Managing multiple health conditions often means taking a handful of pills every morning, but mixing certain prescription and over-the-counter medications creates severe health risks. You can protect your long-term wellbeing by identifying dangerous drug combinations and working with your doctor to adjust your routine. Millions of older adults unknowingly take interacting medications that cause dizziness, internal bleeding, or cognitive decline. Changes in how the aging body processes chemicals mean that a combination you tolerated a decade ago might suddenly become toxic. By reviewing your daily regimen and understanding the chemical interactions at play, you can prevent preventable hospitalizations and maintain your independence.
The Science Snapshot: Why Aging Changes Medication Metabolism
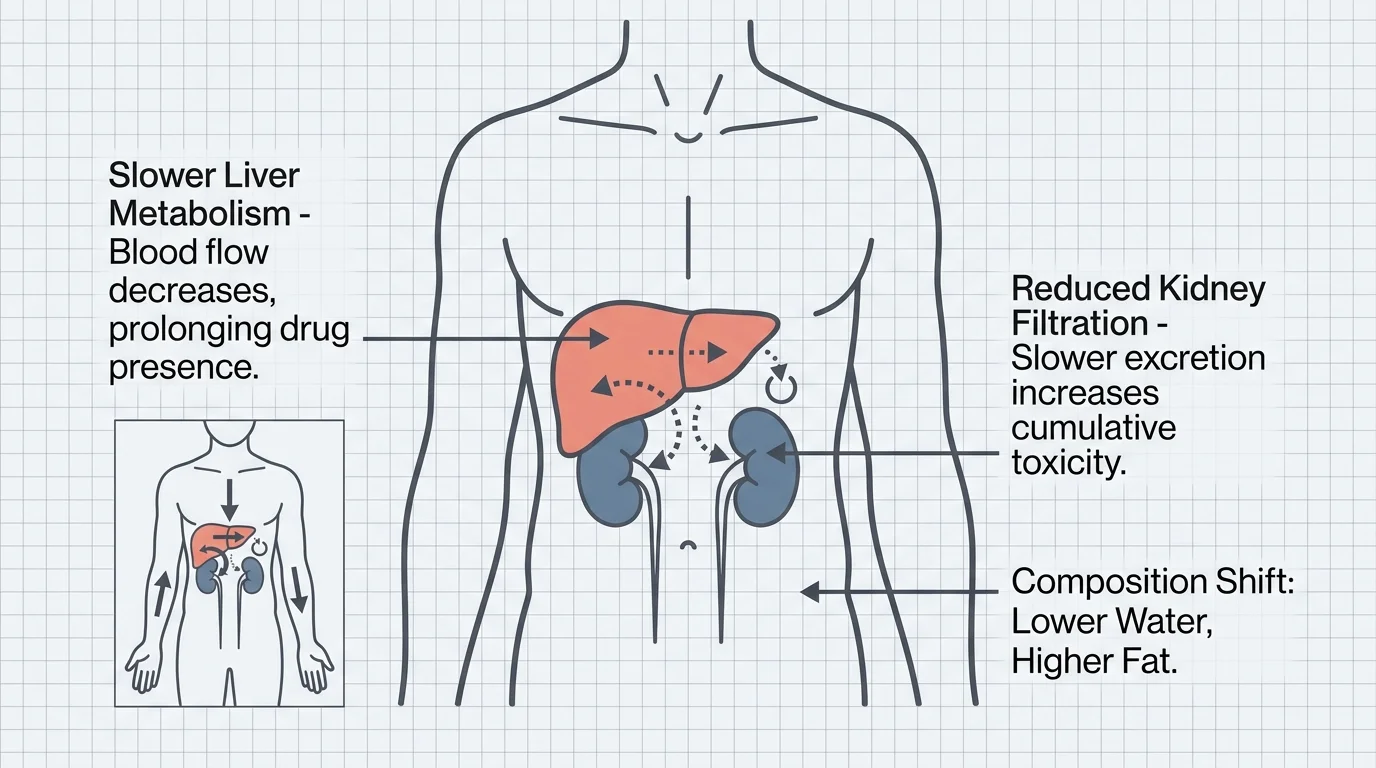
As you age, your body undergoes profound physiological changes that directly impact how you absorb, distribute, metabolize, and excrete medications. Pharmacologists refer to this biological process as pharmacokinetics, and it perfectly explains why a dose of medication that worked flawlessly in your fifties can cause debilitating side effects in your seventies. Your liver and kidneys serve as the primary filtration organs for clearing drugs from your system. Over time, blood flow to these vital organs naturally decreases, and they lose some of their functional reserve. Consequently, medications linger in your bloodstream significantly longer, drastically increasing your risk of cumulative toxicity.
