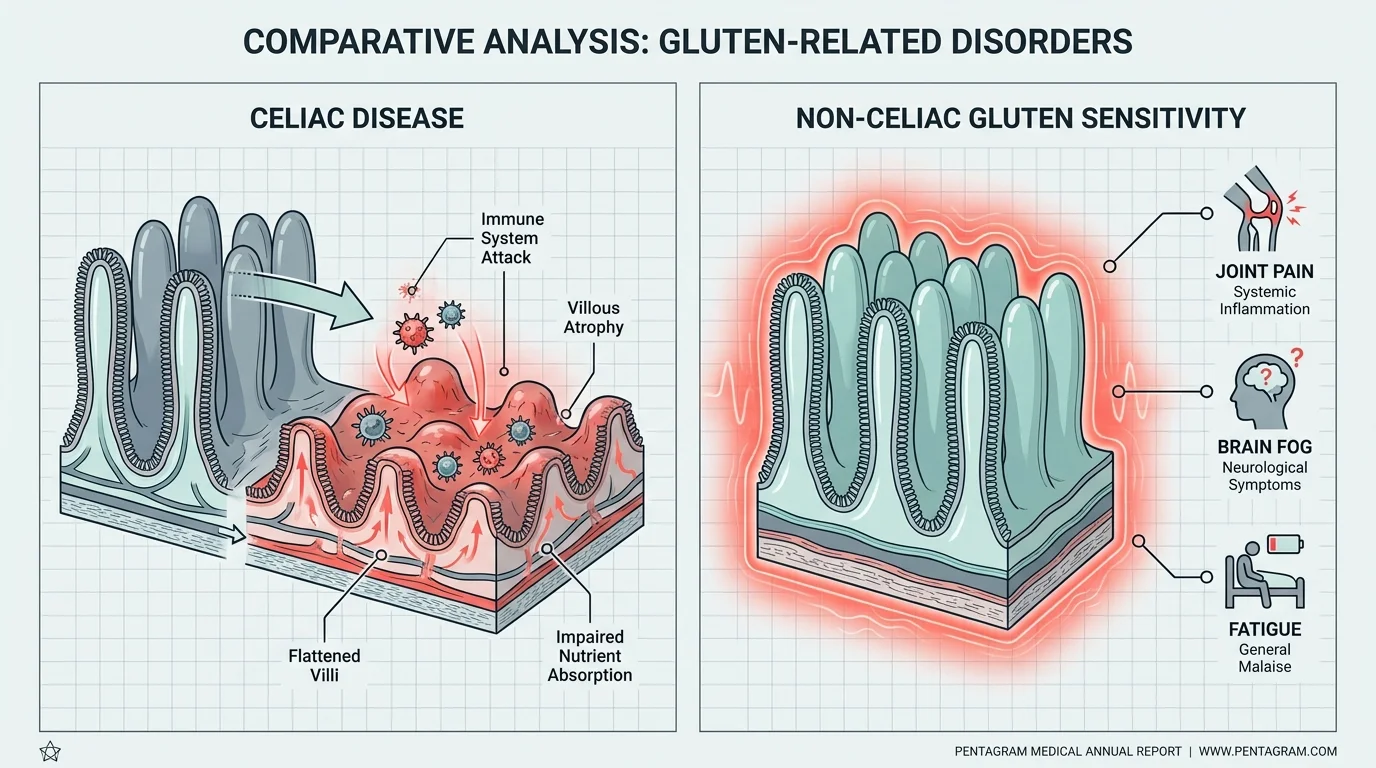
Reaction 8: Systemic Inflammation In Non-Celiac Gluten Sensitivity
Experiencing profound brain fog, persistent joint pain, and profound fatigue after consuming a bowl of pasta leads many to self-diagnose a severe wheat allergy. While true wheat allergies and autoimmune Celiac disease certainly exist, a growing portion of the population experiences Non-Celiac Gluten Sensitivity (NCGS). This distinct condition generates systemic inflammation and digestive distress without the measurable IgE antibodies of an allergy or the intestinal damage characteristic of Celiac disease.
