Identifying subtle physical changes early empowers you to maintain your independence and avoid prolonged hospital stays as you age. When aches, fatigue, or memory slips become part of your daily rhythm, you might assume they are just a natural consequence of growing older. However, dismissing these minor discomforts often allows underlying conditions to progress quietly until they demand emergency medical intervention. By learning to distinguish between normal aging and genuine medical red flags, you can take immediate action and protect your long-term vitality. Your body constantly communicates its needs; you simply need to know how to listen and respond decisively.

The Science Behind Ignored Symptoms
Research consistently demonstrates that older adults frequently underreport symptoms to their physicians. Studies published by the World Health Organization indicate that a significant percentage of seniors attribute functional decline purely to chronological age—a phenomenon known as ageism directed inward. This cognitive bias delays crucial diagnostic testing and allows manageable conditions to evolve into acute crises. Data reveals that early intervention in chronic diseases significantly improves both the quality and length of life. For instance, addressing cardiovascular warning signs immediately can reduce the risk of a major cardiac event by more than half, allowing older adults to maintain robust, active lifestyles.
Clinicians recognize that physiological changes in older adults often present atypically compared to younger populations. A systemic infection might manifest only as mild confusion rather than a high fever; a silent heart attack might present as simple jaw ache rather than crushing chest pain. Understanding these atypical presentations remains essential for your proactive health management. The Centers for Disease Control and Prevention emphasizes that regular health screenings and immediate reporting of new symptoms serve as your most effective defense against premature decline. When you dismiss a persistent new ache, you deprive your healthcare providers of the vital clues they need to implement minimally invasive treatments.
The 7 Medical Red Flags You Should Never Ignore

Unexplained Weight Loss
Shedding pounds without actively altering your diet or exercise routine warrants immediate medical evaluation. While you might initially celebrate a looser waistband, dropping more than five percent of your body weight over six months serves as a prominent clinical warning sign. This involuntary loss frequently points to underlying malignancies, hyperthyroidism, gastrointestinal disorders, or undiagnosed depression. Your body requires substantial energy to fuel chronic disease processes, which manifests as accelerated calorie burning and muscle wasting. Bring this specific symptom to your primary care physician right away to initiate comprehensive blood panels and nutritional assessments before your immune system weakens.

Persistent or Atypical Breathlessness
Struggling to catch your breath after climbing a familiar flight of stairs signals that your cardiovascular or pulmonary systems need immediate clinical attention. Many seniors mistakenly blame a sudden drop in stamina on simply being out of shape. However, breathlessness that arises abruptly, worsens when you lie flat in bed, or wakes you up at night requires urgent investigation. These specific respiratory patterns strongly correlate with early-stage heart failure or chronic obstructive pulmonary disease. Do not wait for severe chest pain to validate your breathing difficulties; oxygen deprivation quietly damages your vital organs long before acute, unignorable symptoms strike.

Sudden Changes in Bowel Habits
Shifts in your digestive rhythm offer critical insights into your internal health, yet many individuals feel too embarrassed to discuss these changes. Experiencing newfound constipation, chronic diarrhea, or noticeably narrower stools demands an open conversation with a gastroenterologist. These fluctuations frequently accompany diverticulitis, thyroid dysfunction, or colorectal abnormalities. Furthermore, discovering blood in the stool—whether bright red or dark and tarry—always constitutes a medical emergency. Regular monitoring of your digestive baseline allows you to detect subtle deviations early and address inflammatory conditions before they severely compromise your daily nutrient absorption and overall physical comfort.
Transient Vision Alterations
Dismissing a brief loss of vision, a sudden influx of dark floaters, or intermittent blurred vision puts your long-term sight at severe risk. Seniors frequently attribute these episodes to simple fatigue, poor lighting, or dry eyes. However, a sudden shadow falling over your visual field or a burst of light flashes typically indicates a retinal detachment or a vascular occlusion inside the eye. Additionally, temporary dimming of vision in one eye serves as a classic presentation of a transient ischemic attack. Immediate ophthalmic evaluations drastically improve your chances of preserving your vision and preventing further neurological damage.

Uncharacteristic and Profound Fatigue
Feeling completely depleted after a routine day fundamentally differs from standard tiredness. If you find yourself needing multiple naps to function or lacking the energy to engage in beloved hobbies, your body is loudly signaling a systemic issue. Profound fatigue acts as the primary symptom for anemia, hidden bacterial infections, or progressive heart disease in older adults. Instead of attempting to push through the exhaustion with extra caffeine, track the frequency and severity of your fatigue in a notebook. Presenting this detailed log to your provider facilitates targeted testing for metabolic imbalances and oxygen delivery deficits.
Brief Episodes of Confusion or Speech Difficulty
Moments of profound disorientation, sudden physical clumsiness, or an inability to articulate words clearly demand immediate emergency care, even if the symptoms resolve completely within minutes. Many seniors write off these brief episodes as simple brain fog or harmless fatigue. In reality, these fleeting neurological deficits characterize transient ischemic attacks; they act as the ultimate warning sirens preceding a catastrophic stroke. Bypassing an emergency room visit guarantees that the underlying vascular blockage remains unaddressed and volatile. Time dictates the survival of brain tissue, making rapid medical intervention entirely non-negotiable for protecting your cognitive function.