Shifts in your physical body composition also play a major role in medication dynamics. Older adults typically experience a decrease in total body water and lean muscle mass, alongside a relative increase in body fat percentage. Water-soluble drugs become highly concentrated in your blood, while fat-soluble drugs accumulate deeply in fatty tissues, leading to an artificially prolonged drug half-life. Furthermore, seniors frequently experience polypharmacy—the concurrent use of five or more medications daily. According to the Centers for Disease Control and Prevention, older adults are disproportionately affected by adverse drug events, leading to thousands of preventable emergency room visits annually. Understanding these foundational biological realities empowers you to advocate for safer prescribing practices and holistic health interventions.
The 6 Dangerous Drug Combinations Seniors Must Watch For
When you combine medications without thoroughly evaluating their combined chemical effects, you risk triggering severe interactions that amplify unwanted side effects or completely neutralize the benefits of your treatments. The following six combinations represent some of the most common and hazardous medication pairings found in the medicine cabinets of older adults today.
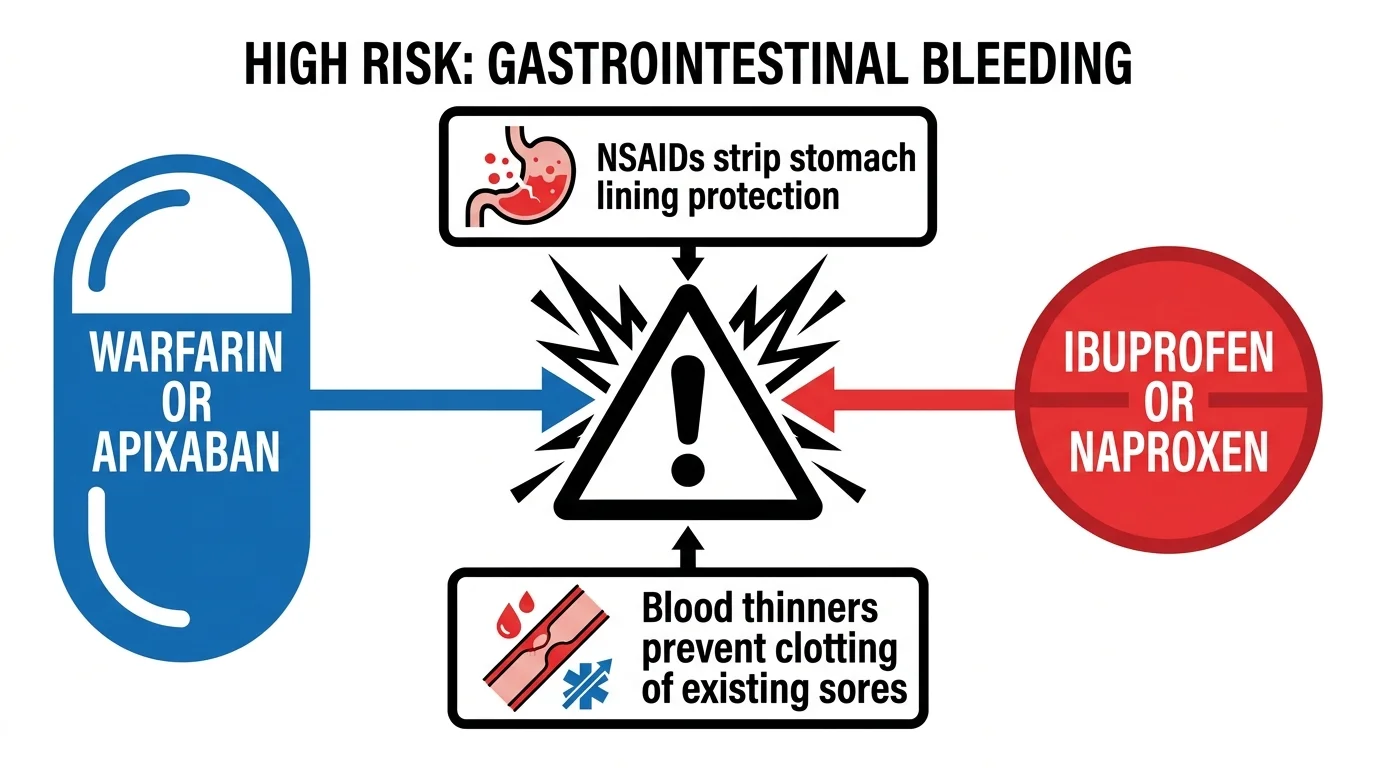
1. Blood Thinners and Nonsteroidal Anti-Inflammatory Drugs
Millions of seniors take daily anticoagulants, commonly known as blood thinners, to prevent strokes, heart attacks, and deep vein thrombosis. If you rely on medications like warfarin, apixaban, or rivaroxaban, you must exercise extreme caution when reaching for over-the-counter pain relievers. Nonsteroidal anti-inflammatory drugs, including ibuprofen and naproxen, also inherently inhibit blood clotting. More importantly, these anti-inflammatory drugs suppress the production of prostaglandins, which are protective chemicals that maintain the delicate mucosal lining of your stomach. When you mix these two categories of drugs, you strip away your stomach’s natural cellular defense while simultaneously preventing your blood from clotting. This exponentially increases your risk for life-threatening gastrointestinal bleeding. Even low-dose daily aspirin, when combined with another blood thinner and an over-the-counter painkiller, creates a highly dangerous environment for internal hemorrhaging. You should explore alternative pain management strategies with your physician, such as targeted physical therapy or acetaminophen, which generally avoids this specific bleeding risk.
