Waking up with achy joints or feeling a sudden twinge in your knees when climbing stairs often feels like a standard part of getting older. You might brush off these early warning signs, attributing them to an intense weekend gardening session or an awkward sleeping position. However, there is a distinct line between everyday muscular soreness and the onset of clinical joint disease. Recognizing that line allows you to protect your mobility and maintain your quality of life. Knowing when to see a doctor for arthritis requires paying close attention to the frequency, intensity, and specific characteristics of your discomfort. Rather than accepting pain as an inevitable reality of aging, you can learn to interpret the signals your body sends and take proactive steps toward medical intervention.
The landscape of joint health encompasses more than one hundred different conditions, ranging from mechanical wear-and-tear known as osteoarthritis to systemic autoimmune diseases like rheumatoid arthritis and psoriatic arthritis. Because each type requires a drastically different approach to care, early detection plays a pivotal role in preventing irreversible joint damage. Delaying medical consultation often allows inflammatory processes to silently erode cartilage and bone. To help you differentiate between harmless aches and serious red flags, you should carefully evaluate your physical experiences against several clinical benchmarks. If you notice any of the following seven warning signs, scheduling a comprehensive evaluation with a healthcare professional becomes a necessary priority.
Recognizing the 7 Critical Warning Signs
1. Persistent Joint Pain That Disrupts Daily Life
Occasional soreness after a long walk perfectly illustrates how a normal body reacts to exertion. Persistent pain that lingers for weeks, however, tells an entirely different story. When pain stubbornly refuses to subside despite rest, ice, or over-the-counter pain relievers, your body is signaling a structural or inflammatory issue within the joint capsule. You might find that tasks you previously accomplished with ease—such as opening a tight jar, bending down to tie your shoes, or gripping a steering wheel—now require immense effort and trigger sharp, stabbing sensations. This level of functional interference serves as a massive joint pain warning. Ignoring discomfort that disrupts your fundamental daily activities forces you to subconsciously alter your movement patterns, which often leads to secondary muscle strains and throws your body out of its natural alignment.
2. Morning Stiffness Lasting Longer Than an Hour
While taking a few minutes to loosen up in the morning happens to nearly everyone, profound stiffness that anchors you to your bed constitutes a classic clinical marker. If you frequently spend an hour or more struggling to bend your fingers or straighten your legs after waking up, you are likely experiencing specific rheumatoid signs. During the night, inflammatory fluids and proteins known as cytokines pool within the inactive joint spaces. Movement normally acts as a mechanical pump to clear these fluids, but a diseased joint lacks the efficiency to do so quickly. Prolonged morning stiffness strongly suggests an underlying autoimmune process rather than simple mechanical wear. Documenting exactly how long it takes for your joints to feel flexible each morning provides your physician with incredibly valuable diagnostic data.
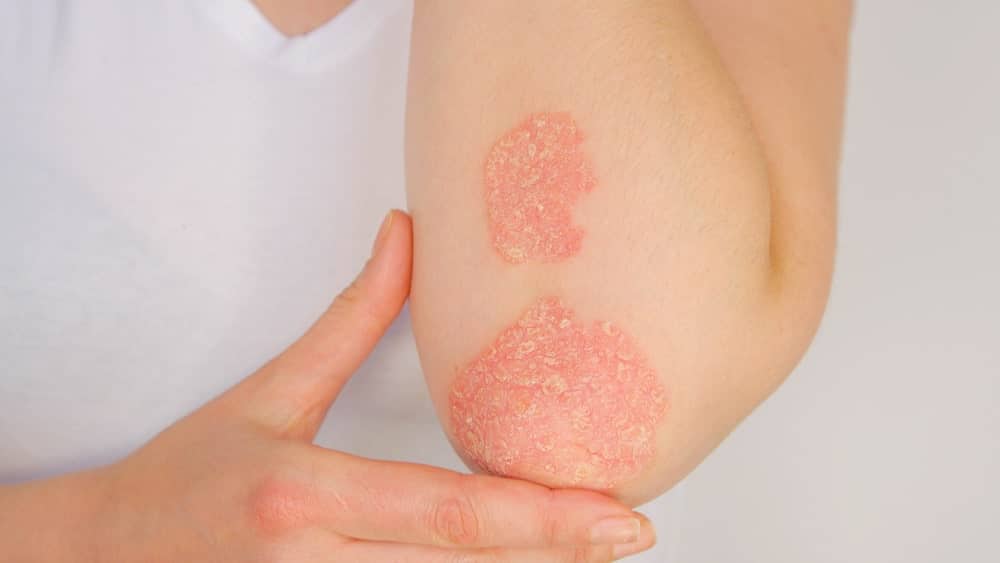
3. Noticeable Swelling and Redness Around a Joint
