Recognizing hantavirus symptoms early can mean the difference between a minor scare and a life-threatening respiratory emergency. When you clean out a dusty shed or sweep up a rural cabin, you risk inhaling airborne virus particles shed by infected rodents. Because early symptoms closely mimic the flu—causing fever, deep muscle aches, and profound fatigue—many people dismiss the warning signs until severe breathing difficulties arise. Understanding how this rodent borne disease progresses empowers you to seek immediate medical intervention before fluid floods your lungs. You need to know the specific timeline of symptom onset and the crucial environmental triggers that require vigilance to protect your respiratory health.

The Science Behind Hantavirus Transmission
Hantavirus pulmonary syndrome is a severe respiratory disease caused by an infection with hantaviruses. In North America, the most prominent strain is the Sin Nombre virus, predominantly carried by the deer mouse. The mechanism of transmission is stealthy and invisible to the naked eye. When infected rodents excrete the virus in their urine, droppings, and saliva, the viral particles dry out over time. If you disturb these dry particles by sweeping, vacuuming, or simply walking through a heavily infested and poorly ventilated space, the virus becomes aerosolized. Breathing in these microscopic, airborne droplets introduces the pathogen directly into your respiratory tract.
Understanding this etiology is crucial because it highlights why specific environments pose such high risks. Closed-up buildings, rural barns, grain bins, and long-abandoned cabins serve as perfect incubators for the virus. Clinical data from the Centers for Disease Control and Prevention indicates that anyone who comes into contact with rodent-infested environments is at risk, regardless of their underlying health status. However, we must also acknowledge that social determinants of health play a massive role in exposure rates. Agricultural workers, individuals living in substandard housing without proper pest exclusion, and rural populations with limited access to immediate medical care bear a disproportionate burden of this disease. Addressing these systemic inequities is a vital component of public health prevention strategies.

Early Warning Signs You Cannot Ignore
The incubation period for hantavirus can be surprisingly long; symptoms typically begin to surface anywhere from one to eight weeks after your initial exposure to infected rodent droppings. The earliest phase of the illness is notoriously difficult to diagnose because it masquerades as a conventional seasonal flu. You will likely experience a sudden onset of fever, profound fatigue, and intense muscle aches. These muscle aches, known medically as myalgia, are particularly localized in large muscle groups—you will feel a deep, aching soreness in your thighs, hips, back, and sometimes your shoulders.
Alongside these universal early markers, roughly half of all infected individuals experience pronounced gastrointestinal distress. Nausea, vomiting, diarrhea, and severe abdominal pain frequently accompany the fever, leading many people to mistakenly believe they are suffering from a stomach bug or food poisoning. Headaches, chills, and dizzy spells are also common during this initial period. Because these early viral signs lack specific respiratory hallmarks, doctors often misdiagnose the condition unless the patient explicitly mentions a recent history of rodent exposure or activities like cleaning out a dusty outdoor structure.
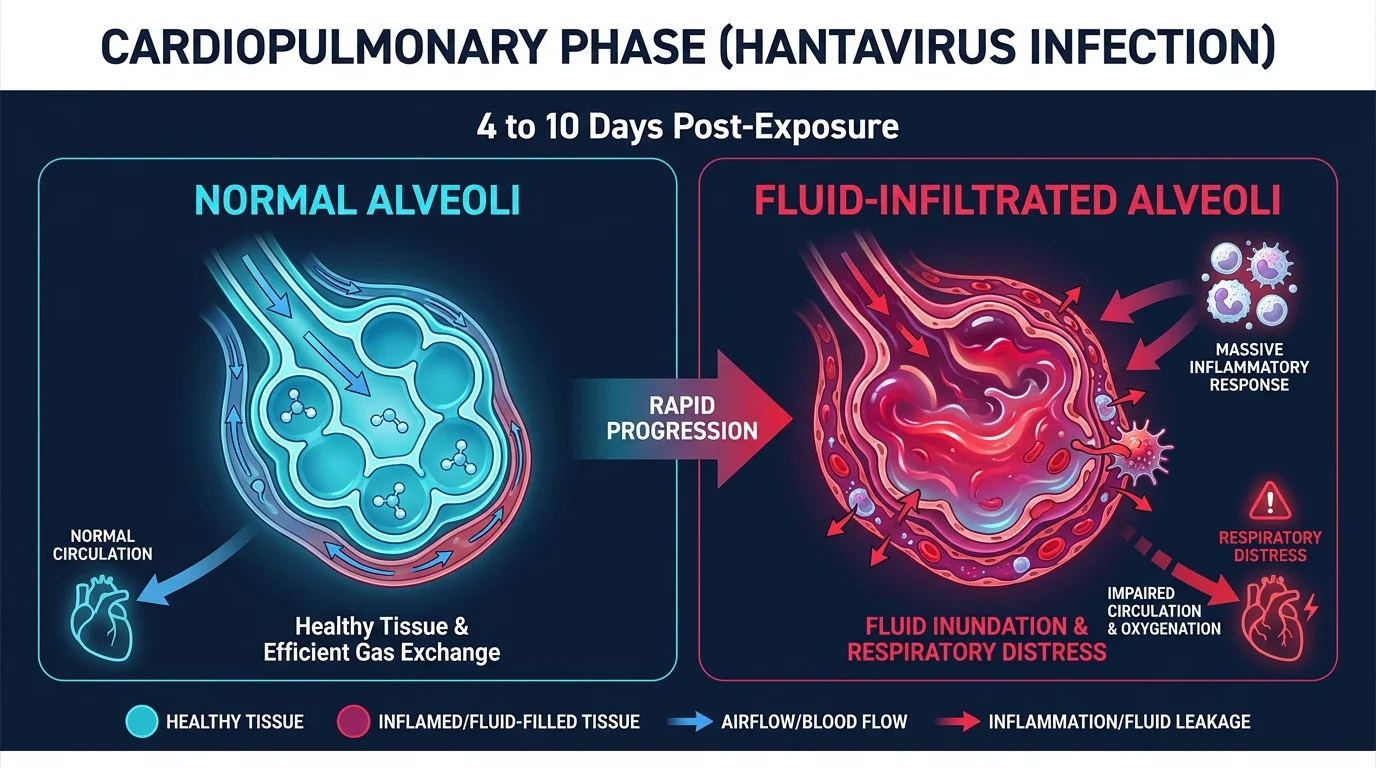
The Dangerous Shift to Respiratory Distress
The true danger of a hantavirus infection reveals itself during the cardiopulmonary phase, which typically strikes four to ten days after the initial flu-like symptoms begin. This transition is abrupt and terrifying. The virus triggers a massive inflammatory response within the endothelial cells that line your blood vessels, particularly within your lungs. This inflammation causes a condition known as capillary leak syndrome; your blood vessels become dangerously permeable, allowing blood plasma to flood into the air sacs of your lungs.
As pulmonary edema sets in, you will develop a persistent, dry cough and an escalating shortness of breath. Patients often describe the sensation as feeling like a tight, suffocating band has been wrapped around their chest, or as if they are drowning from the inside out. This rapid deterioration of lung function drastically reduces the oxygen levels in your bloodstream, leading to profound hypoxia. At this stage, hantavirus pulmonary syndrome becomes a dire medical emergency. Without immediate, intensive medical intervention, the condition can quickly progress to acute respiratory failure and cardiogenic shock. Research from the National Institutes of Health demonstrates that early recognition of this specific respiratory deterioration is the single most critical factor in improving patient survival rates.
Holistic Pillars for Respiratory Resilience and Recovery
Navigating the threat of a rodent borne disease requires a comprehensive strategy that addresses your environment, your immediate medical needs, and your long-term physical recovery. By implementing actionable steps across different aspects of your life, you can significantly reduce your risk of exposure and ensure your body is prepared to heal if you do face a severe respiratory infection.

