Ignoring certain nighttime symptoms can silently accelerate chronic disease and compromise your longevity. While occasional sleep disruptions happen, specific overnight warning signs like persistent night sweats, shortness of breath, or severe leg cramps require immediate medical evaluation. Paying attention to what your body communicates in the dark empowers you to catch underlying conditions early, from cardiovascular issues to endocrine imbalances. Restorative sleep serves as your biological repair cycle; when unusual physical sensations repeatedly interrupt this process, your body signals a deeper vulnerability. Recognizing these eight crucial symptoms helps you protect your long-term wellness, allowing you to seek timely professional care and transform anxious, fragmented nights back into a foundation for sustainable health.
The Science of Sleep Disturbances and Systemic Health
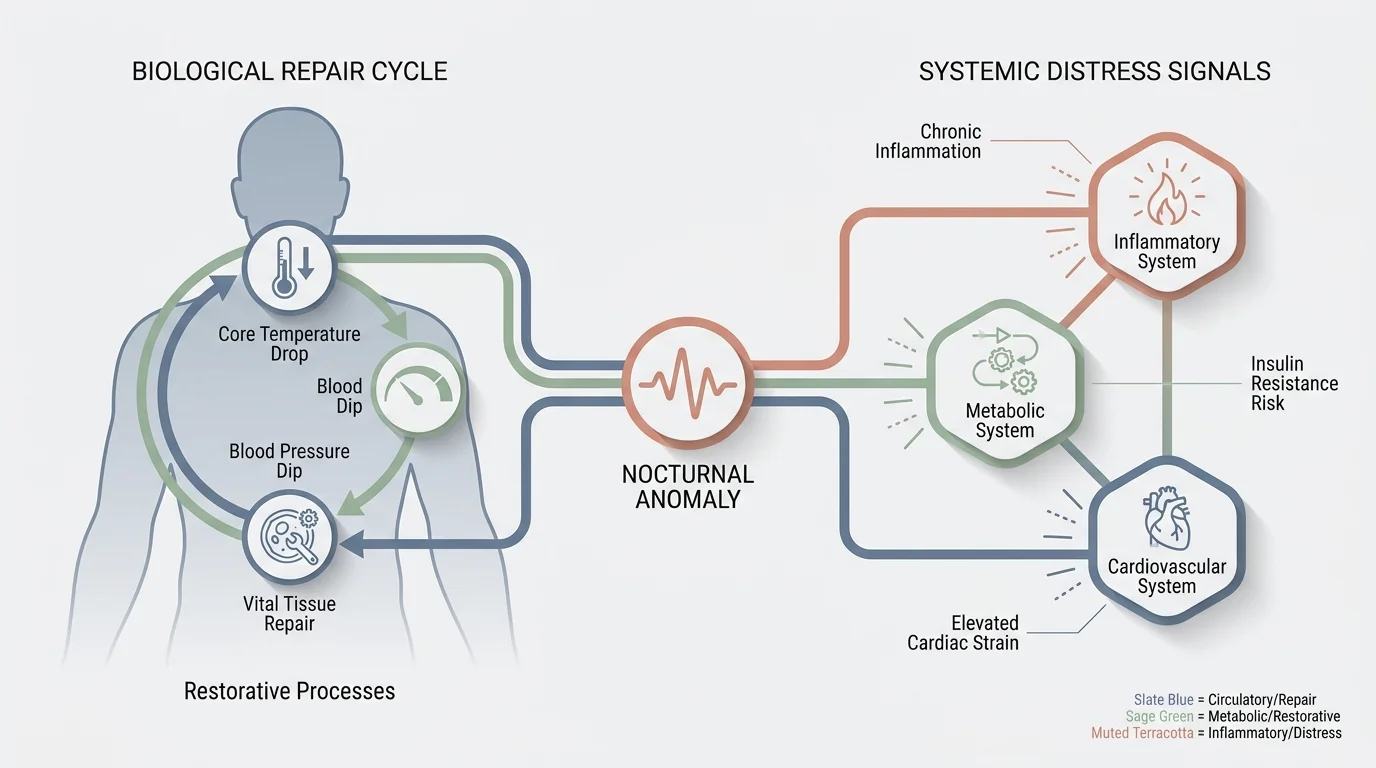
Your body undergoes profound physiological changes when you sleep. Core body temperature drops, blood pressure naturally dips, and vital tissue repair systems activate. When a persistent symptom interrupts this delicate biological orchestration, it often points to a systemic imbalance rather than a simple environmental nuisance. Researchers and medical professionals understand that sleep serves as a critical diagnostic window; the absence of daytime physical exertion and mental distractions allows underlying inflammatory, metabolic, or cardiovascular distress signals to become undeniable. Acknowledging these nighttime anomalies early enables you to leverage modern medicine and lifestyle interventions effectively. You do not have to endure fragmented rest as an inevitable consequence of aging, stress, or a demanding lifestyle. By identifying the physiological root causes of these nocturnal disruptions, you empower yourself to improve your daily vitality and secure your long-term health trajectory. Consulting evidence-based resources from the National Institutes of Health can provide foundational context for how sleep disturbances correlate with broader disease risk factors.

