You spend hours tossing and turning, watching the illuminated numbers on your clock slowly tick toward morning. Perhaps you wake up gasping for air in the middle of the night, or you simply feel completely drained of energy despite spending eight to nine hours in bed. Countless older adults dismiss these frustrating, restless nights as an inevitable and normal part of the aging process. However, chronic sleep disruptions signal much more than a mere nighttime inconvenience; they act as a hidden catalyst for severe cardiovascular disease. The relationship between how effectively you rest and how well your heart functions represents a critical, often overlooked area of senior health.
When you consistently fail to achieve deep, restorative sleep, your cardiovascular system bears the brunt of the physiological damage. Ignoring chronic exhaustion places immense, unnecessary stress on your heart muscle and your blood vessels. As your sleep architecture changes with age, you become more vulnerable to conditions that fragment your rest and elevate your blood pressure. By understanding the profound connection between sleep health and cardiovascular risk, you can take immediate and proactive steps to protect your heart, reduce your risk of serious medical events, and reclaim your daily vitality.
Understanding the Condition: The Biology of Sleep and Cardiovascular Risk
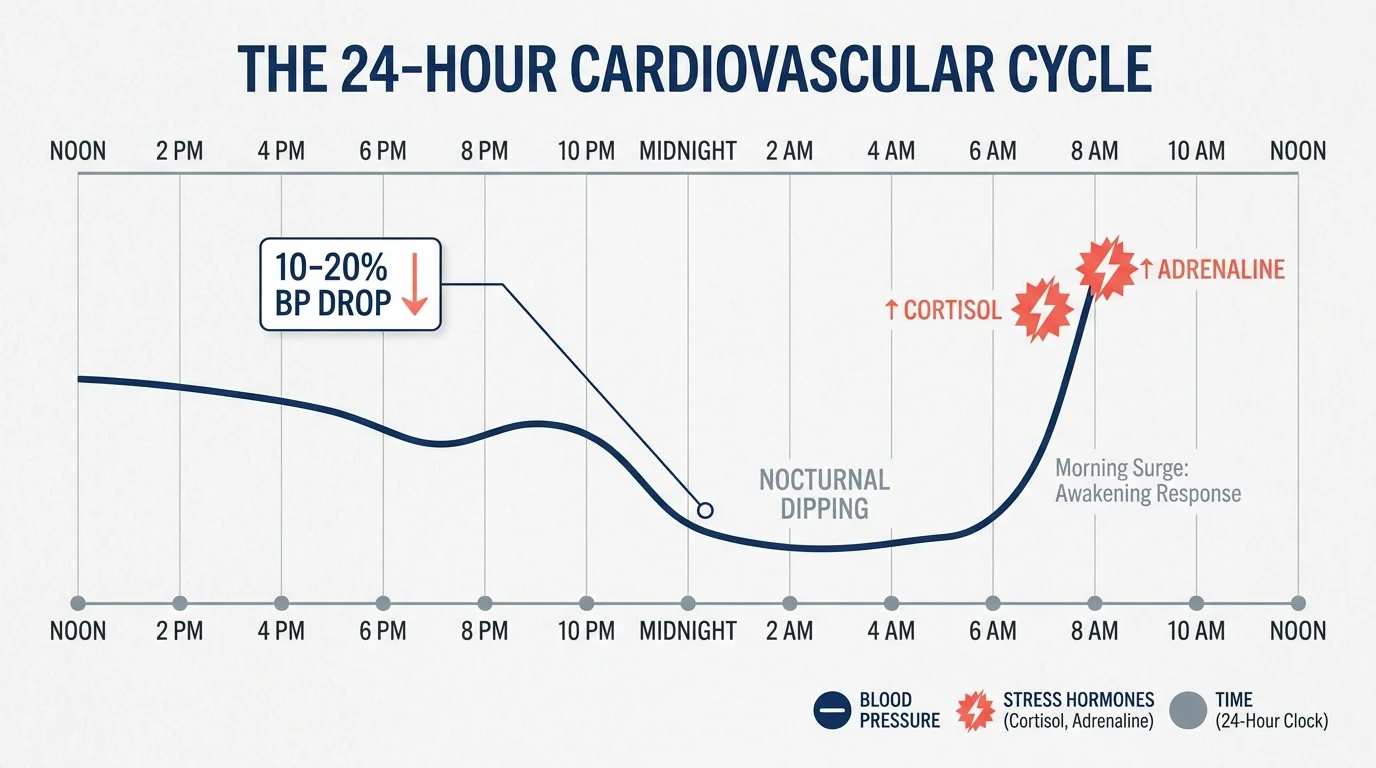
To grasp why poor sleep harms your heart, you must first understand what happens to your body when you rest properly. During healthy, uninterrupted sleep, your heart rate slows down and your blood pressure naturally drops by about ten to twenty percent. Cardiologists refer to this essential resting period as nocturnal dipping. This nightly dip gives your entire cardiovascular system a much-needed break from the strenuous demands of waking life. It allows your blood vessels to relax, repair microscopic damage, and clear out metabolic waste products.
