
The Holistic Heart: Beyond the Lab Report
You sit across from your doctor, listening as they read off a string of acronyms and numbers—LDL, HDL, triglycerides—while your mind races ahead to a future of restrictive diets and medications. Your clinical report might feel like a final verdict on your health, but true wellbeing after sixty looks completely different. It resembles a vibrant morning walk with friends, a restful night of deep sleep, and the steady energy to pursue your lifelong passions without fear holding you back. Your cholesterol numbers do not dictate a sentence of deprivation; rather, they serve as a dynamic dashboard illuminating how your interconnected physical, emotional, and social systems function together.
When you cross into your sixties, your metabolism shifts, and the way your body processes lipids changes alongside it. However, treating cholesterol as a purely mathematical problem ignores the beautiful complexity of human biology. High levels of low-density lipoprotein or dipping levels of high-density lipoprotein are merely signals. These signals ask you to look closer at your daily routines, your stress load, and the quality of your relationships. By reframing these laboratory results as an invitation rather than a warning, you can design a lifestyle that aligns your body, mind, and community for long-term resilience.
Foundations of Physical Resilience: Decoding Your Body
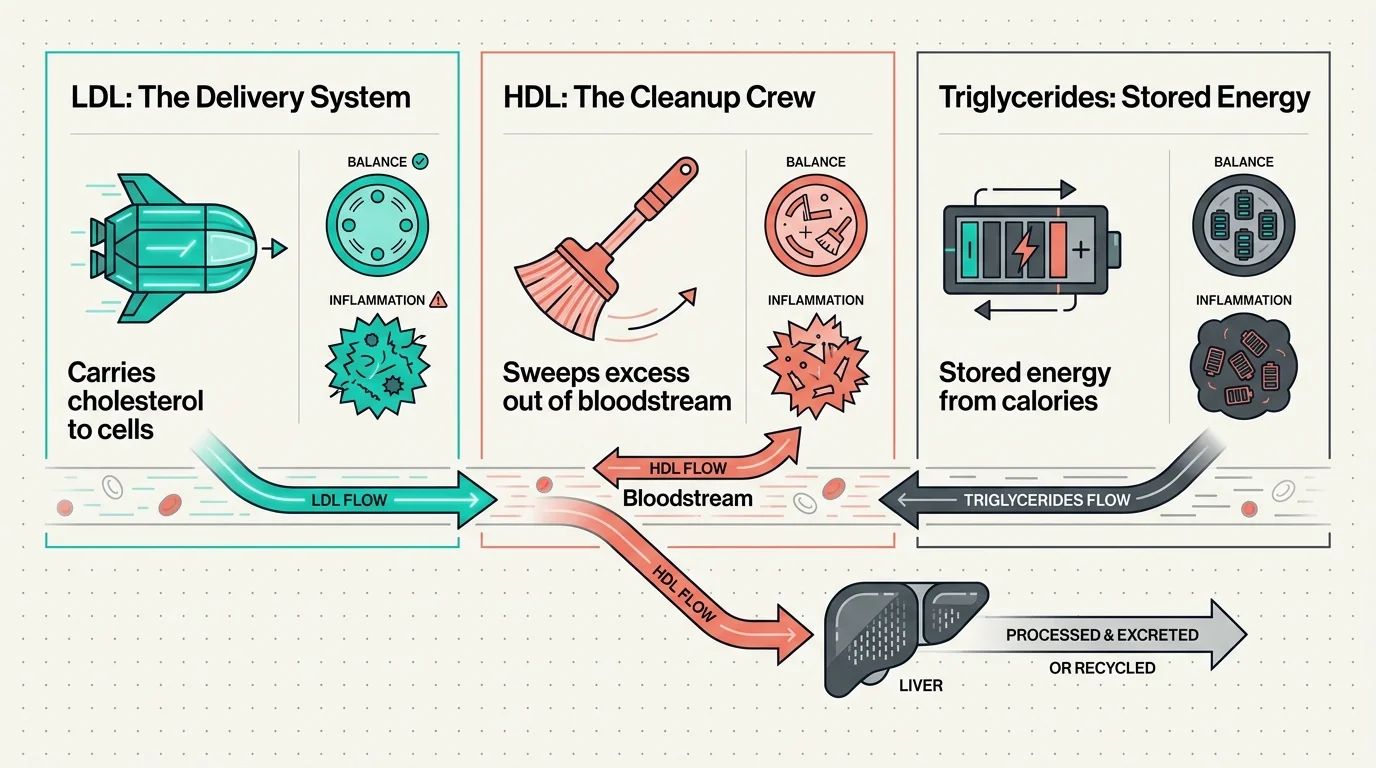
To master your cardiovascular health, you must first understand the specific roles these lipids play without getting lost in medical jargon. Low-density lipoprotein acts as a delivery system, carrying essential cholesterol to your cells for hormone production and cellular repair. High-density lipoprotein functions as the cleanup crew, sweeping excess cholesterol out of your bloodstream and returning it to your liver. Triglycerides represent stored energy from the calories you consume but do not immediately burn. When these elements fall out of balance, they point toward systemic inflammation and metabolic stress. Addressing this balance requires a unified approach to nutrition, movement, and recovery.