Evaluating Overnight Warning Signs

1. Unexplained and Drenching Night Sweats
Drenching night sweats go far beyond feeling slightly warm under heavy blankets or sleeping in a poorly ventilated room. If you frequently wake up needing to change your pajamas or bed sheets, your body is signaling a significant thermoregulatory disruption. While menopausal transitions represent a common and manageable cause for many individuals, severe nocturnal sweating can also indicate hidden bacterial infections, thyroid dysfunction, or even certain malignancies like lymphoma. Your endocrine system relies on a stable physiological environment to regulate hormones; when it misfires repeatedly at night, a clinical evaluation helps you identify the exact trigger. Document the frequency of these episodes and note any accompanying daytime symptoms, such as unexplained weight loss or persistent fatigue, to provide your healthcare provider with a comprehensive diagnostic picture.

2. Shortness of Breath or Waking Up Gasping
Waking up abruptly with a choking sensation or feeling completely out of breath is a terrifying experience that demands prompt medical attention. This sudden oxygen deprivation often points to obstructive sleep apnea, a condition where the airway collapses during deep sleep, severely stressing your cardiovascular system. Beyond sleep apnea, nocturnal shortness of breath can also serve as an early indicator of congestive heart failure or undiagnosed asthma. When your heart struggles to pump fluid efficiently, that fluid can back up into your lungs when you lie flat, making breathing exceedingly difficult. Guidance from the National Heart, Lung, and Blood Institute emphasizes that addressing these breathing interruptions can dramatically reduce your risk of high blood pressure and sudden cardiac events.

