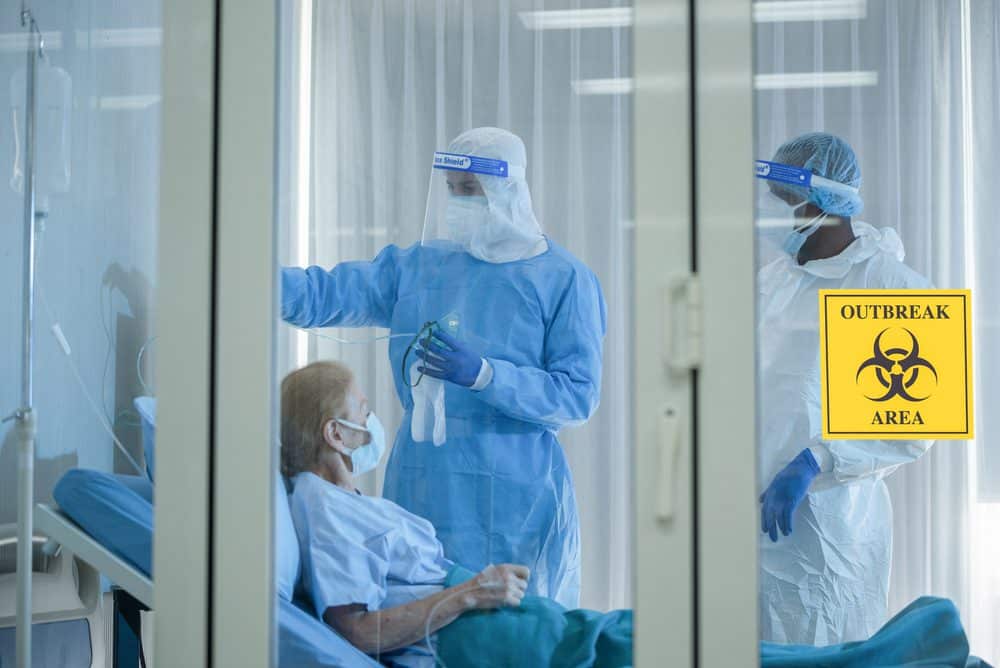
This fall, when Americans were processing the almost inexistent transition from summer to fall, COVID-19 alarms started to arise. First, there was a steady uptick in wastewater COVID-19 levels, followed by a slight increase in hospitalizations.
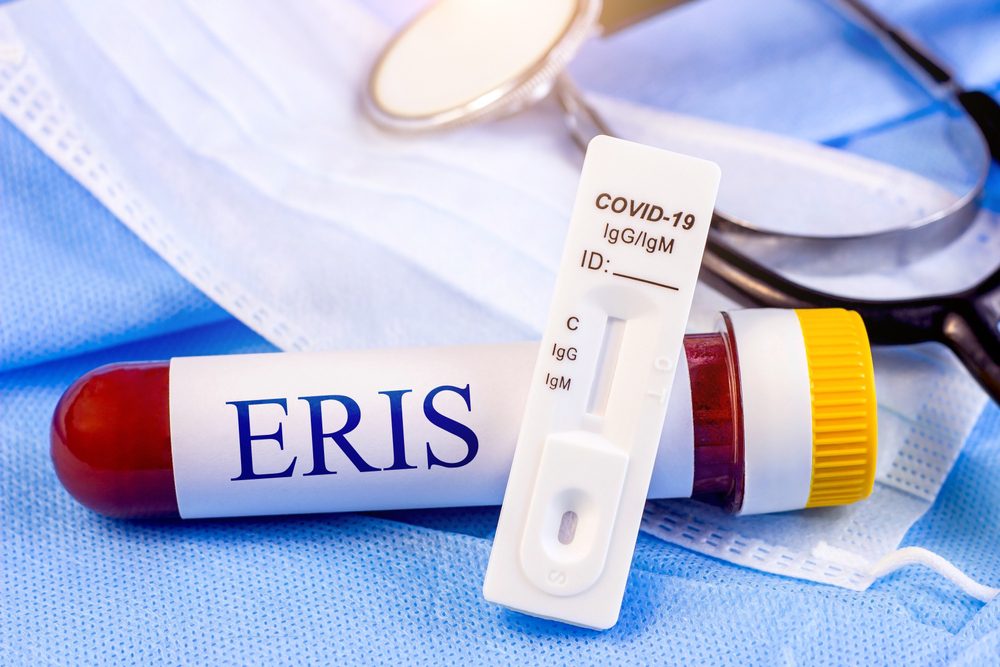
Then, right in the middle of August, the World Health Organization declared it was monitoring a brand new omicron variant known as BA.2.86, also known as Pirola, created from a high number of mutations.