Nourishing Your Body for Lipid Balance
Dietary adjustments frequently trigger feelings of restriction, yet managing your lipids effectively requires adding protective foods rather than simply subtracting your favorites. Soluble fiber serves as one of your most powerful allies because it binds to cholesterol in your digestive tract and carries it out of your body before it enters your bloodstream. Tossing a handful of walnuts into your morning oatmeal, adding a half-cup of black beans to your lunch, or snacking on an apple provides the essential fiber necessary to regulate your lipid profile. These small, intentional additions transform your meals into therapeutic tools.
Furthermore, swapping saturated fats for polyunsaturated and monounsaturated fats actively improves your cellular health. Drizzling olive oil over roasted vegetables or eating fatty fish like salmon twice a week supplies your body with omega-3 fatty acids, which profoundly lower triglyceride levels and reduce arterial inflammation. You do not need to adhere to an impossibly strict regimen; you only need to make consistent, nutrient-dense choices that signal safety and abundance to your metabolic system.
Movement as Metabolic Medicine
Physical activity does far more than burn calories; it fundamentally alters how your body processes fats. Regular, moderate movement acts as a direct catalyst for increasing your high-density lipoprotein, giving your body a more robust cleanup crew to clear out arterial plaque. You do not have to run marathons to harvest these benefits. Engaging in thirty minutes of brisk walking, swimming, or cycling most days of the week significantly enhances your cardiovascular endurance and metabolic flexibility.
Strength training also plays a non-negotiable role in healthy aging and lipid management. Muscle tissue consumes vast amounts of glucose, and maintaining adequate muscle mass prevents the insulin resistance that frequently drives up triglyceride levels. Lifting light weights, using resistance bands, or practicing bodyweight exercises like modified squats and wall push-ups twice a week preserves your muscle density. This physical foundation keeps your metabolism firing efficiently, directly supporting a healthier lipid panel.
The Sleep and Stress Connection
You cannot out-eat or out-exercise the damaging effects of chronic exhaustion. Sleep deprivation acts as a massive stressor on your body, disrupting the delicate hormonal balance that dictates how your liver produces and manages cholesterol. When you consistently sleep fewer than seven hours a night, your body increases its production of ghrelin—the hunger hormone—driving you toward sugary, heavily processed foods that spike your triglycerides. Prioritizing a cool, dark sleeping environment and establishing a winding-down routine directly protects your heart.
Stress management operates right alongside sleep as a critical pillar of physical resilience. When you experience chronic stress, your adrenal glands flood your system with cortisol. This ancient survival mechanism forces your liver to pump extra glucose and cholesterol into your blood to provide energy to fight or flee. Unfortunately, modern stressors rarely require a physical escape. Extensive data published by the World Health Organization highlights that unmanaged psychological stress significantly elevates the risk of cardiovascular events, proving that calming your nervous system is just as crucial as watching your diet.

Emotional Health and Your Mind
Your psychological state dramatically influences your physiological reality. The way you process emotions, confront challenges, and view your aging process actively alters your internal chemistry. Chronic anger, anxiety, and depressive symptoms promote systemic inflammation, which accelerates the oxidation of low-density lipoprotein. Oxidized cholesterol is far more likely to stick to your arterial walls, making your emotional hygiene a literal matter of life and death.
Cultivating a resilient mindset serves as an invisible shield for your heart. Research emerging from positive psychology research centers demonstrates that older adults who maintain a high level of optimism and a strong sense of purpose exhibit significantly healthier lipid profiles and lower rates of cardiovascular disease. You can build this emotional resilience through daily mindfulness practices, such as spending ten minutes in quiet meditation, writing in a gratitude journal, or simply sitting in nature. These practices dial down your sympathetic nervous system, lowering cortisol and protecting your blood vessels from inflammatory damage.