3. Severe Leg Cramps and Muscle Spasms
A sudden, agonizing cramp in your calf or foot can jolt you out of the deepest stages of sleep. While an isolated cramp might simply result from intense daytime physical activity or minor dehydration, chronic nighttime muscle spasms suggest more complex underlying issues. Frequent cramping often highlights critical electrolyte imbalances, particularly deficiencies in magnesium, potassium, or calcium. In more serious scenarios, persistent nocturnal leg pain indicates peripheral artery disease—a condition where narrowed blood vessels reduce blood flow to your limbs. Paying attention to exactly when the cramps occur and whether they improve with gentle stretching or walking helps your doctor differentiate between a simple nutritional deficit and a concerning vascular blockage.
4. Persistent Snoring Accompanied by Morning Fatigue
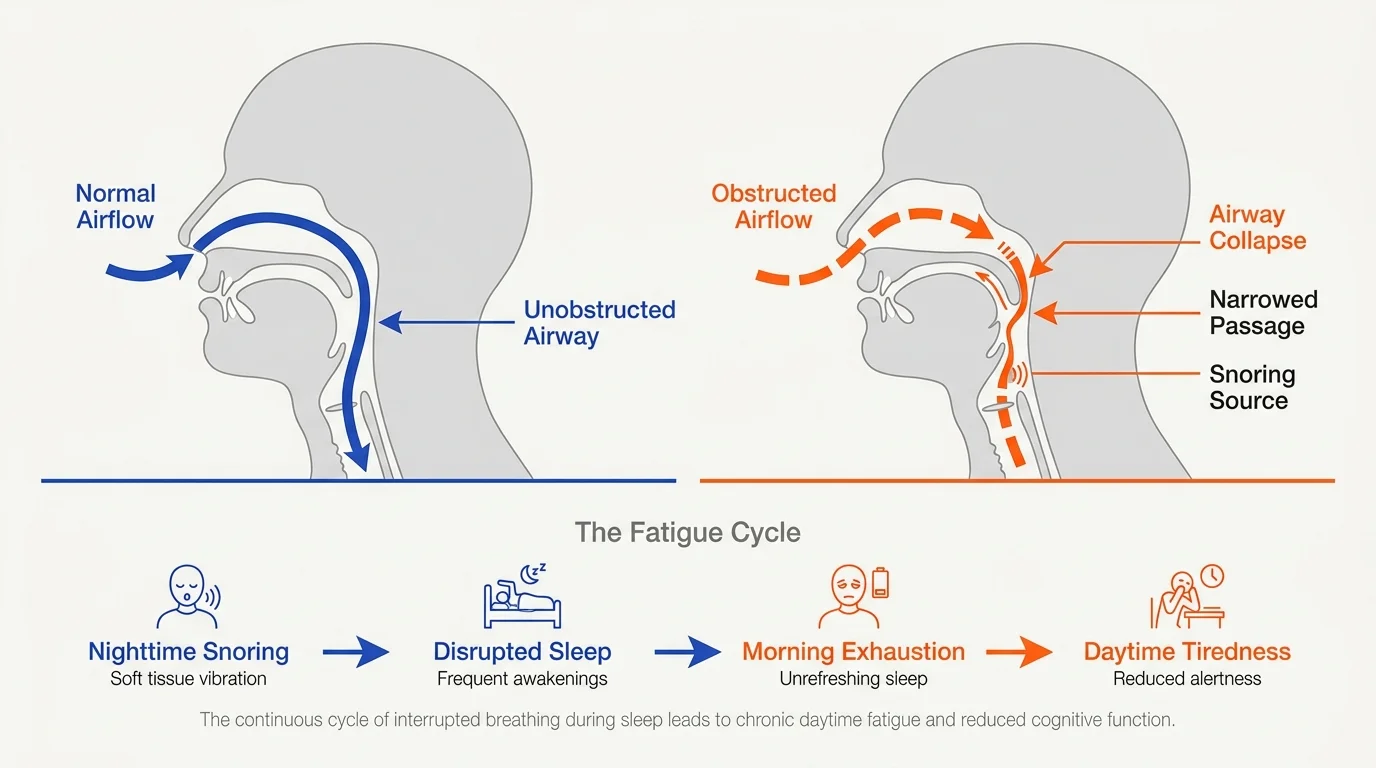
Snoring is frequently dismissed as a harmless annoyance for sleeping partners, but loud, persistent snoring paired with unrefreshing sleep requires a closer look. The vibration of soft tissues in your throat indicates restricted airflow, which forces your heart and lungs to work significantly harder throughout the night. If you sleep for eight hours but still wake up feeling completely drained, battling morning headaches, or struggling with intense brain fog, your brain is likely suffering from chronic overnight oxygen deprivation. Addressing severe snoring involves more than buying specialized pillows; it requires a structural and physiological assessment to protect your cognitive function and long-term metabolic health.

5. Frequent Urination Interrupting Sleep
Frequent trips to the bathroom during the night disrupt your sleep architecture and leave you exhausted the next day. Medical professionals refer to this condition as nocturia. While reducing evening fluid intake seems like an obvious and practical fix, persistent nocturia often points to underlying health conditions rather than a simple hydration issue. Your kidneys might be processing excess blood sugar, a classic early warning sign of type 2 diabetes. Alternatively, shifting prostate health, pelvic floor prolapse, or the side effects of certain blood pressure medications can drive this symptom. The National Institute of Diabetes and Digestive and Kidney Diseases strongly recommends evaluating persistent nocturia to rule out progressive kidney or metabolic disorders.