Proactive Medical Care and Self-Advocacy
Your relationship with your healthcare provider is your first line of defense once symptoms appear. If you develop a fever and deep muscle aches after cleaning a shed, camping in a rural area, or noticing mouse droppings in your home, you must advocate for yourself aggressively. Do not wait for respiratory symptoms to manifest before seeking care. When you visit an urgent care center or emergency room, explicitly inform the attending physician about your recent rodent exposure. This specific piece of medical history is often the only clue that prompts a doctor to run specialized serological blood tests for hantavirus antibodies rather than simply sending you home with instructions to rest and hydrate. If your condition progresses to the pulmonary phase, treatment will require admission to an intensive care unit where clinicians can provide supplemental oxygen, mechanical ventilation, or, in extreme cases, extracorporeal membrane oxygenation to support your failing lungs and heart.

Environmental Mindset and Anxiety Reduction
Fear of outdoor spaces and rural environments is a common psychological reaction to learning about aerosolized viruses. However, replacing anxiety with mindful, evidence-based preparation allows you to enjoy nature and maintain your property safely. Before cleaning any space that has been closed up for a long time, open all doors and windows to cross-ventilate the area for at least thirty minutes. Never use a broom or a vacuum cleaner on dry rodent droppings, as this directly aerosolizes the viral particles. Instead, saturate the contaminated area with a commercial disinfectant or a mixture of bleach and water. Allow the liquid to sit and neutralize the virus for five minutes before wiping up the debris with paper towels while wearing rubber gloves and a secure mask. Adopting these methodical cleaning protocols transforms a potentially dangerous environment into a manageable household chore.

Nutritional Support for Immune Defense
While no specific food can prevent or cure an acute hantavirus infection, maintaining a robust, well-nourished body gives your immune system the resources it needs to mount an effective defense and recover from severe physiological stress. Surviving an intensive care stay takes a massive metabolic toll on your body. Whether you are aiming to prevent illness or actively recovering from a respiratory infection, prioritize a diet rich in anti-inflammatory compounds. Focus on incorporating high-quality lean proteins to repair damaged cellular tissues, alongside abundant colorful vegetables and fruits that provide essential antioxidants like vitamin C and zinc. Staying meticulously hydrated keeps the mucosal linings of your respiratory tract functioning optimally. For personalized guidance on rebuilding your physical strength and muscle mass after a prolonged, severe illness, consulting a registered dietitian through resources like the Academy of Nutrition and Dietetics can provide you with tailored metabolic strategies.