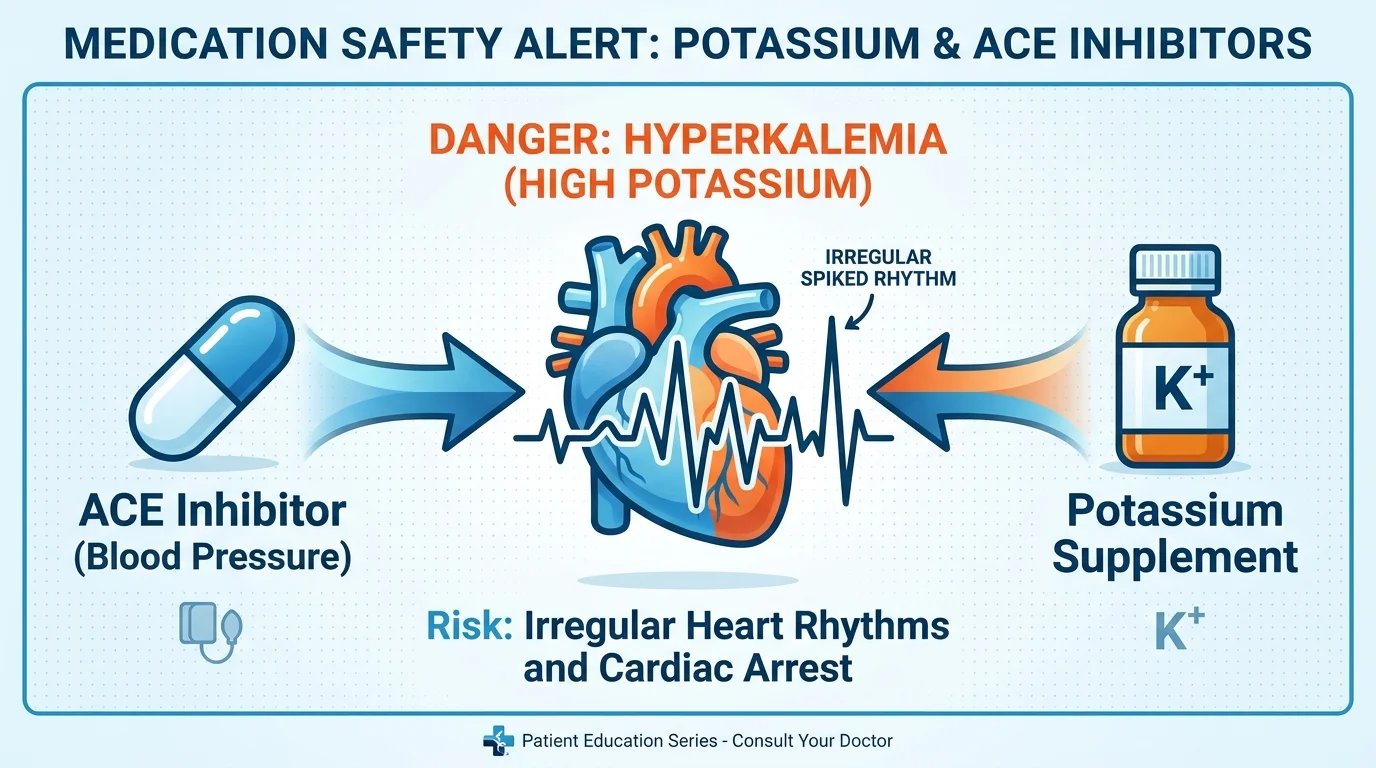
2. ACE Inhibitors and Potassium Supplements
Cardiovascular health requires careful, continuous management, and doctors frequently prescribe angiotensin-converting enzyme inhibitors—such as lisinopril or enalapril—to lower elevated blood pressure and support overall heart function. These medications naturally cause your kidneys to retain potassium rather than excreting it. While potassium remains vital for proper nerve transmission and muscle function, too much of it leads to a dangerous physiological condition called hyperkalemia. If you take a standalone potassium supplement or heavily consume artificial salt substitutes that contain potassium chloride while on an angiotensin-converting enzyme inhibitor, your potassium levels can spike to highly toxic levels. High potassium drastically disrupts the delicate electrical signals in your heart, potentially triggering dangerous arrhythmias, severe muscle weakness, or even sudden cardiac arrest. You must routinely check your electrolyte levels through blood tests if you take these blood pressure medications.