6. Chest Pain or Unusual Pressure
You should never ignore chest pain, tightness, or pressure, regardless of what time it occurs. While nighttime chest discomfort might occasionally stem from severe acid reflux or a strained pectoral muscle, it remains a primary warning sign of a cardiac event. Angina, which is chest pain caused by reduced blood flow to the heart muscles, can strike while you are resting in bed. If the pressure radiates to your jaw, neck, back, or left arm, or if it is accompanied by cold sweats and nausea, treat it as an absolute medical emergency. According to guidelines provided by the Centers for Disease Control and Prevention, recognizing and acting upon these cardiac symptoms rapidly is the most effective way to prevent irreversible heart damage.

7. Heart Palpitations and Racing Pulse
Laying quietly in the dark only to feel your heart pounding, fluttering, or racing against your ribs is profoundly unsettling. Nighttime heart palpitations frequently result from late-day caffeine consumption, alcohol intake, or acute anxiety, but they also serve as key indicators of electrical issues within the heart. Conditions like atrial fibrillation or hyperthyroidism can cause your heart rate to spike unpredictably during sleep. Because your resting heart rate should naturally decrease overnight, a violently racing pulse indicates an inappropriate surge of adrenaline, cortisol, or thyroid hormones. Tracking the exact duration of the palpitations and discussing them with a cardiologist ensures you receive appropriate screening for potentially dangerous arrhythmias.
8. Sudden Joint Pain or Swelling
Waking up with stiff, swollen, or intensely painful joints is not simply an unavoidable part of getting older. While osteoarthritis often feels worse after a long day of movement, inflammatory joint conditions tend to flare up dramatically during the night or first thing in the morning. Your body’s natural production of cortisol—a potent anti-inflammatory hormone—drops to its lowest levels overnight, allowing conditions like rheumatoid arthritis or gout to provoke severe pain. Repeatedly waking up due to joint pain accelerates joint degradation and compromises your overall mobility. The World Health Organization notes that early intervention in inflammatory arthritis is critical for preserving joint function and preventing irreversible structural damage.

Strategy Pillars: Managing Your Health Beyond the Mattress

Nutrition: Fueling for Restorative Slumber
What you consume in the hours leading up to bedtime dictates your metabolic stability throughout the night. To combat symptoms like palpitations, acid reflux, and night sweats, you must stabilize your blood sugar by avoiding heavy, carbohydrate-dense meals and refined sugars late in the evening. Instead, focus on small, nutrient-dense snacks rich in complex carbohydrates and lean proteins if you feel hungry before bed. Furthermore, eliminating alcohol and caffeine at least four to six hours before sleeping drastically reduces the likelihood of heart racing and thermoregulation issues. Proper daytime hydration prevents severe muscle cramping, but you must taper your fluid intake two hours before sleep to minimize disruptive bathroom trips.

Movement: Gentle Physical Activity for Symptom Relief
Strategic physical activity during the day profoundly influences how your body rests at night. If you struggle with leg cramps or restless legs, incorporating gentle stretching routines focused on your calves and hamstrings right before bed provides immediate mechanical relief. For individuals experiencing nocturnal shortness of breath or early-stage vascular issues, maintaining a consistent daily walking habit improves overall circulation and venous return. However, avoid high-intensity cardiovascular workouts within three hours of bedtime, as the resulting spikes in cortisol and core body temperature can easily trigger night sweats and restless, fragmented sleep. Movement should serve as a tool to release tension, not a catalyst for overstimulation.