Because the symptoms of NCGS are wide-ranging and neurological, it is critical to pursue formal medical testing before altering your diet. Eliminating gluten prior to a blood test can result in a false negative for Celiac disease, obscuring your true medical picture. Always collaborate with a gastroenterologist to rule out structural damage or autoimmune conditions before committing to a lifelong gluten-free lifestyle, ensuring you base your dietary protocols on accurate clinical data.

Real Voices: Insights From Clinical Practice
Listening to healthcare professionals underscores the hidden dangers of self-diagnosing food allergies based on generalized symptoms. Clinical dietitians and board-certified allergists routinely observe patients who have restricted their diets to a dangerously narrow variety of foods out of fear, ultimately resulting in severe malnutrition and elevated psychological distress. As one leading allergist recently noted during a clinical symposium, eliminating entire food groups without laboratory confirmation starves your gut microbiome of necessary diversity and drastically lowers your overall quality of life.
Medical providers strongly advocate for equitable access to proper diagnostic testing. If visiting a specialized allergist feels financially out of reach, many community health centers and primary care clinics offer baseline screenings that can differentiate between an enzyme deficiency and an immune response. Reaching out to local resources ensures you do not have to navigate these frightening symptoms isolated and uninformed.
Frequently Asked Questions About Food Reactions
How can I accurately tell if my reaction is a true medical emergency?
Anaphylaxis, the most severe form of an allergic reaction, involves multiple organ systems and requires immediate emergency intervention. If your symptoms escalate rapidly to include trouble breathing, a distinct swelling of the lips and tongue, a sudden drop in blood pressure, or a feeling of impending doom, you must use an epinephrine auto-injector if prescribed and call emergency services. Digestive discomfort alone, no matter how severe the cramping, rarely constitutes a life-threatening anaphylactic event.
Can chronic stress make my food intolerances feel worse?
Absolutely; chronic psychological stress continuously activates your sympathetic nervous system, pulling vital blood flow away from your digestive tract. This physiological shift slows down gastric motility and drastically lowers your threshold for abdominal pain. By integrating daily mindfulness practices and prioritizing adequate sleep, you calm the vagus nerve, which significantly improves your body’s ability to tolerate fermentable carbohydrates and histamine-rich foods without generating severe symptoms.
Are the at-home food sensitivity tests advertised online actually accurate?
The majority of at-home kits measure Immunoglobulin G (IgG) antibodies. However, the American Academy of Allergy, Asthma & Immunology explicitly advises against using IgG testing to diagnose food allergies or sensitivities. The presence of IgG merely indicates that your body has been exposed to a food and has developed a normal, healthy tolerance to it. Relying on these unverified tests frequently leads to unnecessary anxiety and highly restrictive, unhealthy diets.
How does the timeline of symptoms differ between an allergy and an intolerance?
Timing provides a crucial clue when evaluating your bodily responses. A genuine IgE-mediated food allergy typically triggers a reaction within minutes to two hours after ingestion, as the immune system mounts a rapid, aggressive defense. Conversely, food intolerances and sensitivities rely on the slower process of digestion and fermentation. It can take anywhere from a few hours to a couple of days for the offending food to reach the colon and produce the hallmark gas, bloating, and systemic fatigue.
Your Next Manageable Step Toward Clarity
Deciphering the nuanced language of your digestive and immune systems does not have to be an overwhelming endeavor. Start by implementing a simple, objective symptom log. For the next two weeks, record what you eat, the specific symptoms you experience, and exactly how long after the meal those symptoms appear. Include notes on your daily stress levels and sleep quality, as these vastly influence digestive health. Take this detailed evidence to a qualified healthcare provider or registered dietitian. Armed with concrete data rather than generalized fear, you can formulate a precise, nourishing plan that honors your body’s unique metabolic needs while keeping your diet as expansive and joyful as possible.








Leave a Reply