Protecting your kidney health requires recognizing subtle warning signs before severe damage occurs, especially as you age. Your kidneys act as your body’s master filtration system, silently removing waste and balancing vital fluids day after day. Because these bean-shaped organs are incredibly resilient, they often adapt to declining function without causing obvious pain or alarm. You might dismiss early kidney symptoms as normal signs of aging health or attribute them to lack of sleep and daily stress. By paying close attention to specific, quiet physical changes, you can partner with your healthcare team to catch potential issues early. Learning to identify these seven silent indicators empowers you to take prompt medical action and preserve your long-term vitality.
The Science Snapshot: Understanding Silent Decline
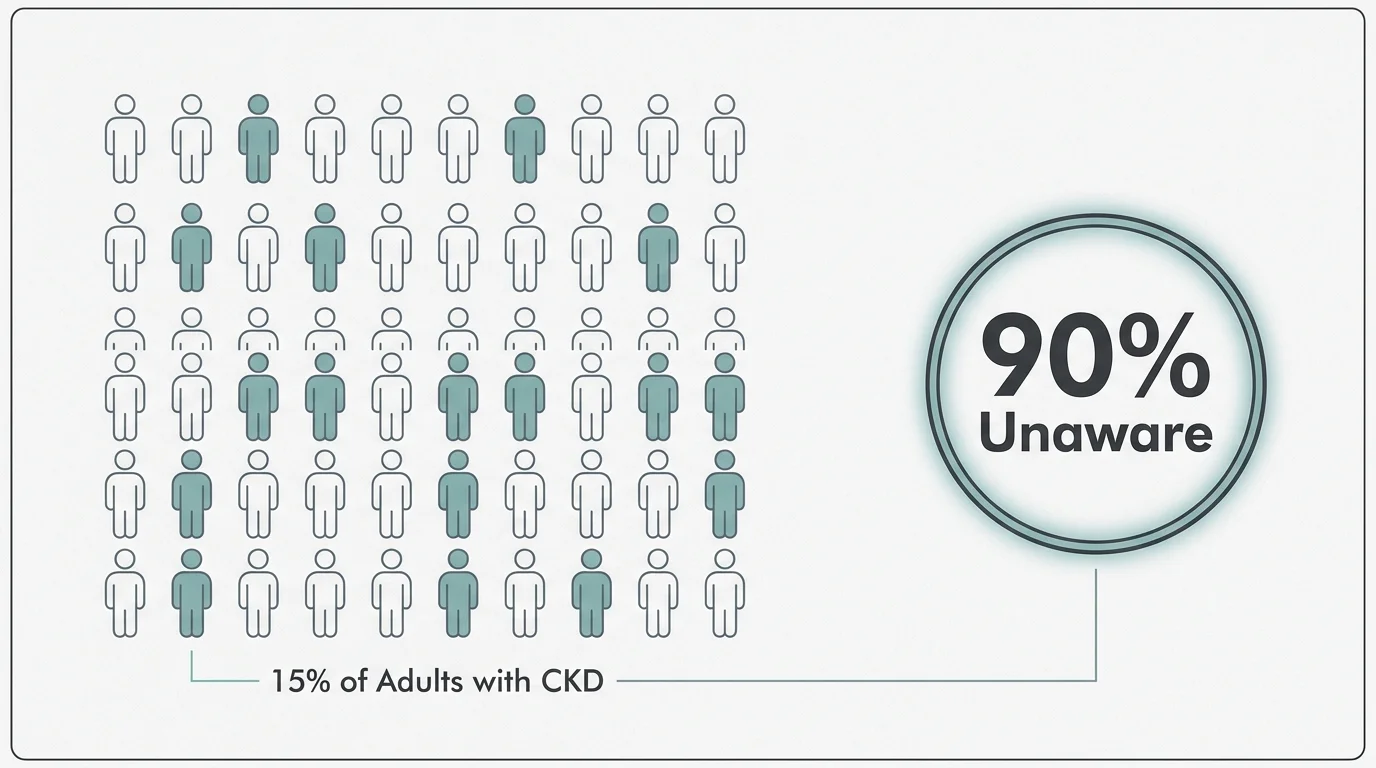
The statistics surrounding early-stage renal decline are staggering; millions of individuals live with compromised filtration systems without realizing it until the damage becomes severe. According to the Centers for Disease Control and Prevention, approximately fifteen percent of adults in the United States experience chronic kidney disease, yet nearly ninety percent remain entirely unaware of their condition. This massive awareness gap stems from the organ’s incredible biological adaptability. Because your body possesses two kidneys functioning as highly efficient filters, they easily compensate for microscopic damage by working harder, actively masking the subtle indicators of systemic distress.
Routine blood and urine tests often remain the only definitive methods for detecting early changes in your estimated glomerular filtration rate. Recognizing the physical hints your body drops can bridge the critical gap between unnoticed decline and proactive preservation. The earlier you spot these silent signs, the more effectively you can deploy lifestyle interventions to halt further progression.