Movement and Pulmonary Rehabilitation
Surviving hantavirus pulmonary syndrome is a profound victory, but the journey to full health does not end when you leave the hospital. Post-viral fatigue and diminished lung capacity can linger for months. Regaining your endurance requires a strategic, phased approach to physical movement. In the early stages of recovery, forced cardiovascular exercise can backfire, causing severe setbacks. Instead, you should focus entirely on respiratory physiotherapy. Work with a physical therapist to learn diaphragmatic breathing exercises that gently re-expand the lower lobes of your lungs and improve oxygen exchange. As your pulmonary function stabilizes, you can gradually introduce light, low-impact movements such as restorative yoga or short, flat-surfaced walks. The American Lung Association emphasizes that slow, consistent respiratory conditioning is the most effective pathway to reclaiming your baseline stamina after an acute cardiopulmonary crisis.

Real Voices in Clinical Practice
Understanding the clinical reality of this illness requires listening to the professionals who treat it and the patients who endure it. Infectious disease specialists repeatedly emphasize that the diagnostic puzzle hinges entirely on patient communication. Clinicians note that when a previously healthy adult arrives at the emergency room with unexplained, rapidly progressive shortness of breath, a detailed environmental history is just as critical as a chest X-ray. Doctors working in rural healthcare settings often observe that the initial symptoms are so deceptively mild that patients try to push through the fatigue, only seeking help when they can no longer walk across a room without gasping for air.
From the patient perspective, survivors of hantavirus pulmonary syndrome frequently describe the psychological trauma of their physical deterioration. Many recall the terrifying speed at which their bodies shut down, transitioning from feeling slightly under the weather to requiring life support in a matter of hours. Their stories serve as powerful reminders that vigilance is not paranoia; recognizing the warning signs and respecting the severity of zoonotic diseases can quite literally save your life. Organizations tracking global health threats, such as the World Health Organization, continue to highlight patient narratives to raise awareness about the hidden dangers of human-wildlife interactions.
Frequently Asked Questions About Hantavirus Symptoms
Can hantavirus spread from person to person?
In North America, the strains of hantavirus responsible for causing pulmonary syndrome—most notably the Sin Nombre virus—cannot be transmitted from one person to another. You cannot catch this specific respiratory infection from touching, kissing, or being near an infected individual, nor can it be contracted from a healthcare worker. You must inhale the aerosolized rodent excrement directly. However, it is important to note that a different strain found in South America, known as the Andes virus, has documented cases of rare person-to-person transmission among close contacts.
How quickly do hantavirus symptoms appear after exposure?
The incubation period is notoriously variable and can be frustratingly long. Symptoms generally take anywhere from one week to eight weeks to manifest after you inhale the viral particles. This long gap often causes individuals to forget about the exposure event entirely. By the time the initial fever and muscle aches appear, you might not associate your current illness with the dusty attic you cleaned out a month prior, making accurate self-reporting to your physician incredibly difficult.
Are early hantavirus symptoms different from COVID-19 or the seasonal flu?
During the first few days, distinguishing hantavirus from COVID-19 or influenza based purely on symptoms is nearly impossible without laboratory testing. All three conditions present with systemic inflammation, high fever, fatigue, and muscle aches. However, hantavirus does not typically cause the distinct loss of taste and smell associated with COVID-19, nor does it immediately present with a runny nose or sore throat like many common colds. The differentiating factor is almost always your recent environmental history and the abrupt, severe shift into fluid-filled lungs a few days later.
What exactly should you tell your doctor if you suspect an infection?
If you experience severe flu-like symptoms and have recently been in a high-risk environment, you must provide your doctor with a clear chronological narrative. Tell them exactly when you were exposed to rodents or rodent droppings, what specific activities you were doing—such as sweeping a cabin, opening a sealed crawlspace, or working in an agricultural building—and when your fever and muscle aches began. Explicitly ask if they can rule out hantavirus pulmonary syndrome, which prompts them to order the appropriate serologic tests for specific antibodies rather than just standard viral panels.
A Compassionate Approach to Your Preventive Health
Protecting yourself from rare but severe environmental pathogens does not require living in fear; it requires replacing ignorance with intentional, informed action. By understanding how the virus is transmitted and recognizing the critical timeline of symptoms, you possess the knowledge needed to protect your respiratory health. When you respect the spaces where wildlife and human habitats intersect, you inherently lower your risk of exposure.
Your health is a continuous practice of awareness and self-advocacy. The most manageable first step you can take today is simply assessing your own living spaces and storage areas for signs of rodent activity, ensuring you have the right supplies—like bleach, rubber gloves, and proper masks—ready before you begin any deep cleaning projects. Take a moment to reflect on your own environmental exposures: are there neglected spaces in your home that require a mindful, safe approach to maintenance? By addressing these areas with care and caution, you create a safer, healthier environment for yourself and your family.









Leave a Reply