3. Statins and Macrolide Antibiotics
Cholesterol-lowering statins like atorvastatin and simvastatin rank among the most widely prescribed cardiovascular medications globally. However, these life-saving drugs rely heavily on specific liver enzymes—particularly the cytochrome P450 3A4 enzyme—for clearance from your body. When you develop a bacterial infection and receive a prescription for a macrolide antibiotic, such as clarithromycin or erythromycin, these powerful antibiotics severely inhibit the exact liver enzymes responsible for breaking down the statin. As a result, statin concentrations in your bloodstream can surge to toxic levels within mere days. This excessive concentration leads to severe, debilitating muscle pain and a rare but life-threatening condition called rhabdomyolysis. During rhabdomyolysis, rapid muscle breakdown releases proteins into your bloodstream that overwhelm your kidneys, potentially causing irreversible renal failure. You must actively inform your prescribing physician and pharmacist about your statin use whenever you receive a new antibiotic prescription.
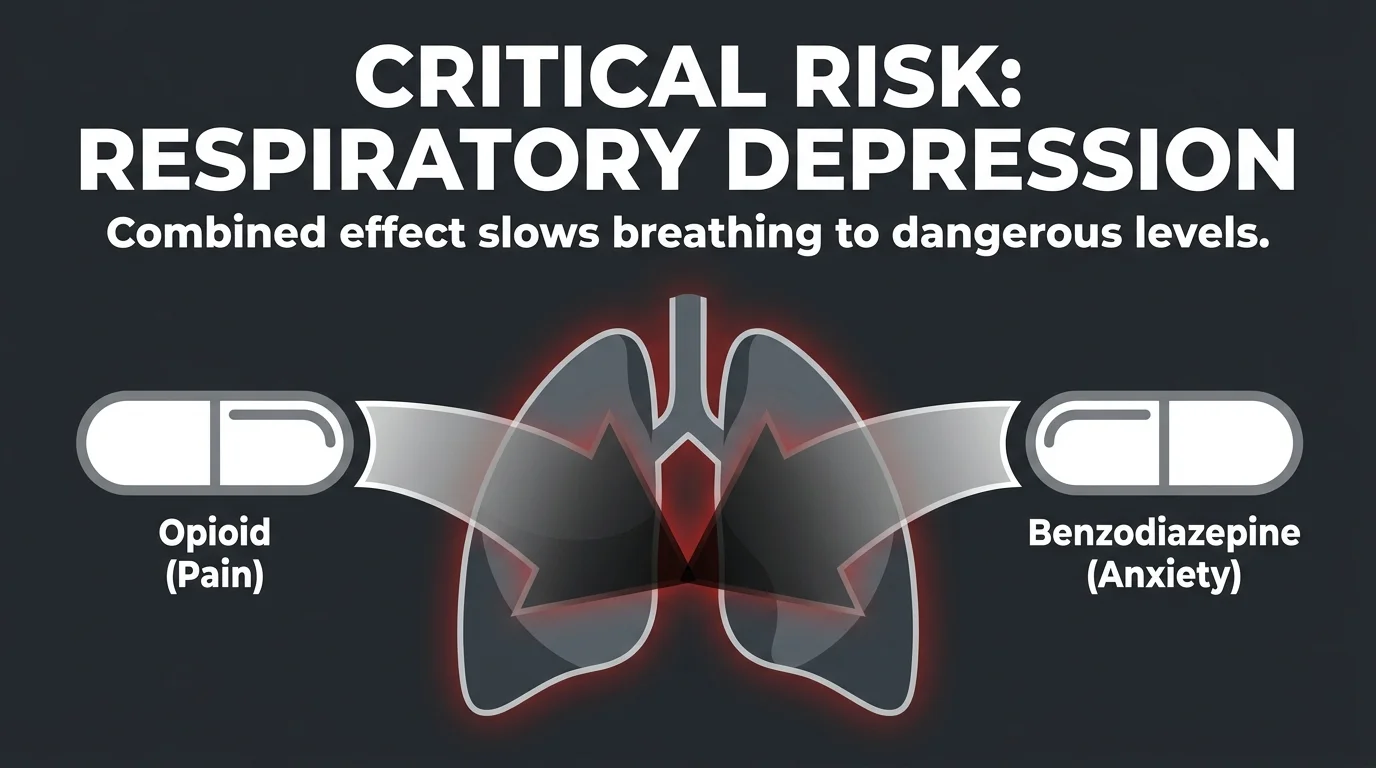
4. Opioids and Benzodiazepines
The simultaneous use of prescription opioids for severe pain and benzodiazepines for anxiety or sleep disorders creates a lethal chemical synergy. Medications like oxycodone, hydrocodone, or tramadol profoundly depress your central nervous system, slowing your breathing and heart rate. Benzodiazepines, such as alprazolam, diazepam, or lorazepam, exert a similarly suppressive effect on the brain’s GABA receptors. When combined, these drugs amplify each other’s effects exponentially, leading to profound sedation and severe respiratory depression. Older adults are incredibly sensitive to this specific combination, facing a dramatically heightened risk of fatal overdose, extreme cognitive confusion, and devastating physical falls. The National Institute on Drug Abuse explicitly warns against this dangerous pairing. If you currently take both medications, work closely with a comprehensive medical team to safely and gradually taper your dosages while introducing holistic therapies for pain and anxiety relief.