Community Engagement and Relationships
Human beings are profoundly social creatures, and our cardiovascular systems reflect our level of connection. Loneliness and social isolation trigger the same biological alarm bells as physical threats, elevating blood pressure and disrupting lipid metabolism. Comprehensive reports from the American Psychological Association indicate that deep, meaningful relationships buffer the physical impacts of stress, effectively lowering systemic inflammation and supporting healthy cholesterol levels.
Investing in your social health requires intentional action. Joining a local walking group, volunteering for a cause you care about, or simply scheduling weekly phone calls with distant family members strengthens your social safety net. When you engage in joyful, shared activities, your brain releases oxytocin. This powerful hormone naturally dilates your blood vessels, lowers your blood pressure, and reduces the oxidative stress that damages your heart. Your community is an active component of your cardiovascular treatment plan.
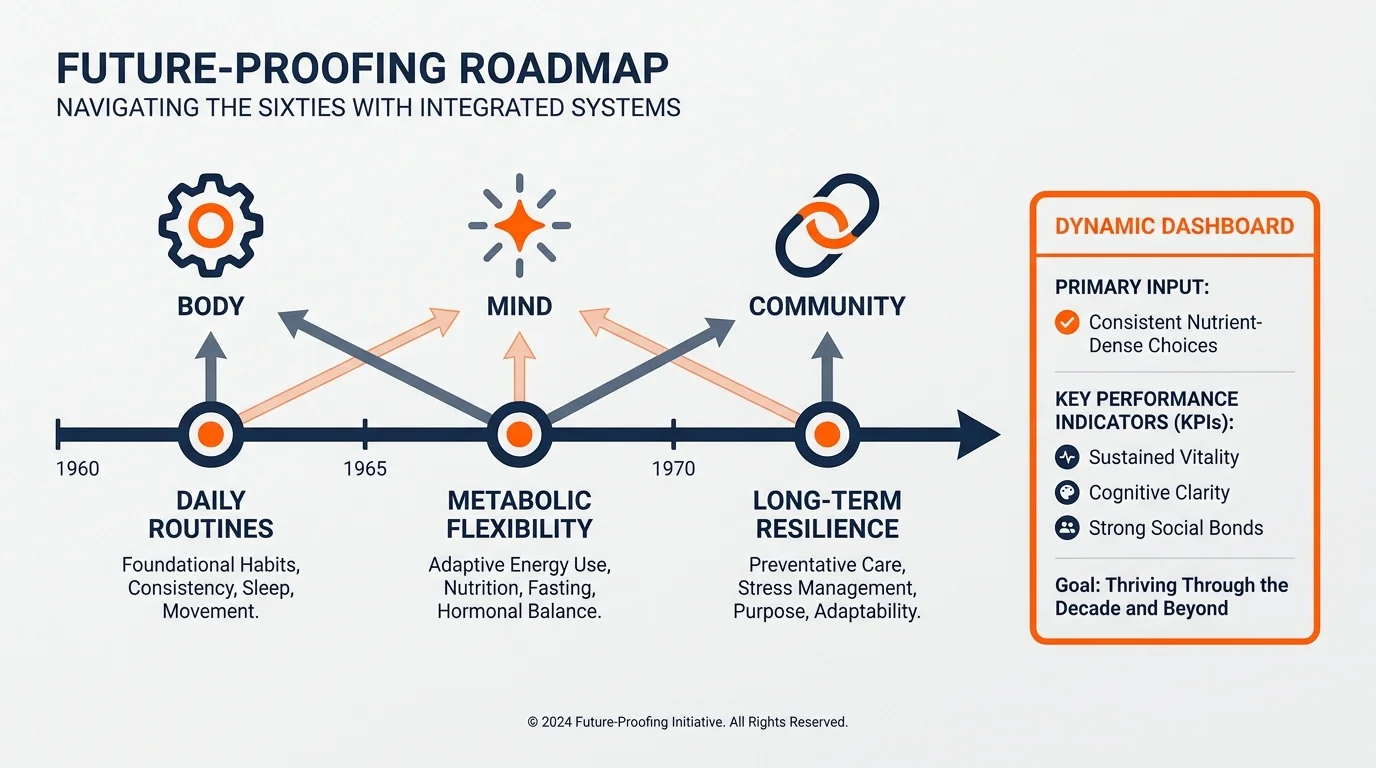
Future-Proofing Your Wellbeing and Planning Ahead
Sustainable health transformations do not happen through massive, overnight overhauls; they happen through the strategic application of habit stacking. Habit stacking involves pairing a new, desired behavior with a routine you already perform effortlessly. For instance, if you brew a pot of coffee every morning, use those five minutes to perform a series of gentle stretches or a brief breathing exercise. If you listen to a favorite podcast in the afternoon, tie that listening time to a twenty-minute neighborhood walk. By anchoring new habits to existing ones, you bypass the need for endless willpower.