Healthy joints appear relatively defined, with visible contours of the surrounding bones and tendons. When a joint suddenly looks puffy, swollen, or loses its natural shape, you are witnessing active inflammation at work. The synovial membrane—the delicate tissue lining the inside of your joint—can become irritated and produce excess fluid in a frantic attempt to protect the area. This physiological response leads to visible swelling, often accompanied by a distinct sensation of warmth and a reddish flush on the overlying skin. These visual and tactile changes occur frequently in inflammatory arthritis and gout. You should never ignore a joint that feels hot to the touch; this symptom demands prompt medical evaluation to rule out severe acute inflammation or even a joint infection, which can destroy cartilage rapidly if left unchecked.
4. Joint Symptoms Accompanied by a Fever or Fatigue
Many people falsely assume that arthritis strictly affects the bones and cartilage. In reality, systemic autoimmune conditions compromise your entire body. If your joint pain arrives alongside an unexplained low-grade fever, a general sense of malaise, or sudden weight loss, your immune system is likely misfiring on a global scale. Furthermore, extreme, unexplainable fatigue often serves as one of the earliest and most debilitating symptoms of rheumatoid arthritis and lupus. This is not the standard tiredness you feel after a poor night of sleep; it is a profound, heavy exhaustion that feels akin to having a severe case of the flu. When your body diverts massive amounts of energy to sustain a chronic inflammatory response, your daily energy reserves deplete rapidly. Experiencing joint pain alongside these flu-like symptoms requires an immediate investigation by a rheumatologist.
5. A Grinding Sensation Combined With Limited Range of Motion
The ends of your bones feature a smooth, slippery coating of cartilage that allows for frictionless movement. As this cartilage degrades—a hallmark of osteoarthritis—the protective barrier thins out, leaving rough bone surfaces to rub directly against one another. You might begin to hear or feel a distinct popping, clicking, or grating sensation known medically as crepitus. While a random painless pop in your knee carries little clinical significance, crepitus accompanied by pain and a noticeable reduction in your range of motion indicates substantial joint deterioration. You may notice that you can no longer fully extend your arm or bend your knee past a certain angle. This progressive locking and grinding signals that the mechanical integrity of your joint has been compromised, making medical imaging crucial for assessing the extent of the damage.
6. Pain That Wakes You Up During the Night
Experiencing pain while actively using a joint makes logical sense. Experiencing severe throbbing that jolts you awake from a deep sleep points to a highly active disease process. Nighttime joint pain happens because your natural cortisol levels—which possess anti-inflammatory properties—drop during sleep, allowing inflammation to spike unchecked. Additionally, without the distractions of daily life, your brain processes pain signals much more acutely in the quiet of the night. Sleep deprivation creates a brutal feedback loop; lack of sleep increases your sensitivity to pain, and the increased pain further destroys your sleep quality. If you find yourself repeatedly waking up to massage a throbbing hip or shoulder, your condition has bypassed mild early stages and requires aggressive professional management.