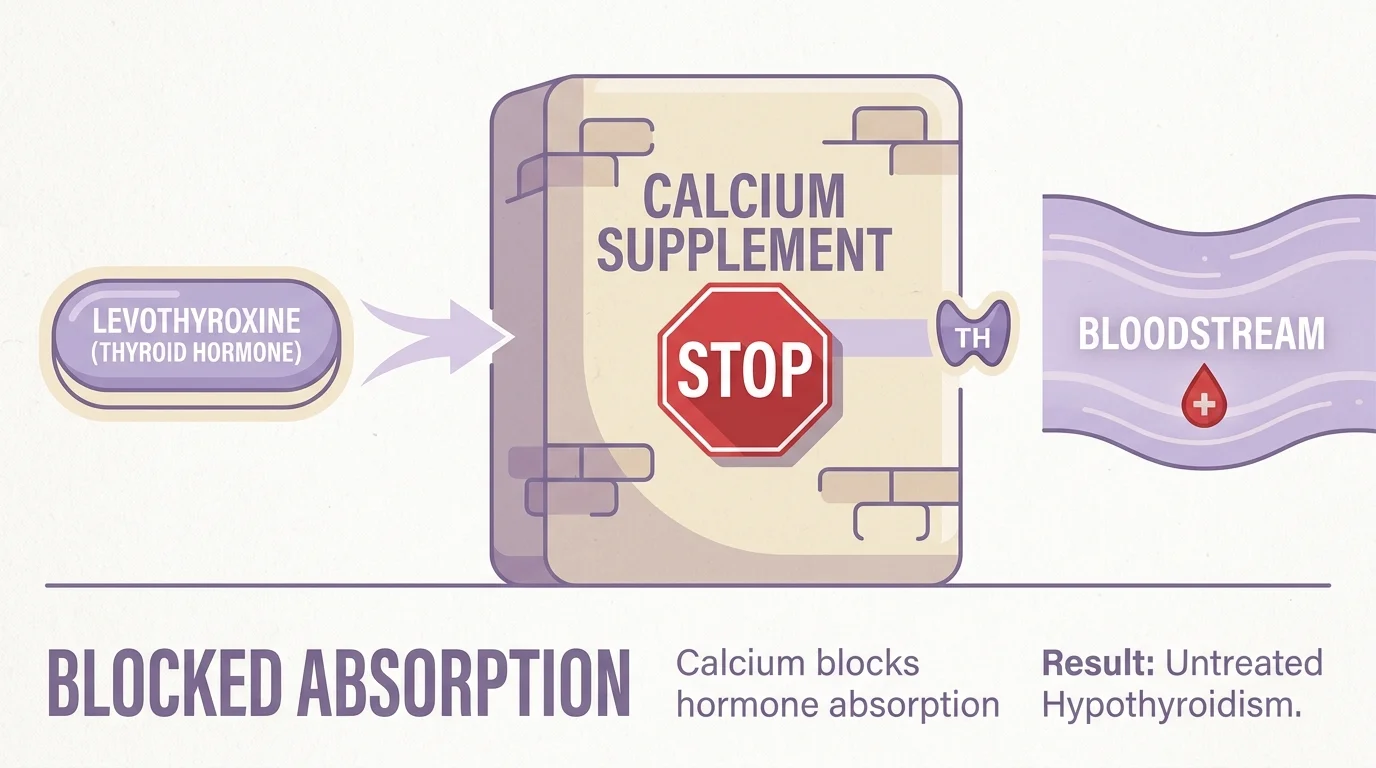
5. Calcium Supplements and Thyroid Hormones
Hypothyroidism affects a significantly large percentage of older adults, necessitating daily synthetic thyroid hormone replacement therapy like levothyroxine. Simultaneously, many seniors take daily calcium supplements to protect against osteoporosis, bone density loss, and fractures. While both treatments hold significant value for healthy aging, calcium carbonate directly binds to levothyroxine inside your digestive tract. This physical binding prevents your body from properly absorbing the essential thyroid hormone, rendering your vital prescription practically useless. The resulting severe drop in active thyroid levels causes profound physical fatigue, unexplained weight gain, clinical depression, and cognitive sluggishness. To successfully manage both conditions simultaneously, you must rigorously separate your doses. Take your thyroid medication on a completely empty stomach first thing in the morning, and wait a minimum of four full hours before consuming any calcium supplements or calcium-fortified foods.