Sign 1: Noticeable Changes in Urination Patterns
One of the earliest warnings your filtration system provides involves a shift in your daily bathroom habits. You may find yourself waking up multiple times during the night to urinate, a condition known medically as nocturia. When the organ’s internal filters suffer damage, they lose their ability to properly concentrate urine; this prompts an increased urge to relieve yourself regardless of your daily fluid intake.
For many individuals navigating aging health, these shifting patterns frequently get mistakenly attributed to benign prostate enlargement, fluctuating hormones, or standard menopausal changes. Paying close attention to the frequency, volume, and appearance of your urine provides crucial data. Foamy urine, which requires multiple flushes to clear, indicates that valuable protein is spilling over from your bloodstream into your bladder, demanding prompt investigation from your medical provider.

Sign 2: Pervasive Fatigue and Brain Fog
Chronic exhaustion that fails to improve with adequate rest often points to systemic imbalances beneath the surface. Healthy kidneys produce a vital hormone called erythropoietin, which directs your bone marrow to manufacture oxygen-carrying red blood cells. As renal function declines, the production of this essential hormone drops significantly.
This resulting shortage of red blood cells leads to anemia, depriving your brain and muscles of the oxygen they require for optimal daily performance. You might experience profound heaviness in your limbs, difficulty concentrating on routine tasks, or a persistent haze that disrupts your mental clarity. Understanding kidney symptoms requires looking beyond isolated organ pain and recognizing how these master filters influence your entire circulatory and neurological system on a daily basis.

Sign 3: Swelling in Your Ankles, Feet, or Hands
Fluid retention serves as a highly visible indicator that your body is struggling to manage its internal fluid volume. When healthy, your system perfectly balances sodium and water, efficiently excreting the excess through your bladder. Compromised filtration leads directly to sodium retention, forcing fluid to pool in your lower extremities due to gravity.
You may notice that your shoes feel uncomfortably tight by the afternoon or that your socks leave deep, visible indentations in your skin. While occasional swelling can result from standing for extended periods or consuming a highly salted restaurant meal, persistent edema requires professional evaluation. This warning sign highlights the critical connection between your daily sodium intake, vascular health, and your body’s waste management capabilities.
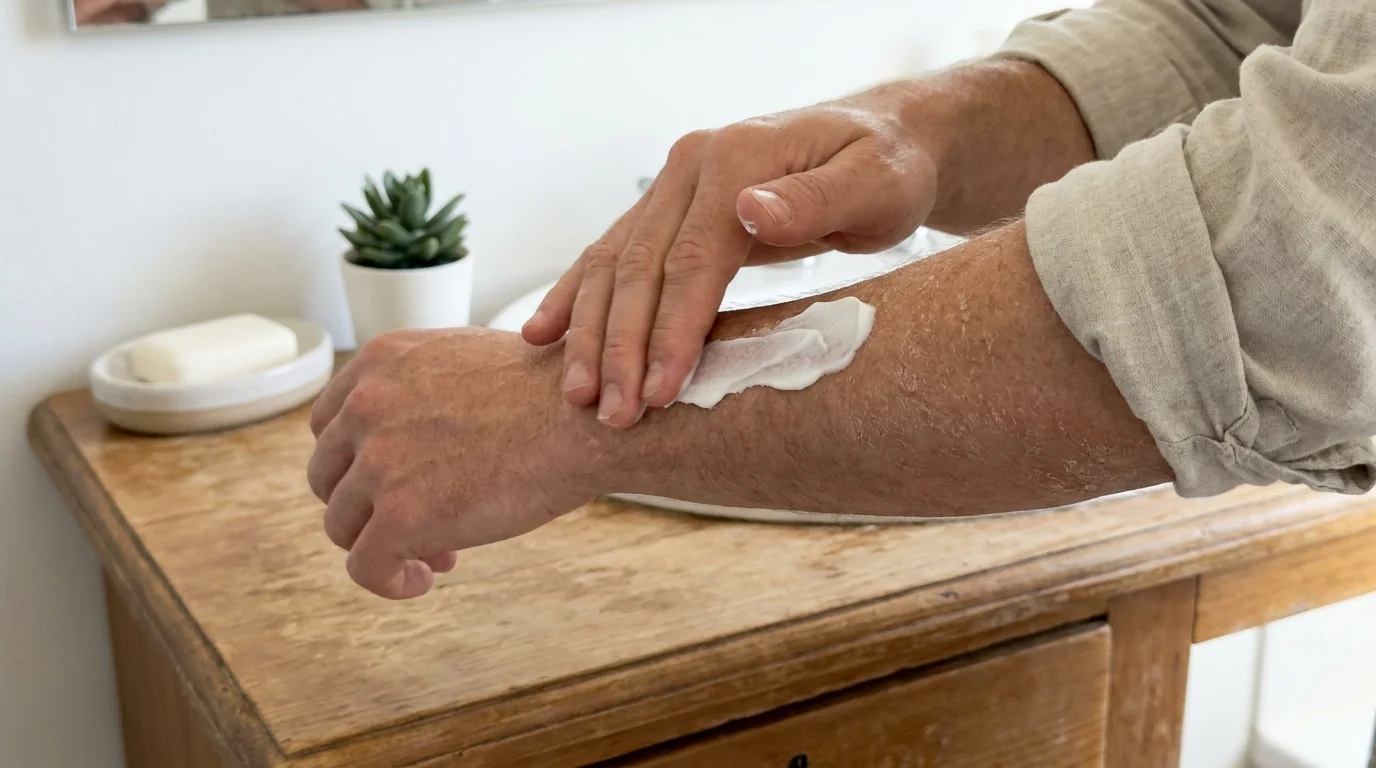
Sign 4: Severe Dryness and Itchy Skin
Most people associate dermatological issues with seasonal weather changes, completely overlooking the profound link between skin health and internal toxicity. Your renal system performs the complex task of maintaining the precise balance of minerals and nutrients circulating in your bloodstream. When this intricate balancing act fails, phosphorus and other minerals accumulate to toxic levels throughout your body.
This buildup triggers severe, relentless itching that feels deeply rooted beneath the surface of your skin, often failing to respond to topical moisturizers or standard over-the-counter antihistamines. According to resources from the National Institute of Diabetes and Digestive and Kidney Diseases, this intense pruritus frequently signals advanced mineral and bone disorders intimately tied to chronic renal failure. Addressing the root cause requires internal metabolic correction rather than external cosmetic creams.