Mindset: Calming Nighttime Anxiety
The psychological toll of experiencing disruptive physical symptoms in the dark often creates a vicious cycle of anxiety and insomnia. When you worry about waking up gasping for air or suffering a muscle cramp, your nervous system remains in a hyper-vigilant state, preventing deep, restorative sleep. Establishing a structured wind-down routine helps signal to your brain that it is safe to relax. Engage in grounding practices such as diaphragmatic breathing, progressive muscle relaxation, or journaling to offload daytime stress. It is crucial, however, to separate manageable sleep anxiety from genuine physical distress; mindfulness techniques will not cure a physiological airway obstruction, but they will help you remain calm while you seek appropriate medical solutions.
Medical Care: Partnering with Professionals
Symptom management requires a collaborative approach with qualified healthcare providers. Self-diagnosing based on internet searches often leads to unnecessary panic or dangerous delays in receiving critical care. Recognize that social determinants, such as demanding work schedules and limited access to healthcare facilities, make prioritizing medical appointments difficult. Despite these barriers, you must advocate for your health by scheduling comprehensive blood panels, cardiovascular screenings, or specialized sleep studies. Bring a detailed log of your symptoms to your appointments, noting the time of onset, duration, and severity. This concrete data empowers your clinician to bypass guesswork and order the precise diagnostic tests needed to uncover the root cause of your nighttime distress.

Voices from the Clinical Frontlines
Physicians who specialize in sleep medicine continually observe how easily patients normalize their nocturnal suffering. Many clinicians express frustration that individuals endure years of drenching sweats, chronic pain, or severe snoring simply because they assume these are inevitable signs of aging or stress. Patients who finally undergo sleep studies or comprehensive blood work frequently report a profound sense of relief when they receive an accurate diagnosis. Discovering that a racing heart stems from an easily manageable thyroid imbalance, or that morning exhaustion is entirely resolved by using a CPAP machine, transforms their quality of life. The clinical consensus is clear: your body speaks loudest when the world is quiet. Listening to those overnight signals, rather than enduring them in silence, is the most profound act of self-care you can undertake.
Frequently Asked Questions About Nighttime Symptoms
When do night sweats become a serious medical concern?
Night sweats require medical evaluation when they happen consistently for more than two weeks, force you to change your sleepwear, or occur alongside unexplained weight loss, chronic coughing, or persistent daytime fatigue. While minor sweating due to a heavy blanket is normal, drenching sweats that disrupt your rest indicate that your body is fighting an underlying systemic issue. A physician will typically check your thyroid hormone levels, screen for localized infections, and evaluate your broader endocrine function to determine the exact cause.
Can daily stress and anxiety cause shortness of breath while I am sleeping?
Yes, severe anxiety and panic attacks can absolutely wake you up with a feeling of breathlessness or a racing heart. However, you should never assume shortness of breath is just anxiety without first ruling out physical causes. Because sleep apnea, asthma, and congestive heart failure present with identical nocturnal breathing issues, you must undergo a clinical assessment. Once a doctor confirms your heart and lungs are physically healthy, you can safely focus on stress reduction and targeted anxiety management therapies.
How do I know if my frequent urination requires a doctor visit?
If you are waking up more than once per night to urinate and you have already restricted your evening fluid intake, it is time to schedule a medical consultation. This is especially true if you also experience increased thirst, painful urination, or a weak urine stream. Your healthcare provider can quickly test your fasting blood sugar to rule out diabetes, check for urinary tract infections, and assess your kidney function, allowing you to treat the root cause rather than just enduring the exhaustion of broken sleep.
Will changing my diet really help with nighttime heart palpitations?
Dietary modifications offer surprisingly effective relief for many people experiencing benign nighttime palpitations. Heavy evening meals often trigger severe acid reflux, which can stimulate the vagus nerve and cause your heart to flutter or race. Additionally, hidden caffeine in late-day teas, chocolates, or certain medications acts as a potent stimulant. By shifting your largest meal to earlier in the day and strictly monitoring your evening stimulant intake, you can dramatically reduce digestion-related heart racing. If the palpitations persist despite these changes, a cardiological workup is mandatory.
Your Next Manageable Step
Transforming your sleep health does not require you to overhaul your entire life overnight. Start with a single, highly practical action: keep a notebook on your bedside table tonight. For the next seven days, briefly jot down any physical symptoms that wake you up, noting the approximate time and how you feel in the morning. This simple symptom log costs nothing, takes only seconds to complete, and provides invaluable, concrete data for your next doctor’s appointment. Take a moment today to reflect on your current baseline—are you settling for fragmented, anxious rest when your body is actually asking for medical support? Honoring your body’s overnight warning signs is your first proactive step toward reclaiming the deep, restorative sleep you deserve.











Leave a Reply