Preventive care and proactive tracking also keep you in the driver’s seat of your aging journey. Rather than waiting for your annual physical to think about your health, monitor your vitality through daily subjective measures. Notice how easily you climb a flight of stairs, track the quality of your sleep, and pay attention to your energy crashes after meals. These subtle clues often reveal more about your metabolic health than a single fasting blood draw. When you actively participate in gathering this data, you become a collaborative partner with your healthcare team rather than a passive recipient of medical advice.
Exploring comprehensive lifestyle interventions can also dramatically alter your trajectory. Many progressive clinics now focus on the root causes of metabolic dysfunction rather than just managing symptoms with pharmaceuticals. Exploring resources like the American College of Lifestyle Medicine can connect you with practitioners who integrate nutrition, sleep science, and behavioral health into a unified cardiovascular strategy, ensuring your future remains vibrant and unhindered.
Frequently Asked Questions About Managing Heart Health
What should you do when your cholesterol numbers go up despite your best efforts?
First, practice self-compassion and avoid viewing a temporary increase as a personal failure. Human biology fluctuates due to a variety of factors, including recent periods of high stress, minor infections, thyroid changes, or even poor sleep leading up to the test. Instead of aggressively restricting your diet, review your recent lifestyle patterns holistically. Have you been managing a stressful life transition? Has a minor injury reduced your daily step count? Discuss these contextual factors with your physician, and consider asking for a more detailed lipid fraction test, which measures the actual particle size of your cholesterol, providing a much clearer picture of your actual cardiovascular risk than a standard panel.
How can you improve cardiovascular health if mobility issues limit your physical activity?
Cardiovascular conditioning does not require high-impact exercise. If joint pain or mobility restrictions prevent you from walking long distances, you can engage your heart through seated exercises, water aerobics, or recumbent cycling. Aquatic therapy is particularly effective because the buoyancy of the water removes the strain on your hips and knees while providing excellent cardiovascular resistance. Additionally, upper body ergometers or seated shadow boxing elevate your heart rate and stimulate your metabolism. Focus on whatever movement feels joyful and accessible, knowing that any sustained elevation in your heart rate provides profound metabolic benefits to your lipid profile.
How do you prioritize heart-healthy habits when caregiving or other duties consume your time?
When your schedule feels completely overwhelmed by the demands of caring for others, you must reframe self-care as a non-negotiable requirement for your caregiving capacity. You cannot pour from an empty vessel. Start by finding micro-moments for health. You do not need a full hour to exercise; three ten-minute bursts of brisk walking throughout the day provide the exact same cardiovascular benefits as a continuous thirty-minute session. Keep unsalted nuts, fresh fruit, and pre-cut vegetables easily accessible so that when exhaustion hits, your default snacks actively support your lipid balance. Most importantly, ruthlessly protect your sleep window, as a well-rested brain handles caregiving stress far more efficiently.
When should you seek professional support beyond a primary care physician to manage heart-related stress?
You should consider engaging a mental health professional or a specialized health coach when anxiety about your medical numbers begins interfering with your daily joy. If you find yourself obsessively worrying about every bite of food, experiencing panic regarding your future, or isolating yourself because social events involve unpredictable meals, it is time to seek psychological support. A therapist specializing in health anxiety or a certified lifestyle medicine coach can help you dismantle catastrophic thinking. They provide evidence-based coping strategies that allow you to manage your cardiovascular risk from a place of empowerment rather than a place of chronic fear.
Creating Your Wellbeing Check-In Ritual
Transforming your approach to heart health requires consistent reflection. Establish a weekly wellbeing check-in ritual to honor the incredible work your body does for you every day. Set aside ten minutes each Sunday morning, pour a cup of herbal tea, and gently review your week. Ask yourself how well you managed your stress, whether you fueled your body with nourishing foods, and how connected you felt to your community. This quiet reflection removes the anxiety of perfectionism and replaces it with compassionate curiosity.
As you move forward, remember to celebrate your small, daily wins. Acknowledge the victory of choosing water over a sugary beverage, the triumph of completing a restorative walk, and the deep value of calling an old friend. Your cholesterol numbers will inevitably fluctuate, but the vibrant, multifaceted life you build around them remains entirely in your control. By aligning your physical actions, your emotional resilience, and your social bonds, you secure not just a healthier heart, but a profoundly rich and lasting vitality.








Leave a Reply