Sign 5: Metallic Taste and Ammonia Breath
A sudden shift in how your favorite foods taste can indicate that metabolic waste products are accumulating rapidly in your bloodstream. This condition, known as uremia, alters your sensory perception and leaves a persistent metallic or bitter flavor in your mouth. You might notice that meat suddenly tastes repulsive or that your overall appetite has diminished significantly without any clear explanation.
Rising urea levels also create a distinct ammonia odor on your breath that rigorous brushing and flossing cannot eliminate. Experiencing unexplained weight loss alongside these sensory changes requires immediate medical investigation, as it reflects a severe systemic response to accumulating toxins that your body can no longer eliminate efficiently through normal urinary pathways.

Sign 6: Shortness of Breath Without Exertion
Struggling to catch your breath after simply walking across a room or climbing a short flight of stairs warrants careful attention. This terrifying sensation connects to kidney decline in two distinct, interconnected ways. First, the severe anemia caused by decreased hormone production leaves your entire body starved of oxygen, forcing your lungs to work overtime to compensate for the deficit.
Second, the fluid retention that causes swelling in your extremities can also cause dangerous fluid to accumulate inside your lungs, creating a sensation of drowning or severe chest tightness. Never disregard unexplained breathlessness as a mere consequence of declining senior health or minor deconditioning; it demands a comprehensive cardiorenal evaluation to ensure your heart and internal filters are functioning harmoniously.