When sleep disruptions occur—whether due to severe insomnia, frequent trips to the bathroom, or sleep-disordered breathing—you lose this vital protective drop in blood pressure. Your body instead remains in a relentless state of high alert. Each time you wake up or experience a micro-arousal that pulls you out of deep sleep, your sympathetic nervous system kicks into high gear. This sudden fight-or-flight response triggers the rapid release of stress hormones, including cortisol and adrenaline. These potent chemicals cause your blood vessels to constrict and your heart rate to accelerate, creating dangerous spikes in your cardiovascular workload while you lie in bed.
Over time, this chronic nighttime stress damages the delicate inner lining of your blood vessels, an issue known as endothelial dysfunction. When your blood vessels cannot expand and contract properly, you face a significantly higher risk of developing systemic inflammation and arterial plaque buildup. The American Heart Association recognizes poor sleep as a primary, modifiable risk factor for resistant high blood pressure, stroke, and heart failure in older adults. If your blood pressure remains elevated throughout the night, you effectively experience the wear and tear of a stressful day for twenty-four uninterrupted hours.
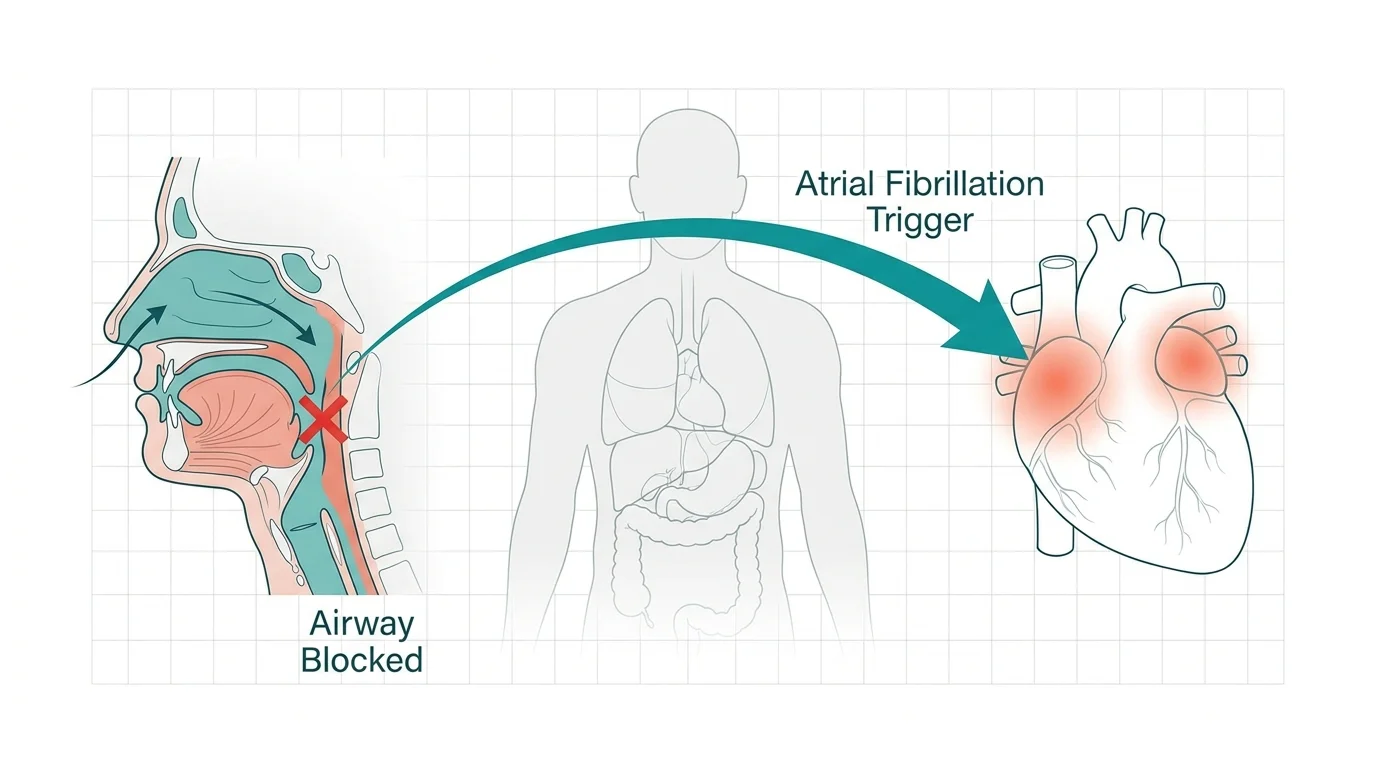
Obstructive sleep apnea stands out as the most severe and direct threat to cardiovascular health in seniors. When the muscles in the back of your throat relax too much during sleep, they physically block your airway and halt your breathing. Your blood oxygen levels immediately plummet. In response, your brain panics and jolts you awake just enough to take a gasping breath. This violent cycle can repeat dozens of times per hour. The physical effort of trying to breathe against a closed airway creates an immense vacuum effect in your chest, stretching the walls of your heart. This stretching acts as a major trigger for atrial fibrillation, a dangerous irregular heart rhythm that dramatically increases your risk of suffering a stroke.

Diagnosing the Problem: How Medical Professionals Evaluate Your Risk
