As you pass your 65th birthday, your risk for developing vision-threatening conditions multiplies rapidly. Protecting your independence requires knowing exactly which visual changes are harmless and which signal irreversible damage. Recognizing the earliest warnings of macular degeneration, glaucoma, and cataracts allows you to seek prompt medical intervention before permanent vision loss occurs. Ignoring subtle distortions, sudden flashes, or a gradual narrowing of your peripheral sight can cost you your ability to drive and read. Understanding the specific symptoms that warrant an immediate visit to an ophthalmologist empowers you to take control of your aging eyes. Prompt diagnosis and modern therapies can preserve your eyesight for decades to come.

Understanding Age-Related Vision Threats
The passage of time changes the physical structure of your eyes. Your lenses become less flexible and increasingly dense; your retinas thin out; the vital fluids circulating within your ocular chambers can face drainage issues. While minor changes like needing stronger reading glasses represent a normal part of aging known as presbyopia, other silent structural shifts often precede devastating eye diseases. Aging introduces systemic challenges—like fluctuating blood pressure, elevated blood sugar, and cumulative cellular oxidative stress—that directly target the fragile blood vessels and nerves supporting your vision.
Medical professionals diagnose age-related eye conditions through comprehensive dilated eye examinations. During these detailed assessments, an ophthalmologist administers special eye drops to widen your pupils, allowing a clear view of the retina and the optic nerve at the back of your eye. Advanced diagnostic tools have revolutionized early detection. Optical Coherence Tomography uses light waves to capture cross-sectional images of your retina, revealing microscopic layers of tissue and pinpointing early signs of disease long before you notice visual symptoms. Visual field testing further maps your peripheral sight to uncover blind spots indicative of early optic nerve damage. Connecting with established comprehensive guidelines helps you understand the exact tests your doctor will perform during these vital annual visits.
Genetics also play a formidable role in your ocular health profile. Having a family history of glaucoma or macular degeneration substantially heightens your personal risk. Decades of exposure to ultraviolet light without adequate protection accelerates the formation of cataracts and damages the macula. Recognizing these underlying risk factors allows you and your healthcare provider to construct a personalized monitoring schedule. Early detection remains the single most effective strategy for preventing irreversible blindness in older adults.
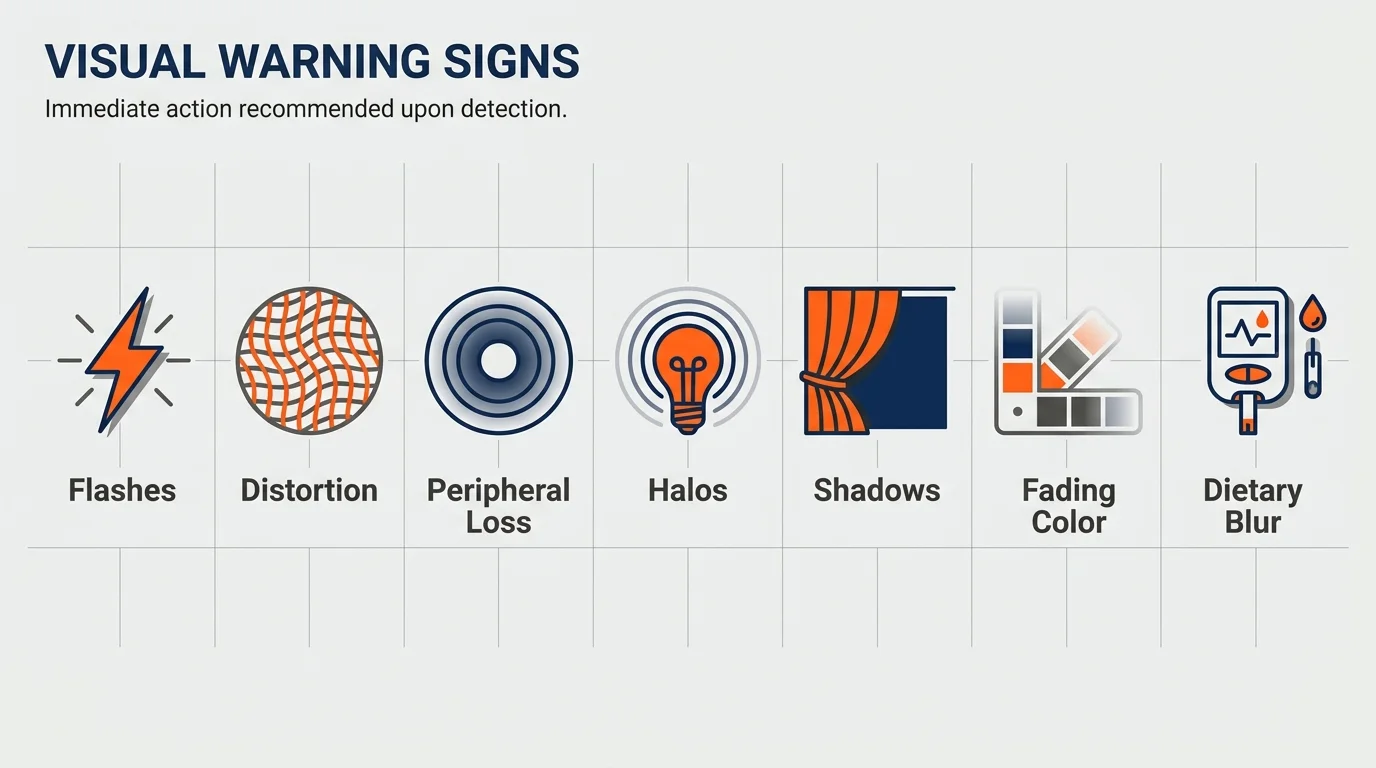
The 7 Warning Signs You Cannot Ignore