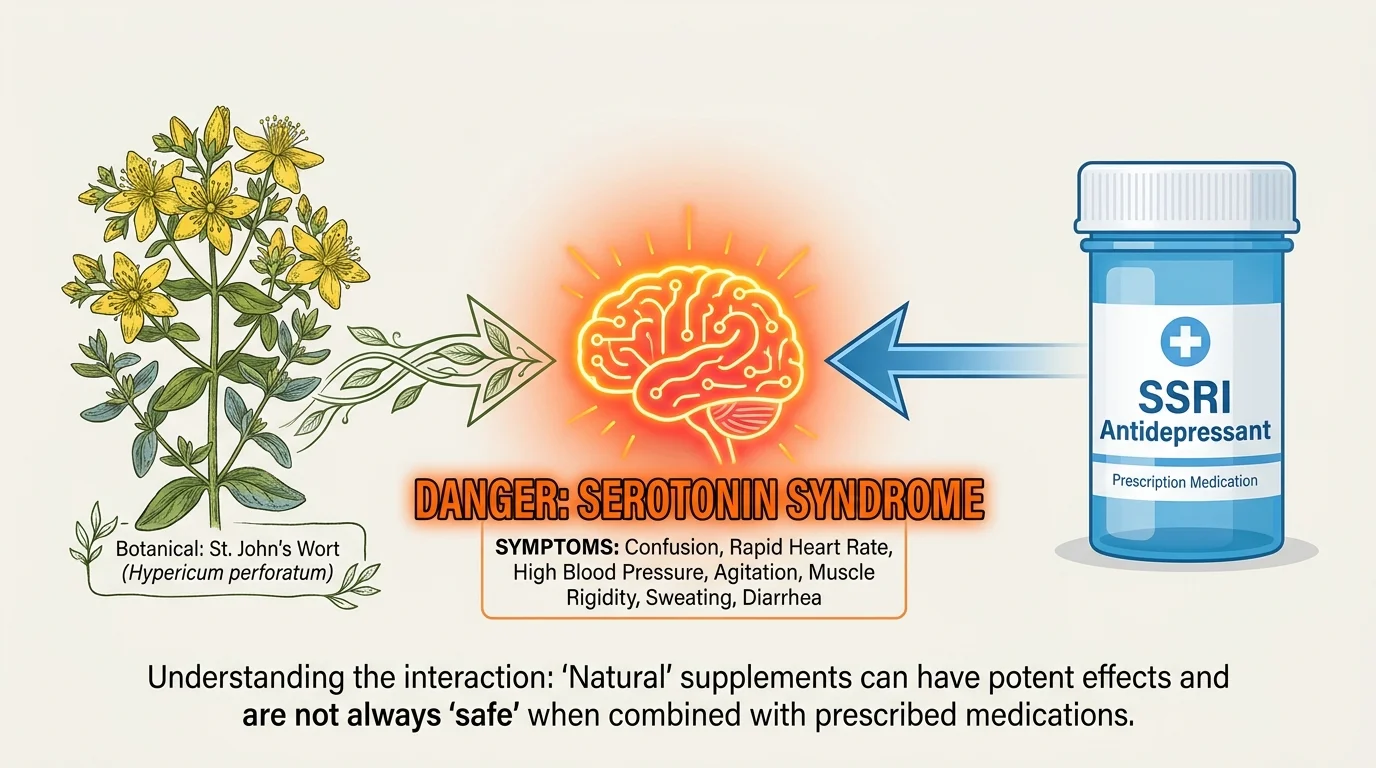
6. Herbal Supplements and Antidepressants
The global wellness market heavily promotes natural remedies to enhance memory and mood, but natural components do not always equate to safe interventions. Ginkgo biloba, a highly popular supplement for cognitive support, and St. John’s Wort, widely used for seasonal depression, cause severe chemical interactions with prescription selective serotonin reuptake inhibitors. Mixing St. John’s Wort with common medications like sertraline, citalopram, or fluoxetine can immediately trigger serotonin syndrome—a potentially fatal accumulation of serotonin in the brain characterized by intense muscle tremors, dangerously high fever, and sudden seizures. Furthermore, Ginkgo biloba possesses mild blood-thinning properties that interact negatively with antidepressants, significantly increasing your risk of spontaneous internal bleeding. You must treat all herbal supplements with the exact same respect and caution as pharmaceutical drugs and fully disclose every natural remedy to your primary healthcare provider.