Sign 7: Puffy Eyes, Especially in the Morning
While a restless night can certainly leave you with mild under-eye bags, persistent periorbital edema indicates a specific type of critical protein loss. The intricate micro-filters within your kidneys, known as glomeruli, are designed to retain valuable proteins in your blood while allowing waste and excess water to pass through into your bladder.
When these tiny filters sustain structural damage, significant amounts of albumin leak into your urine. The loss of albumin disrupts the osmotic pressure in your blood vessels, allowing fluid to seep into the surrounding delicate tissues, particularly the thin skin around your eyes. Severe morning puffiness that resists cold compresses likely signals a critical loss of vital proteins and requires a simple urine test to confirm the presence of microscopic vascular damage.
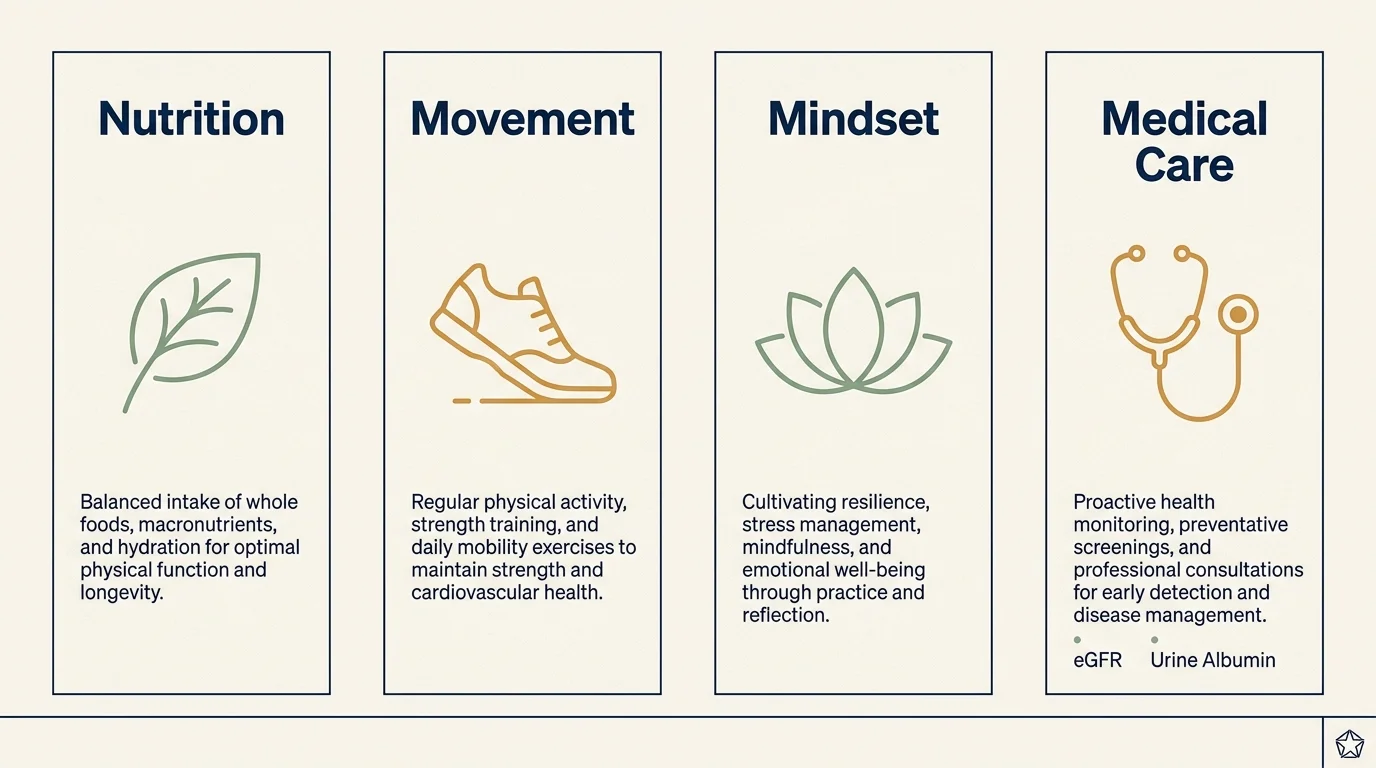
Strategy Pillars: Protecting Your Kidney Health

Nutritional Adjustments for Renal Support
Taking control of your dietary patterns provides an immediate and powerful defense against progressive internal damage. Transitioning toward a plant-forward diet rich in fresh vegetables, whole grains, and lean proteins actively reduces the workload on your biological filters. Managing your daily sodium intake remains paramount; excess salt forces your body to hold onto water, driving up blood pressure and accelerating structural damage to your internal vessels.
Working alongside a certified expert helps you navigate the complex balance of potassium, phosphorus, and protein specific to your individual metabolic needs. The Academy of Nutrition and Dietetics emphasizes that personalized medical nutrition therapy can significantly delay the progression of renal decline, essentially transforming your daily meals into highly protective medicine.

Movement and Cardiovascular Fitness
Consistent physical activity bolsters your vascular health, which directly sustains the delicate blood vessels feeding your internal organs. Engaging in moderate aerobic exercise—such as brisk walking, swimming, or cycling—improves blood circulation and helps manage underlying chronic conditions like hypertension and insulin resistance. You do not need to perform grueling, high-intensity workouts to reap these significant benefits; daily consistency matters far more than extreme exertion.
Aim for thirty minutes of intentional movement most days of the week, carefully tailoring the activity to your current mobility levels. Integrating light strength training two days a week further enhances your metabolic stability. Regular movement serves as an active biological shield, regulating your blood sugar and reducing the chronic, systemic inflammation that threatens your organ function over time.