New, Localized, or Severe Headaches
Developing a completely new type of headache after the age of fifty requires thorough diagnostic imaging. If you experience a sudden, thunderclap headache, pain localized strictly to the temples, or morning headaches accompanied by nausea, you must seek prompt medical care. These specific pain patterns frequently indicate temporal arteritis—a dangerous inflammation of blood vessels that can cause permanent blindness—or intracranial pressure anomalies. Relying on over-the-counter pain relievers merely masks the symptom without addressing the root cause. Swift diagnosis and steroid treatments prevent irreversible damage to your optic nerves and delicate vascular system.
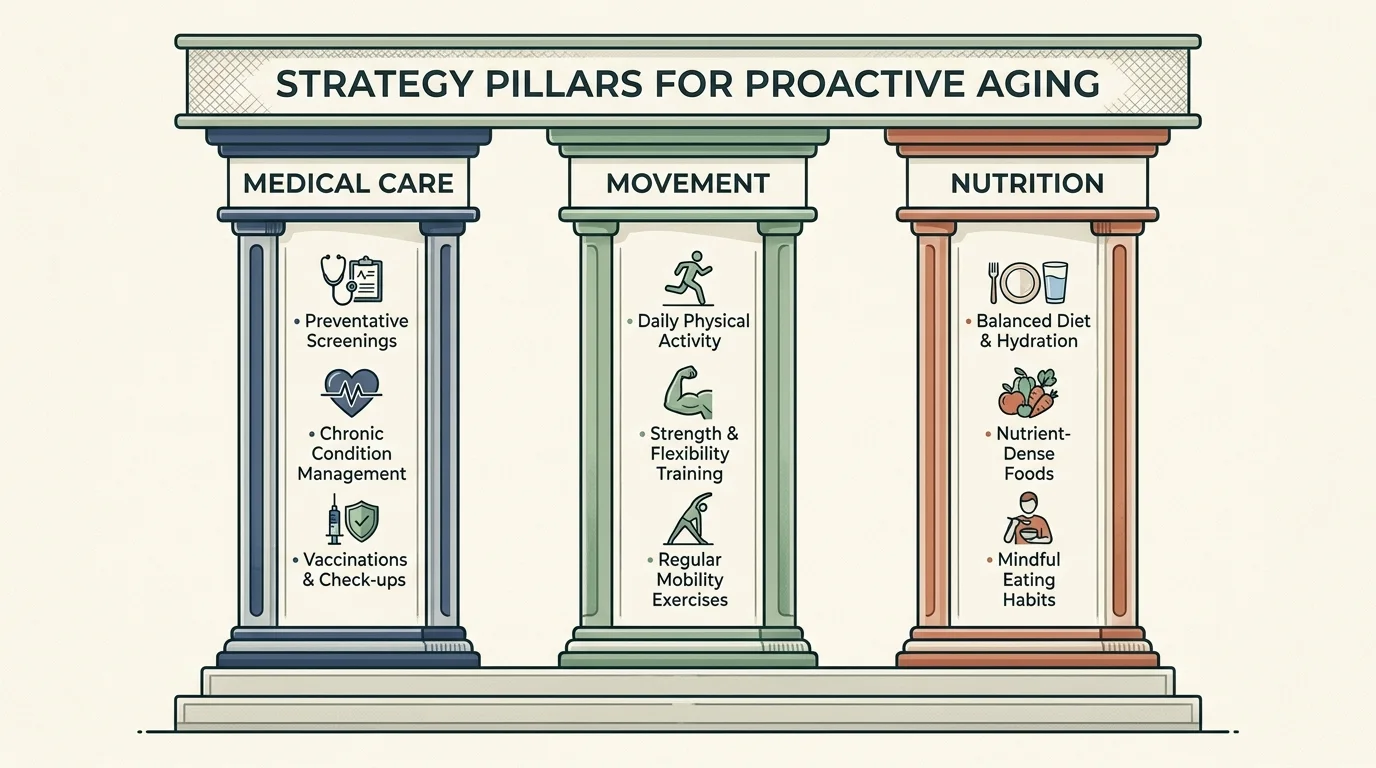
Strategy Pillars for Proactive Aging

Medical Care: Cultivating a Collaborative Team
Establishing an open, transparent dialogue with a trusted primary care physician forms the bedrock of healthy aging. You must feel entirely comfortable discussing potentially embarrassing symptoms without fear of dismissal or judgment. Prepare for every medical appointment by writing down specific physical changes, noting exactly when they began and what activities exacerbate them. Consider consulting the National Institute on Aging for standardized health checklists to guide these important conversations. Recognize that accessing quality healthcare depends heavily on your geographic location and financial resources; leverage community health centers or telehealth services if transportation barriers limit your access. Always advocate fiercely for yourself; if a symptom worries you, insist on a thorough investigation.