Diagnosing the complex intersection of sleep fragmentation and heart disease requires a thorough and methodical approach. Your healthcare provider will not simply hand you a prescription for a sleeping pill and send you on your way. Instead, they will investigate the root biological causes of your sleep disruptions and carefully assess your current cardiovascular baseline. The diagnostic journey often begins with a detailed conversation about your daily habits, your level of daytime fatigue, and your specific nighttime symptoms. You should always prepare for this appointment by keeping a sleep diary for two weeks, noting your exact bedtimes, wake times, caffeine consumption, and how often you get up during the night.
Your doctor will also ask you to complete standardized questionnaires, such as the Epworth Sleepiness Scale, to measure how likely you are to doze off during routine daytime activities. Because seniors often live alone or sleep in separate beds from their partners, you might not realize how loudly you snore or how often you stop breathing. If you do have a bed partner or an overnight caregiver, ask them to attend the appointment with you; their firsthand observations regarding your breathing patterns provide invaluable clues to your medical team.
To definitively identify sleep-disordered breathing, your physician will order a polysomnogram, widely known as a sleep study. Traditionally, this required spending the night in a specialized sleep center while technicians monitored your brain waves, blood oxygen levels, heart rate, and chest movements. Today, many seniors qualify for home sleep apnea testing. These highly advanced, portable devices allow you to sleep comfortably in your own bed while recording essential respiratory and cardiac data. The convenience of home testing makes it much easier for older adults to get an accurate diagnosis without the anxiety of sleeping in a clinical laboratory.
Because the link between sleep and heart rhythms is so strong, your evaluation might also overlap with cardiology testing. If your doctor suspects that oxygen deprivation has already triggered abnormal heartbeats, they might ask you to wear a Holter monitor. This wearable electrocardiogram continuously tracks your heart’s electrical activity over twenty-four to forty-eight hours. By analyzing this data alongside your sleep patterns, your doctors can determine if episodes of atrial fibrillation or sudden heart rate spikes are directly coinciding with your nighttime breathing pauses.