7. Symmetrical Pain Appearing on Both Sides of Your Body
The geographic distribution of your pain offers a powerful clue regarding its origin. Osteoarthritis typically presents asymmetrically; you might have a deteriorating right knee from an old sports injury while your left knee remains perfectly healthy. Conversely, autoimmune conditions like rheumatoid arthritis demonstrate a striking symmetry. If the knuckles on your left hand begin to swell and ache, and the exact same knuckles on your right hand follow suit shortly after, you are witnessing a systemic immune attack. This mirrored pattern occurs because the autoantibodies circulating through your bloodstream target specific tissues uniformly across your body. Identifying this bilateral symmetry helps doctors narrow down the vast list of potential diagnoses and jumpstart appropriate targeted therapies.
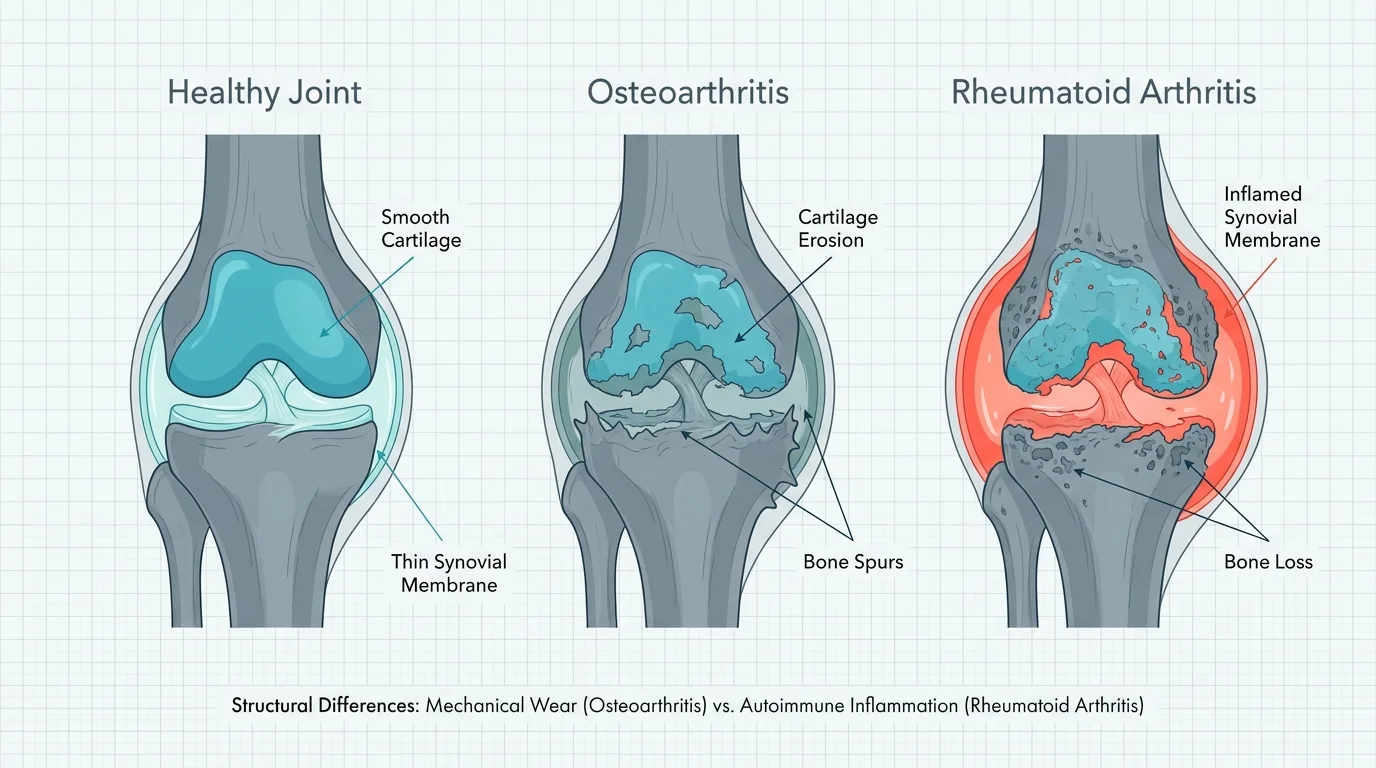
Understanding the Condition: Causes, Risk Factors, and Diagnosis
To effectively combat joint disease, you must understand the underlying mechanisms driving your symptoms. Osteoarthritis, the most prevalent form, develops when the protective cartilage capping the ends of bones gradually wears away over decades of use. This leads to the classic bone-on-bone friction that causes deep, aching pain. Autoimmune types, such as rheumatoid and psoriatic arthritis, operate differently. In these scenarios, a confused immune system mistakenly identifies the healthy synovial lining of the joints as a dangerous foreign invader and launches a relentless biological attack against it. The resulting inflammation thickens the synovium and eventually destroys the cartilage and bone within the joint capsule.