A Sudden Surge of Floaters and Flashes of Light
Seeing an occasional tiny speck drifting across your line of sight is generally harmless. However, a sudden, dense shower of new floaters—often described as looking like a swarm of bugs or cobwebs—signals a serious structural shift inside your eye. This phenomenon frequently occurs alongside abrupt flashes of light that mimic a camera flash in your peripheral vision. These symptoms typically indicate that the gel-like substance inside your eye, called the vitreous, is pulling away from the retina.
While posterior vitreous detachment itself happens naturally with age, the traction it exerts can tear the delicate retinal tissue. A retinal tear creates a pathway for fluid to seep underneath the retina, pushing it away from its nourishing blood supply and causing a retinal detachment. This constitutes an absolute medical emergency. Seeking immediate surgical intervention can reattach the retina and save your sight; waiting even a single day can result in permanent, profound vision loss.

Straight Lines Appearing Wavy or Distorted
When the straight edges of doorways, window blinds, or sentences on a page suddenly look warped or wavy, you are experiencing metamorphopsia. This highly specific visual distortion serves as the hallmark warning sign of Age-Related Macular Degeneration. The macula forms the precise center of your retina, governing your sharp, central vision required for recognizing faces, reading, and watching television. As you age, yellow deposits called drusen can accumulate under the macula, disrupting its smooth contour.
In the aggressive wet form of macular degeneration, abnormal blood vessels proliferate beneath the retina. These fragile vessels leak fluid and blood, physically lifting and warping the macula. This fluid accumulation bends the light entering your eye, making straight lines appear bent or broken. Using an Amsler grid—a simple chart resembling graph paper—allows you to monitor your central vision daily. Noticing any new distortion on this grid demands an urgent evaluation by a retinal specialist.

A Gradual Loss of Peripheral Sight
Primary open-angle glaucoma earns its reputation as the silent thief of sight because it steals your peripheral vision so gradually that your brain compensates for the loss until the damage becomes severe. You might begin bumping into door frames, failing to notice cars in your side mirrors, or feeling like you are looking through a narrow tunnel. This insidious loss of side vision stems from progressive damage to the optic nerve, the vital cable that transmits visual data from your eye to your brain.
The damage usually results from elevated intraocular pressure. When the clear fluid produced inside your eye fails to drain properly, pressure builds up and mechanically crushes the delicate fibers of the optic nerve. Because you cannot feel this elevated pressure, the disease advances silently. Relying solely on your own perception of your visual field leaves you vulnerable; routine professional pressure measurements and optic nerve scans remain the only ways to catch this thief before it robs you of your independence.