The Treatment Landscape: Protecting Your Heart While You Rest
Treating sleep disorders in older adults requires careful navigation to improve rest without compromising patient safety. Conventional treatments focus on rapidly restoring normal breathing, stabilizing the autonomic nervous system, and lowering nighttime blood pressure. For older patients diagnosed with moderate to severe obstructive sleep apnea, Continuous Positive Airway Pressure, or CPAP therapy, remains the absolute gold standard of care. A CPAP machine delivers a gentle, steady stream of pressurized air through a fitted mask, acting as a pneumatic splint that keeps your airway completely open throughout the night.
By effectively preventing nighttime oxygen drops, CPAP therapy directly lowers your blood pressure and sharply reduces the physical strain on your heart muscle. Although adjusting to wearing a mask takes patience and persistence, the cardiovascular benefits are profound and immediate. If you struggle with the traditional face mask, respiratory therapists can offer alternative styles, such as lightweight nasal pillows, to improve your comfort. For seniors who simply cannot tolerate CPAP therapy, specialized dentists can craft custom oral appliances. These mandibular advancement devices gently shift your lower jaw forward during sleep to maintain an open airway, offering a viable alternative for protecting your heart.
When chronic insomnia drives your sleep deprivation and elevates your resting heart rate, the medical community strongly advises against relying on pharmaceutical interventions. Instead, sleep specialists advocate for Cognitive Behavioral Therapy for Insomnia, frequently referred to as CBT-I. This structured program helps you identify and change the anxious thoughts and disruptive behaviors that keep you awake. CBT-I utilizes techniques like sleep restriction and stimulus control to retrain your brain to associate your bed strictly with deep sleep. Extensive research from organizations like the National Sleep Foundation consistently shows that behavioral interventions provide safer, longer-lasting relief from insomnia than any prescription medication.
If your care team does consider medication, they will proceed with extreme caution. Prescription sleeping pills, including benzodiazepines and Z-drugs, carry severe risks for older adults. Aging kidneys and livers process medications much more slowly, meaning a sleeping pill taken at midnight can leave you heavily sedated and dizzy the following morning. This next-day sedation dramatically increases your risk of suffering a catastrophic fall. Furthermore, chemical sedatives depress your central nervous system, which can dangerously worsen unrecognized sleep apnea by relaxing your throat muscles even further.
Your physician will also review your current cardiovascular medications to ensure they are not inadvertently ruining your rest. Certain beta-blockers can cause vivid, disturbing nightmares that fracture your sleep cycle. Similarly, taking a diuretic water pill too late in the evening guarantees you will wake up multiple times to use the bathroom. By strategically adjusting the timing of your daily medications, your doctor can minimize nighttime interference while keeping your heart condition perfectly managed.

Living With Poor Sleep and Heart Disease Risks: Strategies for Seniors and Caregivers
Managing the complex relationship between sleep quality and cardiovascular risk extends far beyond the doctor’s office. You must actively cultivate a daily routine that supports your biological clock and promotes restorative rest. Your daily habits completely dictate your nightly success. Start by firmly anchoring your circadian rhythm with bright morning sunlight. Exposing your eyes to natural daylight within an hour of waking helps regulate your brain’s melatonin production, sending a clear biological signal about when to be alert and when to feel sleepy.
Daily physical activity serves as a highly effective, natural sleep aid that simultaneously strengthens your heart. Engaging in a brisk morning walk, joining an afternoon water aerobics class, or practicing gentle yoga can significantly deepen your slow-wave sleep. However, you must avoid vigorous cardiovascular exercise within three hours of your bedtime, as the lingering adrenaline and elevated body temperature can make falling asleep incredibly difficult. You should also strategically manage your fluid intake; stop drinking large amounts of water or herbal tea at least three hours before bed to minimize the sleep-shattering effects of frequent nighttime urination.
You must optimize your bedroom environment to support healthy sleep architecture. As you age, your core body temperature fluctuates differently, making you much more sensitive to environmental heat and cold. To achieve deep sleep, your core temperature actually needs to drop slightly. Keep your bedroom cool—ideally around sixty-five degrees Fahrenheit if tolerable—and ensure the space remains pitch dark and completely quiet. Consider investing in breathable, moisture-wicking sleepwear and layered bedding so you can easily adjust your temperature without fully waking up.