Your risk of developing these conditions depends on an intricate mix of uncontrollable and modifiable factors. Advancing age represents a primary risk factor, particularly regarding systemic inflammation 60+ demographics experience as cellular repair mechanisms slow down. Genetics also hold significant weight; possessing specific human leukocyte antigen genes dramatically increases your susceptibility to autoimmune arthritis. Previous joint traumas, repetitive occupational stress, and smoking further elevate your risk profile. Additionally, carrying excess body weight places immense mechanical pressure on weight-bearing joints like hips and knees while simultaneously releasing inflammatory proteins from fat tissues directly into your bloodstream. For a comprehensive breakdown of lifestyle risks, you can consult the detailed resources provided by the Centers for Disease Control and Prevention, which track public health data concerning joint mobility.
When you present your symptoms to a physician, the diagnostic process begins with a meticulous physical examination and a review of your medical history. Your doctor will carefully palpate your joints, checking for warmth, swelling, and precise points of tenderness. To confirm a diagnosis, they will likely order a panel of blood tests to search for specific biomarkers. Elevated levels of C-reactive protein or a high erythrocyte sedimentation rate confirm the presence of active systemic inflammation. The detection of rheumatoid factor or anti-cyclic citrullinated peptide antibodies strongly points toward rheumatoid arthritis. Imaging studies serve as the final piece of the puzzle. Standard X-rays reveal joint space narrowing and bone spurs, while advanced modalities like magnetic resonance imaging or musculoskeletal ultrasound detect early soft tissue inflammation and cartilage changes long before bone damage becomes visible.
The Treatment Landscape: Conventional, Lifestyle, and Emerging Therapies
Receiving an arthritis diagnosis initiates a strategic, multi-tiered treatment plan designed to halt disease progression, minimize pain, and preserve your joint function. The conventional medical approach heavily depends on the specific type of arthritis you face. For mechanical osteoarthritis, initial pharmacological therapy often involves nonsteroidal anti-inflammatory drugs to manage acute flare-ups, supplemented by intra-articular corticosteroid injections that deliver powerful relief directly into the affected joint. For autoimmune arthritis, the strategy requires disease-modifying antirheumatic drugs. These medications do not merely mask pain; they fundamentally suppress the overactive immune pathways causing the damage. The American College of Rheumatology regularly updates clinical guidelines to help physicians deploy these powerful medications safely and effectively.
Beyond traditional pills, the introduction of biologic therapies has revolutionized the treatment of severe inflammatory arthritis. Biologics are complex, genetically engineered proteins designed to target highly specific immune system signals, such as tumor necrosis factor or interleukins. By intercepting these specific inflammatory messengers, biologics can induce deep clinical remission in patients who previously faced guaranteed disability. However, because these therapies suppress portions of your immune system, your care team will monitor you closely for potential infections. Emerging treatments, including targeted synthetic JAK inhibitors, offer similar precision in a convenient oral pill format. Researchers funded by the National Institute of Arthritis and Musculoskeletal and Skin Diseases continue to investigate cutting-edge regenerative therapies, such as stem cell injections and platelet-rich plasma, aiming to actually rebuild lost cartilage rather than just stopping its destruction.