Severe Eye Pain Accompanied by Nausea and Halos
While open-angle glaucoma develops painlessly, acute angle-closure glaucoma strikes with sudden, agonizing intensity. If you experience severe, throbbing pain in one eye accompanied by a headache, nausea, vomiting, and blurry vision, you must seek emergency medical care immediately. You may also notice bright, rainbow-colored halos ringing around light sources, and your eye may appear noticeably red and feel hard to the touch.
This agonizing presentation occurs when the drainage angle inside your eye becomes completely blocked, causing internal eye pressure to spike rapidly to dangerous levels. This extreme pressure suffocates the optic nerve within hours. Intravenous medications and emergency laser procedures are required to break the fluid blockade and rapidly lower the pressure. Dismissing this severe pain as a mere migraine can lead to permanent blindness in the affected eye within a single day.

A Dark Shadow or Curtain Falling Across Your Vision
A dark, impenetrable shadow creeping across your visual field—often described as a gray curtain being drawn over a window—represents a critical warning sign of a progressing retinal detachment. Unlike cataracts, which cause general blurriness, this shadow completely obscures a specific portion of your sight. The shadow usually begins in the periphery and marches relentlessly toward your central vision.
This shadow physically maps the exact area where your retina has peeled away from the back wall of your eye. The detached tissue ceases to function, creating a corresponding blind spot. Alternatively, a sudden, painless dark curtain descending over one eye can indicate a transient ischemic attack or a vascular occlusion—essentially a stroke within the eye. Both scenarios demand immediate dispatch to an emergency room or a specialized eye clinic.

Rapidly Fading Colors and Increasing Glare at Night
If the vibrant world around you begins to look washed out, yellowed, or sepia-toned, you are likely witnessing the progression of cataracts. Your eye’s natural lens must remain crystal clear to focus light precisely onto the retina. Over decades, the proteins within this lens break down and clump together, creating cloudy, opaque areas that scatter incoming light. This scattering severely degrades your visual clarity.
Beyond fading colors, cataracts drastically amplify glare. You may find night driving increasingly treacherous as the headlights from oncoming traffic fracture into blinding starbursts. Reading requires progressively brighter lamps, yet the increased light only creates more uncomfortable glare. Fortunately, modern cataract surgery offers a highly effective, definitive solution, replacing the clouded lens with a clear artificial implant to restore crisp, vibrant vision.