The sheer amount of genetic distance from its ancestors was extremely concerning to the majority of experts. The variant had no less than 30 mutations, and about the same number differentiated the highly transmissible and viral omicron variant from its predecessors.
Moreover, experts feared the worst was yet to come. As it turns out, Pirola is more transmissible and less susceptible to vaccine-induced protection than other variants circulating over the past year and a half.
Over the last couple of weeks, plenty of laboratory studies led to a positive relief: on a cellular level, Pirola isn’t as alarming. This means that the chances of this variant leading to a massive room-flooding of COVID-19 are quite small.
Other, less mutated omicron variants are still dominant strains, and it seems very unlikely for Pirola to wreak major havoc anytime soon.
Also, there’s positive news: scientists are doing enough sequencing to detect any new variants before they’re widespread. But this shouldn’t lead you to believe that you don’t need to get vaccinated anymore.
Even if there’s no scary new variant on the horizon, COVID-19 transmission is still on the uptick, and along with it, a very unwelcome sense of familiarity.
If you’re wondering what the current state of COVID-19 is today, we’re going to get into that immediately. Here’s a closer look at the latest COVID-19 variant and the COVID-19 hospitalization situation, but also as to what COVID-19 transmission trends over time.








Haven’t your lies killed enough people with the Clot Shot?
Ain’t that the truth?
I find it hard to understand those who choose to believe that the vaccine will do harm, and believe all the false theories posted by ignorant people.
@Raetta I Romero what planet did you come down from? Talk about ignorant!!!
One thing you can’t believe is everything the so called experts say, about almost anything concerning peoples health, since when do the medical industry want people to be totally healthy(?) That means they would not make much money off of your health misfortunes, know that they been experimenting with Covid since 1931, concerning germ-warfare, and up until 2020, they finally got the right variant introduce to all of humanity, trying to so called reduce the human population, and they are still trying new options with the same virus RNA, because there are as many as 15,000 of them to experiment with. Also know that every people in the world don’t need to take the vaccine shot only certain people need to, they Stated this back in 2020, but decided to say everyone should take it knowing people will get sick and die from it. Please do your research.
I so believe this to be true, no way do they have our best interest at heart, they only treat to keep us sick so they make money off us, if they cured us then no more money!!!
People are so unbelievably blind to the science! It’s amazing.
I find it hard to believe the folks who comment think of themselves as infectious disease experts. Everything on Google is not true!
One thing you can’t believe is everything the so called experts say, about almost anything concerning peoples health, since when do the medical industry want people to be totally healthy(?) That means they would not make much money off of your health misfortunes, know that they been experimenting with Covid since 1931, concerning germ-warfare, and up until 2020, they finally got the right variant introduce to all of humanity, trying to so called reduce the human population, and they are still trying new options with the same virus RNA, because there are as many as 15,000 of them to experiment with. Also know that every people in the world don’t need to take the vaccine shot only certain people need to, they Stated this back in 2020, but decided to say everyone should take it knowing people will get sick and die from it. Please do your research.
Vaccine almost killed my husband. In his medical records. Wake up! Take it if you choose. I’m in the never again category.
Facts
Even harder to believe there are still people who believe in the vaccine! How you can ignore the data around the countries that have disavowed the use of the vaccine, US VAERS data around vaccine injuries, the CDC’s own data around vaccine efficacy and LOW (17%) rates of people even getting vaccines and boosters. It takes enormous effort to actually ignore the “conspiracies”! lol
You find it hard to believe because you are still asleep. There is SIGNIFICANT evidence from highly reputable sources. Better not hit snooze again, the alarm is sounding.
Kind of like we were supposed to believe everything Faucci said during the pandemic which turned out to be mostly bs?
Easy to understand when you knew 2 people who died as a result of the vaccine but none who died of the disease itself.
Greetings from the country! Know lots of them, they are gullible, incredibly stubborn and tend to be poorly educated. For which they pay a great price. I’m 68, when I was a child they lined you up in first grade and everybody got a vaccine. And that was it, no argument or asinine “theories” allowed. Propaganda is the actual source of the problem, literally it is “Better” then ever. And it works.
Ray, do a little research PLEASE before you make comments. Go to the CDC website & see how they back tracked about: “Take the shot & you won’t be a carrier – not true. “Take the shot & it will protect you from Covid – not true because it mutated. “Take the shot as it will never migrate from the shot area – not true. They have found the MRNA in the brain & other places. Or how about Fauci being question by Congress about what scientific proof was used for the 6 feet of difference between people. He admitted that there was none. After scientists have written papers about the harm the shots have done to people, the UK & other European countries are not promoting the shots. I’m begging you to stop taking the booster shots as you are destroying your immune system. It may not affect you now, but (down the road) you may develop health issues that could cause death. Our mortality rate is off the charts & they have lowered our life expectancy. This occurred around the time of when everyone was told to take the shot. Lastly, I asked my doctor if his
clinic was giving money to doctors as an incentive for pushing the shots. He stated that it was true, but he saw no harm as it incentivized them to promote the shots That is just plain greed!