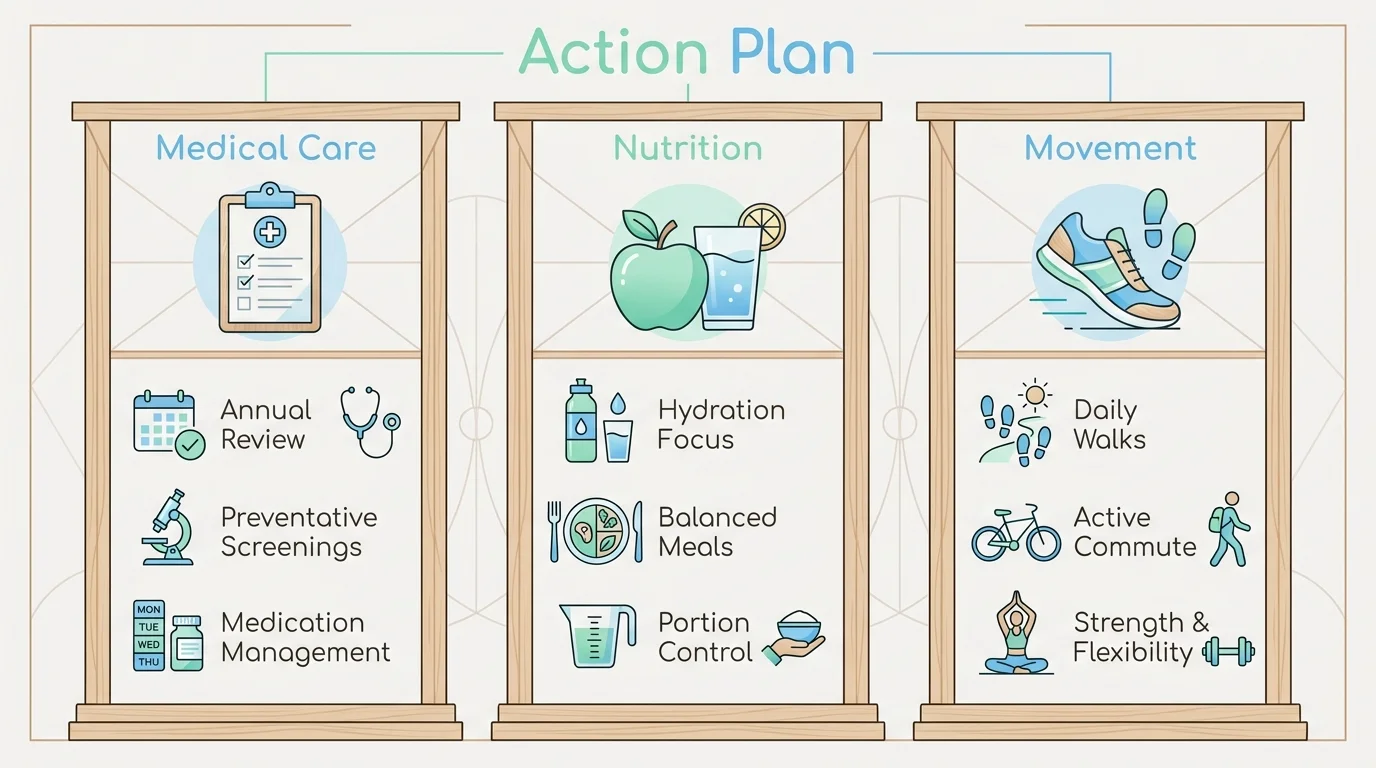
Strategy Pillars: A Holistic Approach to Medication Safety
Addressing the inherent risks of unsafe medication interactions requires a comprehensive, highly proactive strategy. By integrating careful medical oversight, daily nutritional awareness, and sustainable lifestyle modifications, you can drastically reduce your overall reliance on multiple medications and actively safeguard your long-term health.

Medical Care: The Comprehensive Medication Review
The absolute most effective defense against dangerous drug combinations is a formal, comprehensive medication review. Schedule a dedicated appointment with your primary care physician or a specialized clinical pharmacist to conduct a brown bag check; this involves physically bringing every pill bottle, daily vitamin, and herbal extract you consume into the office. During this detailed review, your healthcare team evaluates the ongoing necessity, precise dosage, and chemical safety of each item. This specific process frequently leads to deprescribing, which is a deliberate and medically supervised reduction of medications that no longer serve your primary health goals. Geographic and financial barriers often limit direct access to specialized geriatricians, but you can leverage local community pharmacists or modern telehealth services to obtain this vital clinical oversight. You can explore excellent patient resources through the American Geriatrics Society to find specialized tools that help expertly guide these crucial medical conversations.

Nutrition: Navigating Complex Food and Drug Interactions
Your daily diet intimately and directly affects how chemical medications perform inside your body. Beyond the well-known interactions—such as how certain compounds in grapefruit juice amplify the effects of specific statins and blood pressure pills as outlined by the Food and Drug Administration—you must also carefully monitor your intake of specific micronutrients. If you take the blood thinner warfarin, sudden, drastic changes in your consumption of vitamin K-rich leafy greens like spinach, kale, or Swiss chard will rapidly destabilize your blood clotting times. You certainly do not need to eliminate these incredibly nutrient-dense foods; rather, you must maintain a highly consistent daily intake so your doctor can accurately and safely calibrate your medication dose. Working directly with a registered dietitian perfectly empowers you to design a delicious meal plan that respects your specific medical constraints while providing the vital nutrition required for healthy, vibrant aging.