Fluctuating Blurriness Tied to Your Diet
Seniors managing diabetes must remain intensely vigilant regarding their vision. If you notice that your visual acuity fluctuates drastically from day to day—or even hour to hour—you are likely experiencing the ocular effects of shifting blood sugar levels. High glucose concentrations cause the lens of your eye to swell, temporarily altering your prescription and blurring your focus. As your blood sugar stabilizes, the lens slowly returns to its normal shape.
More dangerously, chronic elevated blood sugar destroys the microscopic blood vessels nourishing the retina, resulting in diabetic retinopathy. These damaged vessels leak fluid into the macula, causing swelling known as diabetic macular edema. Without strict glycemic control and targeted medical intervention, these vascular changes trigger the growth of fragile new blood vessels that bleed easily, leading to profound vision loss. Reviewing current public health data reinforces the critical connection between systemic metabolic control and long-term visual health.
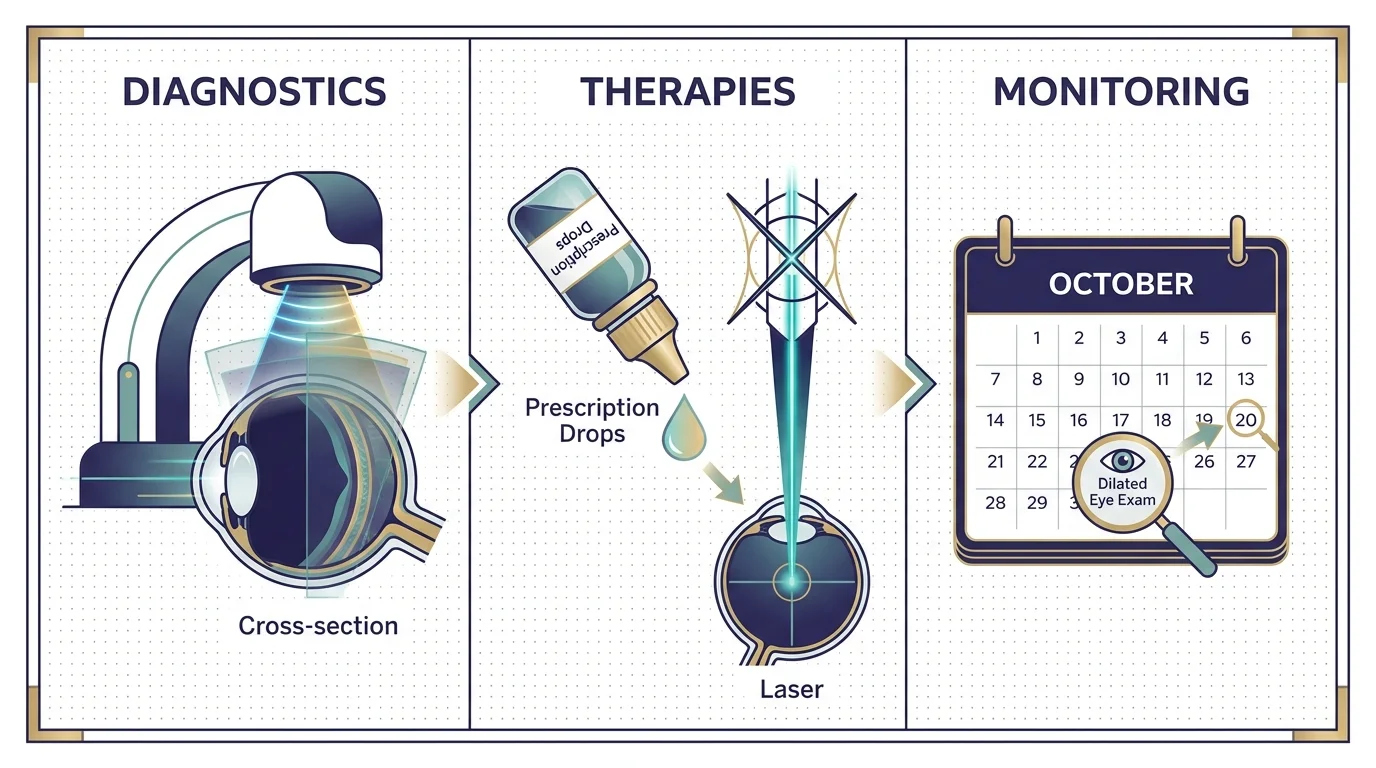
The Treatment Landscape for Senior Eye Diseases
The medical community has made extraordinary strides in treating age-related eye conditions, transforming previously blinding diseases into manageable chronic conditions. For patients battling wet macular degeneration and diabetic retinopathy, the advent of anti-VEGF therapy has revolutionized the standard of care. Ophthalmologists inject these specialized medications directly into the eye to block a specific protein that stimulates abnormal blood vessel growth. While the thought of an eye injection sounds terrifying, the procedure involves powerful localized anesthetics and takes only seconds, consistently halting disease progression and frequently restoring lost vision.
Glaucoma management traditionally relies on prescription eye drops that either reduce fluid production or improve drainage to lower intraocular pressure. However, patients who struggle with the daily regimen of eye drops now have access to Minimally Invasive Glaucoma Surgery. Surgeons frequently perform these micro-incisional procedures in tandem with cataract removal, implanting microscopic stents into the eye’s drainage system to naturally lower pressure with exceptional safety profiles.
Lifestyle interventions serve as a powerful adjunct to conventional medical therapies. Extensive clinical trials have proven that specific nutritional interventions profoundly impact retinal health. The AREDS2 formulation—a precise blend of vitamin C, vitamin E, zinc, copper, lutein, and zeaxanthin—has been clinically shown to reduce the risk of intermediate macular degeneration progressing to the advanced, vision-threatening stage. Engaging with clinical research initiatives allows you to understand the robust scientific data supporting these specific nutritional protocols; however, you must consult your physician before starting any high-dose supplements to ensure they do not interact with your current medications.
Emerging therapies continue to push the boundaries of ocular medicine. Researchers are actively developing sustained-release drug implants that eliminate the need for daily glaucoma drops, alongside groundbreaking gene therapies aimed at halting inherited retinal degenerations. While these advanced treatments offer immense hope, strict adherence to your current conventional treatment plan remains your strongest defense against disease progression.