Caregivers play an indispensable role in managing these interconnected conditions. If you care for an older adult, you act as the crucial first line of defense in identifying dangerous sleep disorders. Pay close attention to their daytime behavior. Excessive afternoon napping, sudden mood changes, irritability, or newly emerging memory problems often stem from severe nighttime oxygen deprivation rather than normal cognitive decline. Caregivers also provide vital assistance with the complex logistics of sleep apnea therapy. Cleaning CPAP equipment, replacing air filters, and ensuring the mask fits without leaking can easily overwhelm an exhausted patient. By helping manage these practical tasks and utilizing resources from the American Academy of Sleep Medicine, caregivers ensure their loved ones receive the full cardiovascular benefit of the prescribed treatment.
Frequently Asked Questions
What are the immediate warning signs that my sleep issues are affecting my heart?
You should immediately alert your doctor if you frequently wake up with a racing, pounding heart or feel a strange fluttering sensation in your chest during the night. Waking up with severe shortness of breath, particularly when lying flat, serves as a major red flag for cardiovascular strain. Additionally, if you experience chronic morning headaches or notice unusual swelling in your legs and ankles, your heart may be struggling against the low oxygen levels caused by untreated sleep apnea. These symptoms require urgent medical evaluation to prevent irreversible heart damage.
How often should I follow up with my doctor if I have both sleep apnea and high blood pressure?
Once you begin treatment for a sleep disorder, you should expect to see your sleep specialist and your cardiologist quite frequently during the first few months. Initially, you will likely have a follow-up appointment within four to six weeks to review your CPAP compliance data and ensure the mask fits properly. Afterward, you should schedule comprehensive reviews every three to six months. As your sleep quality improves and your nighttime oxygen levels stabilize, your blood pressure will likely drop. Your doctor will need to closely monitor these changes and may actually need to safely reduce your hypertension medications to prevent your blood pressure from dipping too low during the day.
Does Medicare or private insurance cover sleep studies and CPAP machines for seniors?
Yes, Medicare Part B and the vast majority of private insurance plans provide robust coverage for both facility-based polysomnography and home sleep apnea tests, provided your physician orders them based on clinical symptoms. If you receive an official diagnosis of obstructive sleep apnea, Medicare typically covers a three-month initial trial of CPAP therapy. However, you must prove that you use the machine consistently to maintain this coverage. Insurance guidelines generally define strict compliance as using the device for at least four hours a night on seventy percent of nights. If you meet this threshold, insurance will continue paying for the machine and your necessary replacement supplies.
What does the latest research say about treating sleep disorders to reverse heart damage?
Recent cardiovascular research, supported by data from the National Institute on Aging, demonstrates that strictly adhering to sleep apnea therapy can actually reverse specific structural changes in the heart. Clinical studies indicate that long-term CPAP use successfully reduces the unhealthy thickness of the heart wall and vastly improves the heart’s overall pumping efficiency. Furthermore, effectively treating chronic insomnia actively lowers systemic inflammation markers, such as C-reactive protein, which plays a critical role in halting the progression of coronary artery disease. Addressing your sleep disorder does not merely stop further damage; it actively helps heal your cardiovascular system.
Moving Forward With Confidence
Facing the reality of cardiovascular disease risks combined with chronic sleep struggles can certainly feel overwhelming, but you absolutely hold the power to change your health trajectory. Your sleep quality directly dictates your cardiovascular resilience. By acknowledging that poor rest is not just a harmless consequence of getting older, you take the first and most crucial step toward achieving better health. You no longer have to accept waking up exhausted and straining your heart in the process.
Share your nighttime symptoms with your primary care physician and confidently request a thorough sleep evaluation. Lean on your caregivers, your medical team, and patient advocacy groups to help you successfully navigate the transition to treatments like CPAP therapy or cognitive behavioral therapy. With the right diagnostic tools and a commitment to maintaining rigorous sleep hygiene, you can protect your blood vessels, stabilize your blood pressure, and dramatically lower your risk of heart arrhythmias. You deserve to wake up each morning feeling fully refreshed, knowing your heart remains strong, well-rested, and completely ready for the day ahead.






Leave a Reply