Movement and Mindset: Alternatives to Heavy Prescriptions
Embracing consistent physical movement and robust mental resilience practices provides incredibly powerful alternatives to managing symptoms exclusively with prescription pills. Chronic joint pain naturally drives many older adults toward a heavy, daily reliance on anti-inflammatory drugs or dangerous opioids. However, guided physical therapy, restorative yoga, and gentle aquatic exercises safely strengthen the supportive muscles surrounding your joints, naturally reducing structural pain and vastly improving mobility. For persistent anxiety and sleep disturbances—which are too often treated with risky benzodiazepines—mindfulness meditation and cognitive behavioral therapy for insomnia offer evidence-based relief completely free of chemical side effects. Acknowledging vital social determinants, such as access to safe neighborhood walking paths or affordable community wellness programs, remains essential. If local community resources are scarce, countless free digital platforms offer guided, senior-friendly routines that you can practice safely and consistently in your living room.

Real Voices: Clinician Perspectives on Polypharmacy
Medical professionals who specialize in the biology of aging consistently emphasize the paramount importance of vigilant, daily medication management. Clinical pharmacists specializing in geriatric care frequently observe the devastating downstream effects of unchecked polypharmacy. They note that many older patients end up in the emergency room simply because one specialist prescribed a new medication to treat the unrecognized side effect of another medication. This dangerous prescribing cascade traps seniors in a relentless cycle of worsening health and dependency. Geriatricians highly advise patients to view their current medication list not as a permanent, rigid fixture, but as a flexible, evolving treatment plan that requires constant medical auditing. Similarly, physical therapists working specifically with older adults continuously highlight that patients who commit to daily, gentle movement frequently and successfully eliminate their need for high-dose pain relievers, thereby restoring both their physical safety and sharp mental clarity.
Frequently Asked Questions About Medication Interactions
How often should I review my medications with a medical professional?
You should absolutely conduct a thorough, comprehensive medication review with your primary care provider or certified pharmacist at least once a full year. However, you must also immediately trigger a review whenever you experience a major health transition, such as being discharged from a local hospital, receiving a brand new medical diagnosis, or starting any new prescription. Constant medical vigilance ensures that temporary, short-term prescriptions do not inadvertently become permanent, hazardous fixtures in your daily routine.
Can common, everyday vitamins interact with my prescription drugs?
Yes, seemingly harmless daily vitamins frequently and severely interact with potent prescription medications. Beyond the well-known calcium and thyroid medication conflict, daily vitamins containing high doses of heavy minerals like iron or magnesium drastically interfere with the proper absorption of certain powerful antibiotics and osteoporosis medications. You must take strict inventory of every single over-the-counter supplement you swallow and discuss the optimal, safe timing for each dose with a certified pharmacist to prevent dangerous absorption failures.
What should I immediately do if I suspect an interaction is causing my symptoms?
If you suddenly develop unexplainable new symptoms—such as severe dizziness, profound physical fatigue, unusual bruising, dark stools, or sudden cognitive confusion—you must not abruptly stop taking your medications on your own. Abruptly ceasing certain drugs, particularly beta-blockers or heavy antidepressants, actively triggers incredibly dangerous physiological withdrawal effects. Instead, immediately contact your prescribing physician or a local emergency clinic, explicitly detail your exact symptoms, and forcefully request an urgent, same-day review of your current medication regimen.
Is it beneficial to use a single pharmacy for all my medical needs?
Consolidating all your prescription fills at a single, trusted pharmacy stands as one of the absolute most effective safety strategies for preventing dangerous drug interactions. When one dedicated pharmacy accurately maintains your complete medication profile, their internal computer systems automatically and instantly flag potential contraindications before the pharmacist ever hands you the bottle. If you absolutely must use different pharmacies due to strict insurance constraints or specialized compounding needs, you carry the absolute personal responsibility of keeping an updated, master written list of your medications and sharing it explicitly with every single provider.
Your Next Manageable Step
Safeguarding your ongoing health against dangerous drug combinations does not require you to suddenly become a medical expert in pharmacology; it simply requires you to become an active, highly vocal participant in your own healthcare journey. Your most vital, immediate next step involves gathering every single pill bottle, vitamin jar, and herbal supplement currently sitting in your home and placing them securely into a single bag. Call your primary care physician or your trusted local pharmacist today to boldly schedule a comprehensive medication review. As you mentally prepare for this empowering appointment, ask yourself: which of these daily chemical routines truly supports my long-term vitality, and which might actually be holding me back? Taking direct, confident control of your medication safety is a profound act of daily self-care that protects your independence and ensures a vibrant, highly resilient future.











Leave a Reply