Living Well with Changing Vision
Experiencing vision loss triggers profound emotional and practical challenges, but it does not mean surrendering your independence. Mastering self-management techniques allows you to navigate your daily life safely and confidently. Simple home modifications yield dramatic improvements; increasing ambient lighting, eliminating trip hazards like loose throw rugs, and utilizing high-contrast colored tape on staircase edges significantly reduce your risk of debilitating falls. Low vision specialists can introduce you to an array of practical tools, from handheld digital magnifiers to voice-activated smart home devices that read recipes, adjust thermostats, and announce the time.
Your caregivers and family members play an indispensable role in your visual health journey. Because definitive diagnostic exams require dilating your pupils—which leaves you temporarily sensitive to light and unable to focus on close objects—securing reliable transportation to and from your appointments ensures you never miss a critical evaluation. Caregivers can also provide vital assistance with organizing intricate eye drop schedules, ensuring you administer the correct medications at the precise intervals required to keep diseases like glaucoma fully suppressed.
Building a robust, collaborative healthcare team forms the foundation of successful long-term management. Your team should include a board-certified ophthalmologist for disease management and surgical intervention, an optometrist for routine refraction and specialized low-vision aids, and your primary care physician to manage underlying systemic conditions like hypertension and diabetes. Exploring patient advocacy resources connects you with support groups and educational materials that empower you and your family to advocate effectively for your comprehensive care needs.
Frequently Asked Questions About Senior Eye Health
How often should I get an eye exam after 65 even if I have no warning signs?
You should schedule a comprehensive dilated eye examination every one to two years after reaching the age of 65, even if your vision seems perfectly fine. Many vision-threatening conditions, particularly glaucoma and early-stage macular degeneration, develop silently over several years without producing any noticeable symptoms. Routine dilated exams allow your ophthalmologist to detect microscopic changes in your retina and optic nerve, enabling proactive treatment long before irreversible damage impacts your daily life.
Does Medicare cover routine eye exams and treatment for diseases like glaucoma?
Original Medicare does not cover routine eye exams strictly for prescribing glasses or contact lenses. However, Medicare Part B does cover annual preventative eye exams if you have diabetes or are at high risk for glaucoma. Furthermore, Medicare covers comprehensive medical exams, diagnostic tests, and surgical treatments—including cataract surgery and anti-VEGF injections—when you exhibit specific symptoms or receive a diagnosis of a medical eye condition. You should verify your specific benefits with your insurance provider or supplemental plan administrator.
What new research offers hope for vision loss in older adults?
The field of ophthalmology is advancing rapidly, offering unprecedented hope for older adults. Current clinical trials are testing stem cell therapies designed to replace dead retinal cells in patients with advanced macular degeneration. Researchers are also refining neuroprotective medications intended to shield the optic nerve from damage in glaucoma patients, independent of eye pressure. Connecting with educational support networks keeps you informed about these revolutionary breakthroughs and potential opportunities to participate in clinical trials.
Can lifestyle changes actually reverse macular degeneration or glaucoma?
No lifestyle change, diet, or exercise routine can reverse the structural damage already caused by macular degeneration or glaucoma. Once the optic nerve fibers die or the macula scars, that specific vision is permanently lost. However, aggressive lifestyle interventions—such as quitting smoking, managing blood pressure, maintaining strict diabetic control, and wearing UV-blocking sunglasses—can drastically slow the progression of these diseases and protect your remaining sight. Lifestyle changes act as a critical defense mechanism, not a cure.
Protecting Your Independence and Looking Forward
Acknowledging that your vision is changing requires courage, but taking proactive steps to protect your sight represents the ultimate act of self-preservation. Your eyes have served you tirelessly for over six decades, capturing a lifetime of memories, faces, and experiences; they deserve meticulous care and immediate attention when warning signs arise. By familiarizing yourself with the subtle distortions, sudden shadows, and painful pressure spikes that signal ocular distress, you transform yourself from a passive patient into an empowered advocate for your own health.
Never dismiss a sudden visual change as just another unavoidable consequence of getting older. Reach out to your ophthalmologist the moment you notice an anomaly, engage openly with your support network, and commit to your prescribed therapeutic regimens. Modern medicine offers remarkable tools to halt disease and preserve your sight, ensuring that your future remains sharp, vibrant, and entirely within your focus.








Leave a Reply