I have a serious question no one will answer, why is it that my backside being double masked doesn’t work while expelling gas, but a single mask on a person’s face works every time to keep the molecular viruses out…?
Have you taken samples to know that it doesn’t???
What a stupid question. Ask your surgeon to be mask free the next time you have surgery.
The mask diminishes the distance your breath travels. Additionally masks serve to reduce the innoculum reducing disease severity. Admittedly the common mask is imperfect as are all human endeavors.
My son, however ran (at the bedsides) a 40 bed Covid ventilator unit for 13 months with an n95 mask and never developed antibodies (until of course the immunization became available). Ordinary people cannot be expected to understand aseptic technique.
David Bramm, MD FAAFP
is covid increasing or not?
Another new strain. China just want stop.
Please give me a break you guys are bought and paided for comparison covid with Republicans and Democrat.. We want our country back!
Please, don’t make Covid a political issue. Not Everything is a political issue. Really! Be thankful for this Thanksgiving Day and remember our Forefathers who made this day possible. God bless America! 🦃 🇺🇸
Illegal aliens bringing it.
Boy, you got that right!!!!!!!
This is my 3rd time that I have incurred illness from covid. Covid is here to stay. Please, everyone In regards to staying virus free proceed with caution and listen to the experts.
So why are the experts saying that people who got the vaccines are dying at alarming rates and people who didn’t get the vaccines are doing just fine????? Fact 68% in America 🇺🇸 did NOT get these killing vaccines!!!
Is it OK to get the flu shot at the same time you get the new Covid shot?
Yes. I got the RSvy shot, flu shot, and the Eris vaccination within days of each other, if not, altogether.
yes
I was wondering abt getting flu, Covid& RSV vaccines @ same time especially disabled every day w/ daily migraines.
I don’t see any responses from who started this thread. Disappointing.
They say it’s safe but they also said the vaccines were safe so they should not be trusted. It’s to much on your immune system so why take the chance. They only care about the $.
These replies are proof of the morons that exist. And unfortunately there are many.
Only a moron would choose “Boo”
It seems to me that with the locations given being border crossings and surrounding states that the cause being illegal immigrants holds a lot more water than trying to imply it’s politically based.
Makes a thinking person wonder what has really happened to the USofA when everyone starts believing every political lie they are told. Remember for a moment that our own Supremes Court (pun intended) ruled that because it is in the nature of a politician to lie they cannot be held accountable for any campaign lies they tell the people… What’s to stop them from taking it a step farther and lying about the other party?? THINK people…USE your brains…DO NOT believe everything you are told just because it is YOUR party telling it….
What I find interesting is the authors lack of scientific thinking. This isnt a political issue. If it starts in the south, it starts in the south. Would be akin to me saying (when covid first started), “The states with the worse cases are New York, Washington, and California. What’s interesting is these are all democrat run states.). Ignoring the fact that these are also the major ports into the US from abroad.
This article reeks of ignorance and shows how worthless this website really is.
Somebody will always read something into something that just isn’t there. COVID is a disease, it is not part of a conspiracy, or grand plan to annihilate. It is not a ruse to gain power. It is a disease among many more. The medical community is here to cure disease and they are. It’s that simple! Vaccinations and masking have proven to work.
FYI, the Governor of New Mexico is a Democrat. But why even bring politics up? In the states with Republican Governors is it only Democrats who get sick??
Doesn’t it seem weird that now we have Covid every year, but you never hear about Flu cases?
What kind of teaser do you think is funny, to not let us know what those I nine states are?
You’d have to be totally ignorant or insane to get the jab now. Another narrative-busting study published in February in the journal Frontiers in Immunology titled, “Brief research report: impact of vaccination on antibody responses and mortality from severe COVID-19.” Joining the steady drip of many other troubling findings about the jabs, this one found vaccinated patients were more likely to have severe covid outcomes than were unvaccinated patients. Researchers found that among covid patients, mortality was significantly higher in vaccinated patients (70%) compared to unvaccinated patients (37%), even after adjusting for comorbidities. Even more fascinating, they found the vaccinated patients had higher total IgG4 antibody levels, suggesting jabbed people develop an improper immune tolerance allowing spike protein to run wild. Remember – Safe and Effective isn’t a lie, it’s two lies…
U R A MORE ON
Fully cited books to educate yourselves
“The Real Anthony Fauci”
“The Wuhan Cover up”
Both by RFK Jr
“Cause Unknown” by Ed Dowd
Wondering how well these numbers correlate to the states with the most vaccinated