Movement: Strengthening Your Physical Baseline
Engaging in a consistent movement practice provides you with an intimate understanding of your body’s standard operating capacity. When you regularly participate in strength training, yoga, or daily neighborhood walking, you establish a highly reliable physical baseline. This routine makes it immediately obvious when a joint suddenly loses mobility or when your cardiovascular endurance drops inexplicably. Prioritizing regular movement enhances blood flow, improves joint lubrication, and bolsters your natural immune response. You actively prevent functional decline by challenging your muscular systems safely, which simultaneously amplifies your ability to detect genuine warning signs amidst normal exercise-induced soreness.

Nutrition: Fueling Resilience and Recognizing Deficits
Your daily dietary choices directly influence your cellular repair mechanisms, immune response, and overall energy levels. Consuming a diverse array of nutrient-dense whole foods minimizes systemic inflammation, thereby preventing diet-induced fatigue or digestive distress from masking actual medical symptoms. Pay close attention to how specific foods affect your body; a sudden intolerance to a lifelong favorite meal often hints at significant shifts in your microbiome or enzymatic production. Working with a registered dietitian, often sourced through directories provided by the Academy of Nutrition and Dietetics, can help you optimize your macronutrient intake. Proper hydration ensures your physiological systems accurately broadcast internal distress signals when trouble arises.

Insights from the Clinical Frontlines
Geriatric specialists repeatedly emphasize the profound danger of normalizing physical discomfort. Leading voices in elder care frequently note that chronological age alone is rarely a sufficient diagnosis for chronic pain or severe fatigue. Clinicians observe daily that patients who promptly report minor physical anomalies experience significantly better medical outcomes than those who wait for a full-blown crisis to seek help. Physical therapists echo this exact sentiment, pointing out that seniors often abandon beneficial physical activity due to an undiagnosed, easily treatable joint issue, triggering a rapid cascade of unnecessary physical decline. Proactive communication prevents reactive, prolonged hospitalizations. Your healthcare providers rely entirely on your daily bodily observations to guide their diagnostic process. By valuing your own physical intuition, you empower your medical team to deliver the precise, preventative care necessary for a vibrant life.
Frequently Asked Questions About Senior Health Symptoms
How can I tell the difference between normal aging and a medical issue?
Normal aging typically involves slow, gradual changes, such as a slight decrease in muscle mass over years or mild joint stiffness that improves as you move in the mornings. Conversely, medical issues usually present abruptly, asymmetrically, or with a severity that suddenly disrupts your established daily routine. If a physical change prevents you from participating in a normal activity or arises overnight, you must consult your physician to rule out acute conditions. Because individual baselines vary significantly, personalized care remains essential for an accurate clinical evaluation.
Should I go to the emergency room for a transient ischemic attack if I feel fine now?
Yes, you must seek emergency medical care immediately following any temporary neurological deficit, such as sudden limb weakness, facial drooping, or notably slurred speech. Even if the symptoms vanish entirely within ten minutes and you feel completely normal, a transient ischemic attack indicates a severe, temporary blockage of blood flow to the brain. Evaluating and treating the underlying vascular cause in a controlled hospital setting drastically reduces your risk of experiencing a catastrophic stroke in the near future.
What should I do if my doctor dismisses my new symptoms as just old age?
You hold the fundamental right to seek a second opinion whenever you feel your medical concerns are not being adequately addressed. If your current physician attributes a sudden, disruptive symptom solely to your age without conducting a thorough investigation, explicitly request a referral to a geriatrician. Geriatric specialists possess extensive, specialized training in the atypical ways illnesses present in older adults. The American Geriatrics Society provides extensive, searchable resources to help you locate a qualified elder care specialist in your local area.
Is it normal to lose my appetite entirely as I get older?
While a slight decrease in overall appetite can safely accompany a less active lifestyle or slower metabolism, completely losing your desire to eat is never a normal aspect of healthy aging. A profound loss of appetite frequently points to hidden dental problems, severe medication side effects, gastrointestinal disorders, or undiagnosed clinical depression. Because chronic malnutrition rapidly depletes your immune system and muscle mass, you should discuss any significant dietary changes with a healthcare provider immediately to formulate a safe nutritional plan.
Take Charge of Your Long-Term Vitality
Protecting your wellbeing requires continuous observation and the courage to speak up when something feels internally amiss. Your daily habits and bodily sensations offer the most accurate, reliable map of your overall health status. Start by dedicating just five minutes each evening to mentally scan your body, carefully noting any new aches, digestive shifts, or unusual waves of fatigue. Keeping a simple, accessible health journal empowers you to spot concerning trends and provides invaluable clinical data for your next medical appointment. What is one subtle physical change you have been quietly ignoring that you will bravely discuss with your doctor this week?










Leave a Reply