Medical interventions achieve their highest success rates when paired with aggressive lifestyle modifications. Physical therapy stands as a non-negotiable cornerstone of treatment. A skilled physical therapist will design a customized exercise regimen that strengthens the specific muscles supporting your vulnerable joints, effectively acting as an internal shock-absorption system. Cardiovascular exercise, particularly low-impact activities like swimming or cycling, improves blood flow to joint tissues and helps maintain a healthy weight. Dietary choices also exert a massive influence over systemic inflammation. Adopting a Mediterranean-style diet rich in omega-3 fatty acids, fresh vegetables, and whole grains while eliminating refined sugars and ultra-processed foods can measurably lower the inflammatory markers circulating in your blood.

Living With Arthritis: Self-Management and Collaborative Care
Thriving with a chronic joint condition requires shifting your mindset from passive patient to active self-manager. Pacing your daily activities prevents you from overtaxing your joints on days when you feel energetic, which helps avoid severe pain flare-ups the following day. Utilizing adaptive equipment—such as ergonomic kitchen utensils, button hooks, and shower chairs—dramatically reduces the mechanical stress placed on your small joints during routine tasks. Heat therapy effectively relaxes stiff muscles and promotes blood flow before activity, while cold packs numb sharp pain and constrict blood vessels to reduce swelling after exertion.
You do not have to navigate this journey in isolation. Building a robust, collaborative healthcare team ensures you receive comprehensive support. A rheumatologist guides your overarching medical strategy, but your team should also include physical therapists for mobility, occupational therapists for daily living adaptations, and perhaps a mental health professional to help process the profound emotional toll that accompanies chronic pain. Furthermore, connecting with local or online patient support networks through organizations like the Arthritis Foundation provides invaluable peer support. Sharing strategies and frustrations with individuals who truly understand your daily physical challenges offers a unique sense of validation and community strength.
Frequently Asked Questions
How long should I wait before seeking an evaluation for my joint pain?
You should absolutely schedule a medical evaluation if your joint pain, swelling, or stiffness persists daily for more than two to three weeks. Do not wait for the pain to become unbearable. Early intervention, particularly within the first few months of symptom onset, offers the best possible chance to prevent permanent joint deformity and secure long-term remission.
What exactly should I expect during my first rheumatology appointment?
Your first visit will be highly detailed and investigative. The specialist will ask extensive questions about your personal and family medical history, the exact timeline of your symptoms, and what makes the pain better or worse. Expect a thorough physical examination where the doctor presses on various joints to assess tenderness and swelling. They will likely draw blood for specialized autoantibody testing and send you for baseline X-rays to establish a starting point for your joint health.
Does Medicare or private insurance cover advanced biologic treatments?
Yes, most major insurance plans and Medicare provide coverage for biologic therapies, but the approval process is rigorous. Insurance companies typically require a step-therapy approach, meaning you must first demonstrate that older, less expensive medications have failed to control your disease adequately. Your rheumatology team employs dedicated staff who specialize in navigating these complex prior authorization processes to secure the medications you need.
Are there new research developments for managing arthritis symptoms in seniors?
Scientific research moves at a rapid pace, yielding highly encouraging results. Current clinical trials focus heavily on personalized medicine, aiming to use genetic profiling to predict exactly which medication will work best for your specific biology, eliminating the frustrating trial-and-error process. Additionally, researchers are making significant strides in developing sophisticated wearable devices that monitor joint inflammation in real-time, allowing doctors to adjust medication dosages precisely when a flare-up begins.
Moving Forward With Confidence
Experiencing the onset of joint disease can feel intensely overwhelming, but recognizing the early warning signs empowers you to alter the trajectory of your health. You possess the agency to advocate for your body and demand answers when persistent pain disrupts your daily routines. By partnering closely with a dedicated medical team, adopting evidence-based lifestyle changes, and utilizing modern therapeutic advancements, you can effectively manage inflammation and protect your mobility. Do not allow untreated pain to dictate your future. Reach out to your primary care provider today to discuss your symptoms, request appropriate specialist referrals, and take the definitive first step toward reclaiming your active, vibrant life.








might as well get used to the pain, the meds doctors give you may work for a short time, then they change to another and same results,
and now you have art pain and med pain for the price and physical therapy another price