Mindset and Stress Management
Chronic psychological stress triggers a cascade of hormonal responses that elevate your blood pressure and constrict your blood vessels, placing immense mechanical strain on your entire circulatory system. Cultivating a resilient mindset through intentional stress management techniques protects your physical architecture from this invisible, daily wear and tear. Practices such as deep diaphragmatic breathing or mindfulness meditation actively engage your parasympathetic nervous system.
This healing “rest and digest” state dilates your blood vessels, substantially improving oxygen-rich blood flow to your vital organs. Recognizing the profound connection between your mental state and your physiological health empowers you to treat relaxation not as an optional luxury, but as a foundational, non-negotiable component of your holistic medical care.

Proactive Medical Care
Partnering with your trusted healthcare team for regular laboratory screening ensures that you catch microscopic metabolic changes long before they manifest as physical discomfort. Because early decline produces absolutely no obvious warnings, requesting a comprehensive metabolic panel and a urine albumin-to-creatinine ratio test provides the objective clarity you need. These simple, non-invasive diagnostics measure your estimated glomerular filtration rate and detect microscopic protein leakage instantly.
According to the World Health Organization, early detection of noncommunicable diseases represents the single most effective strategy for preventing premature mortality and improving your long-term quality of life. Always discuss your complete medication and supplement list with your physician, as certain over-the-counter pain relievers can inadvertently cause acute toxic damage if consumed excessively.

Real Voices: Insights from the Clinic
Clinical professionals continually emphasize the power of patient awareness in fundamentally altering the trajectory of chronic illness. Nephrologists frequently observe that patients who actively monitor their bodies and forcefully advocate for routine testing achieve vastly superior health outcomes compared to those who wait for severe medical distress to strike.
One clinical specialist notes that patients often reflect on their diagnosis by revealing they felt chronically tired for years, but simply assumed it was an unavoidable part of growing older. By validating these subtle, quiet shifts in your energy, taste, and fluid balance, clinicians encourage you to deeply trust your own intuition. True health optimization occurs only when you combine the objective data of modern laboratory tests with the subjective wisdom of your own lived physical experience.
Frequently Asked Questions
What is the most common early symptom of kidney decline?
In the earliest stages, most individuals experience absolutely no noticeable physical changes; this is precisely why proactive laboratory testing remains essential. When signs do eventually surface, changes in bathroom habits—specifically an increased need to urinate during the night—frequently present as the very first tangible indicator. You should never ignore persistent nocturia, as it often signals a loss of concentration ability.
How does high blood pressure affect kidney function?
Hypertension acts as both a primary cause and a destructive consequence of renal impairment. Elevated pressure forces blood violently through your delicate internal capillaries, creating microscopic scar tissue over time. As these critical filters harden and fail, they release specific stress hormones that drive your blood pressure even higher, creating a dangerous, self-perpetuating cycle that requires careful medical management and lifestyle adjustment.
Can drinking more water reverse existing organ damage?
While maintaining adequate daily hydration supports overall filtration and helps prevent the formation of kidney stones, simply drinking massive quantities of water cannot repair existing structural tissue damage. In fact, if your functional capacity has already decreased significantly, consuming excess fluids can dangerously exacerbate lower-body swelling and shortness of breath. Always consult your primary physician to establish a personalized daily hydration goal.
When should I see a doctor about changes in my urination?
You should immediately schedule a medical evaluation if you experience foamy urine, visible blood in the toilet bowl, or a sudden, unexplained increase in urgency that disrupts your sleep for more than two consecutive weeks. Prompt medical attention becomes especially critical if these urinary changes occur alongside sudden daytime fatigue, persistent skin itching, or unexplained swelling in your lower extremities.
Moving Forward with Your Health
Safeguarding your long-term vitality begins with a firm commitment to mindful observation and proactive medical screening. You hold the considerable power to change your health trajectory by recognizing these subtle physical cues and discussing them openly with your medical provider. Instead of waiting for a severe crisis to dictate your choices, take one highly manageable step today: schedule your annual wellness exam and specifically ask for an updated renal panel. As you reflect on your daily habits this week, consider how a few simple, sustainable adjustments to your hydration and nutrition might profoundly support your body’s remarkable internal filters for decades to come.









Leave a Reply